972 lung cancers were diagnosed in Nova Scotia in 2014. Data were available for 967 cancers in 946 patients. 98 cancers (10.1%) were detected through lung nodule CT surveillance (fig.
1). 13 cancers were detected through a lung cancer screening research project.
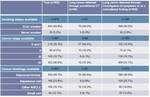
The patients who were diagnosed with lung cancer through surveillance CT were compared to those with lung cancer diagnosed either through imaging requested for evaluation of lung cancer symptoms or as a coincidental finding on imaging requested for another reason (see methods section for definitions).
There was no significant difference in patient age,
gender or smoking status.
However,
lung cancer detected through surveillance CT was much more likely to be stage I and much more likely to be adenocarcinoma.
Further data are provided in Table 1.
Of the 98 lung cancers detected through nodule surveillance programs,
18 cancers arose from nodules initially measuring less than 6mm in diameter,
33 from nodules measuring 6-8mm,
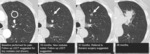
28 from nodules measuring 9-15mm and 19 though surveillance of larger equivocal opacities. Smaller nodules were more likely to be solid and larger nodules more likely to be subsolid. Examples are included in Figures 2-5.
Of the cancers detected through surveillance,
only two nodules initially measuring greater than 15 mm were solid. One was a carcinoid tumor. The second was an invasive adenocarcinoma that was not confirmed as malignant by tissue until 7 years after it was first seen. Delay occurred due to initial negative percutaneous biopsy and then due to the radiologist missing growth (comparison was made only with the most recent prior CT rather than the most remote CT).
There was a median interval of 18 months between initial CT and CT reported as high risk or conclusive for cancer (interquartile range 9 to 34 months). Longer intervals were seen for nodules initially measuring under 8mm,
for subsolid opacities,
for nodules with slow growth rates,
for nodules evaluated with thicker CT slice collimation and when the radiologist compared only to the most recent prior CT.
Of the 98 cancers detected through surveillance programs,
40 (40.8%) underwent percutaneous biopsy. Percutaneous biopsy occurred after a median of 4 surveillance CTs (interquartile range 3-5 months) and a median of 27 months (interquartile range 13-49 months). 71 (72.4%) were investigated by PET (either for diagnosis or staging).
The PET was reported as not concerning for malignancy in 25 (35.2%) of these 71 cases. Nodules with initial false negative PET and false negative biopsy were more likely to experience a longer time to initiation of treatment.
For 37 cases (37.8%),
there was a delay of at least 400 days from when the nodule was first seen by CT to when the patient was seen by a lung cancer specialist. Of these 37 cases,
17 nodules measured less than 8mm on initial CT and 7 were purely ground glass on initial CT.
9 of the 37 experienced a delay of at least 100 days before seeing a specialist after a CT reported as definitive for cancer.
LIMITATIONS: This is a retrospective analysis of nodule surveillance and not a controlled study with consistent CT technique,
nodule analysis and reporting standards. The results partially reflect radiologist behavior,
including error. It is also essential to note that only cases resulting in a diagnosis of cancer have been included.
The presumed hundreds of nodule surveillance studies not resulting in a diagnosis of cancer have not been reviewed.