Keywords:
CT, Lung, Emergency, Decision analysis, Outcomes
Authors:
N. Tsuchiya1, Y. Ohno2, Y. Nakano3, T. Yamashiro1, S. Gibo4, M. Schiebler5, S. Murayama1; 1Okinawa/JP, 2Kobe/JP, 3Shiga/JP, 4Urasoe, Okinawa/JP, 5Madison, WI/US
DOI:
10.26044/esti2019/P-0031
Methods & Materials
The institutional review board approved this retrospective,
cross-sectional study and waived informed patient consent.
From December 2001 to December 2012,
thoracic CT scans of 34 drowning patients (mean age,
41 years; range,
6-78 years; 21 males,
13 females) were evaluated (Fig 1).
A medical record review was performed to evaluate clinical severity and prognosis.
To determine the clinical severity,
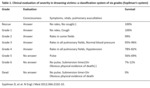
we used the Szpilman’s classification system (Table 1) (2).
Clinical severity was assessed by the medical staff (nurse or doctor) on arrival at the hospital.
Brain anoxia and death in the hospital were recorded.
Treatment outcomes were assessed as (a) hospital stay more than 1 week,
(b) need for intubation,
(c) need for antibiotics.
CT image and CXR were evaluated by experienced chest radiologists who were blinded to clinical information.
CT and CXR were separately scored by different radiologists.
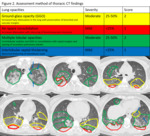
Presence and severity of the following pulmonary CT findings were assessed: ground-glass opacity (GGO: increased hazy attenuation in the lung with preservation of bronchial and vascular margins),
air-space consolidation (increased attenuation with obscuring of bronchovascular structures),
multiple lobular opacities (centrilobular nodules and GGO or consolidation with septal margins and sparing of secondary pulmonary lobules),
and interlobular septal thickening (abnormal thickening of interlobular septa).
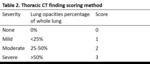
For the severity assessment of the imaging findings,
we used a visual estimate of the percentage of lung opacities using the following Likert scoring system for both lungs: none- 0 point,
mild (<25% of the whole lung area)- 1 point,
moderate (25–50%)- 2 points,
and severe (>50%)- 3 points (Table 2)(Figure 2).
The individual percentage scores for each lung were added together to yield a total consolidation score for chest X-ray.
The presence of a pleural effusion on CT were also assessed.
The mean value of severity score for each CT findings were compared between prognosis difference using Wilcoxon signed-rank test.
The presence of pleural effusion was compared using Fisher's exact test.
Univariate and multivariate logistic analysis were used for correlating the imaging findings along with the valid clinical findings to treatment outcomes.
Statistical analyses were performed by using the JMP 11 (SAS Institute Japan,
Tokyo,
Japan).
A p-value of less than 0.05 was considered as a statistically significant difference.