We present a review of imaging features and role of imaging and radiologist in the diagnostic pathway of these unusual tumours.
For the purpose of this review,
we will focus on unusual masses in the mediastinum and chest wall/pleura. Some of the following are reviewed in this pictorial review.
1.
Mediastinal Lesions: (1) Dermoids and teratomas; (2) Duplication Cysts; (3) Unusual thymic tumours (4) Tracheal tumours (5) Non-neural posterior mediastinal masses
2.
Benign and malignant pleural/chest wall tumours including sarcomas and bone lesions.
We will also explore the role of further imaging such as PET-CT and MRI where appropriate and present a brief review of literature.
A list of interesting case for this pictorial review is as follows.
Case 1:
78 years old female presented with dysphagia and chest pain symptoms gradually getting worse.
Known multiple myeloma.
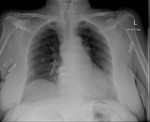
CXR (Fig 1) - Widening of superior mediastinum.
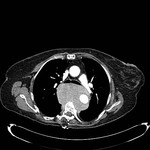
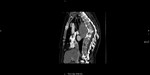
CT (Fig 2 and 3): Large posterior meditational mass with wedge fractures of thoracic vertebral bodies.
Diagnosis: Provisional diagnosis was of lymphoma or small cell cancer but endoscopic trans oesophageal biopsy demonstrated plasma cells,
hence in keeping with mediastinal plasmacytoma .
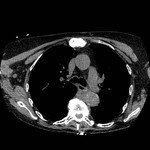
Follow up imaging after 9 months (Fig 4) demonstrated complete resolution of mass.


Fig. 1: Widening of superior mediastinum


Fig. 2: Posterior meditational mass

Fig. 3: Wedge fractures of thoracic vertebral bodies

Fig. 4: Post Treatment Scan
Radiology Pearls:
- Most common site for extramedullary involvement is the upper aerodigestive tract (4%)
- Only 5% of patients with extramedullary plasmacytoma have coexistent multiple myeloma
- Biopsy is usually required to establish diagnosis as difficult to differentiate from lung cancer
- Recurrence can be up to 30% case in 10 years period.
Case 2:
45 years old male referred by general practitioner for left sided chest pain.
CXR and CT : Large anterior mediastinal mass (Fig 5,
6 and 7)
PET CT: Diffuse increased tracer activity in the anterior mediastinal mass.
(Fig 8)
CT Guided Biopsy: Thymic Neuroendocrine tumour.

Fig. 5

Fig. 6: Anterior mediastinal mass

Fig. 7

Fig. 8: Diffuse increased tracer activity in the anterior mediastinal mass


Radiology Pearls:
- Tend to present as large masses as only 50% are functionally active.
- On cross sectional imaging thymic carcinoids may be indistinguishable from thymomas.
- FDG uptake on PET is variable with tendency for the uptake to be low.
Case 3:
77 years old male undergoing investigations for unexplained weight loss.
Previous history of coronary artery bypass graft 10 years ago.
Imaging findings:
Partially calcified aneurysm of coronary artery graft measuring 5cm (Fig 9 and 10)

Fig. 9: Aneurysm of coronary artery graft

Fig. 10


Radiology Pearls:
- Rare complication of CABG with estimated rate <1%
- Differentiation between true and false aneurysms not always possible.
- Up to 55% true aneurysms are asymptomatic as compared to only 15% of pseudo aneurysms.
Case 4:
40 years old female with shortness of breath.
CXR- Retrocardiac mass (Fig 11).
CT: Rounded left paravertebral soft tissue mass (Fig 12).
MRI: Low T1W and Water suppressed T2 images confirm cystic nature (Fig 13 and 14).
Surgical Excision : confirmed Bronchogenic cyst.

Fig. 11: Retrocardiac mass

Fig. 12: Left paravertebral soft tissue mass

Fig. 13: T1W

Fig. 14: T2W with fluid supression


Radiology Pearls:
- Can be mediastinal (70%) or intrapulmonary.
- Approximately 50% are fluid density (0-20Hu) but a significant number could be soft tissue density (>30HU) or even hyper dense to mediastinal soft tissue.
- Usually no contrast enhancement and MRI features typical of a cyst.
- Attempt at sampling can lead to chemical mediastinitis.
Case 5:
30 year old male with acute onset chest pain and haemodynamic instability.
CXR- Anterior mediastinal mass (Fig 15).
CT: Anterior mediastinal mass with fat and calcification with haemorrhagic pericardial effusion (Fig 16 and 17) leading to temponade effect and hence haemodynamic instability.
Surgical Excision: Teratoma.

Fig. 15: Anterior mediastinal mass

Fig. 16: Anterior mediastinal mass with fat and calcification

Fig. 17: Haemorrhagic pericardial effusion


Radiology Pearls:
- 80% anterior mediastinum and rest are usually multi compartmental.
- Variable CT appearances due to variable amount of fat.
- Calcification only up to 26% case.
- Rupture can lead to cardiac temponade.
Case 6:
63 years old female with right sided chest pain and shortness of breath.
CXR and CT – Large mass in right hemi thorax displacing the mediastinum to left side (Fig 18 and 19).
CT guided biopsy – Pleural fibroma.
Surgical excision and 6 months post excision CT (Fig 20) - No evidence of recurrence.


Fig. 18

Fig. 19: Large mass in right hemi thorax displacing the mediastinum to left side

Fig. 20: 6 months post excision CT
Radiology Pearls:
- Calcification,
rib destruction and pleural effusion are usually absent.
- Homogenous background enhancement on contrast CT.
- Low signal intensity on all MRI sequences and MRI useful to demonstrate necrosis or haemorrhage.
- Asbestos exposure is not an association.
Case 7:
36 years old male presented with right sided pleuritic chest pain.
CXR and CT scan: Right posterior mediastinal mass but no effusion (Fig 21 and 22).
PET: heterogeneous FDG uptake with a maximum SUV of 5.1 (Fig 23)
Biopsy: Pleomorphic spindle cell sarcoma.
Excised with excision of pericardium. Recurrence at 4months on follow up CT (Fig 24).


Fig. 21


Fig. 22: Right posterior mediastinal mass but no effusion

Fig. 23: Heterogeneous FDG uptake

Fig. 24: Recurrence at 4 months on follow up CT


Radiology Pearls:
- Spindle cell sarcomas of chest wall extremely rare of young to middle aged.
- Heterogeneously enhanced mass with well-defined margins,
cortical bone destruction,
tumour calcifications and tumour infiltration of the chest wall musculature.
- Mediastinal,
hilar,
diaphragmatic or axillary lymph nodes are rarely involved.
- Recurrence is common and MRI is not very useful for evaluation of early recurrence like in limbs due to artefacts.
Case 8:
55 years old female presented with persistent cough.
Background of Thalassemia.
CXR and CT - Posterior mediastinal mass (Fig 25 and 26)
Abnormal bone texture and absence of spleen (Fig 27 and 28).

Fig. 25: Posterior mediastinal mass

Fig. 26: Posterior mediastinal mass

Fig. 27: Abnormal bone texture

Fig. 28: Absence of spleen


Radiology Pearls:
- Occurs in hemoglobinopathies,
hemolytic anemias,
leukemias,
lymphomas,
and myeloproliferative disorders.
- Most common in posterior mediastinum.
- Biopsy is unnecessary and is associated with risk of haemorrhage.
Case 9:
35 years old male presented with chest pain and SOB.
CXR and CT- Posterior mediastinal mass with areas of poor enhancement on contrast CT (Fig 29 and 30).
PET CT- Heterogeneous trace activity with relatively low activity at the core (Fig 31 and 32).
Biopsy- Mediastinal synovial sarcoma.
Resection attempted but recurrence at 12 months and subsequent death.

Fig. 29

Fig. 30: Posterior mediastinal mass with areas of poor enhancement on contrast

Fig. 31: Heterogeneous trace activity with relatively low activity at the core

Fig. 32


Radiology Pearls:
- Very rare mesenchymal neoplasms that primarily affect the deep soft tissues of the extremities.
- Biopsy is needed for diagnosis due to wide range of differentials for mediastinal masses.
- PET CT useful to rule out distant metastases before surgery which is only possible route to cure.
Case 10:
60 years old male presented with chest pain and mass arising from left chest wall for 6 months.
CXR - Ill defined opacity over left hemithorax with left pleural effusion (Fig 33).
CT- Soft tissue mass which appears rather bland in left anterior chest involving both sides of the ribs with rib destruction and pleural effusion (Fig 34).
MRI- T1W with contrast (Fig 35) demonstrating nearly uniform enhancement of chest wall mass .
Biopsy - Diffuse large B Cell Lymphoma.
Started on treatment and 3 months follow up scan (Fig 36) demonstrated almost complete resolution of the left chest wall mass.

Fig. 33: Ill defined opacity over left hemithorax with left pleural effusion

Fig. 34: Chest wall mass with rib destruction

Fig. 35: MRI with Contrast

Fig. 36: 3 months follow up scan
Radiology Pearls
- Isolated chest wall lymphoma is a rare entity.
- CT and MR sensitive in the evaluating apparent extension of the mass into fat or muscle and unequivocal bone destruction
- Pericardial involvement should be carefully assessed.
- Combined chemotherapy and radiation is reported to lead to complete remission.