Keywords:
Connective tissue disorders, Treatment effects, Diagnostic procedure, CT, Lung
Authors:
M. Lacroix1, J. S. Rech2, C. DE MARGERIE-MELLON1, H. Nunes 2, Y. Uzunhan2, B. Arnulf1, P.-Y. Brillet3; 1Paris/FR, 2Bobigny /FR, 3Bobigny/FR
DOI:
10.26044/esti2019/P-0076
Imaging findings OR procedure details
The mean age at diagnosis was 62 yo (54-70) with 43 AL,
1 AA and 29 indefinite typing.
Among the 43 patients with analysed thoracic CT,
composite patterns were frequent: 35% of patients (n= 15),
including 16% proven pleura disease (=7).
There were 33% of “tracheobronchial “ (n=14),
16% of “nodular” (n=7) and also 16% of “interstitial” pattern (n=7).
“Tracheobronchial” and “nodular” patterns were more frequent in localized amyloidosis (respectively 76% and 80%) whereas “interstitial” and “composite” patterns were more frequent in systemic amyloidosis (respectively 86 and 78%).
Among the patient with “tracheo-bronchial” pattern: 25% presented a tracheal thickening,
mostly circumferential and diffuse (64%) (Figure 1).
More than half of the patients had bronchial disease,
including bronchial thickening (56%),
bronchial stenosis (34%) and bronchiectasis (37%) (Figure 2).
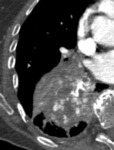
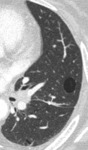
For the “nodular” pattern,
the nodules were solid,
in general multiple and characterized by their large size (mean+/-SD: 24+/-14 mm at initial diagnosis),
smooth edges (58%),
calcifications (37%) and a peripheral predominance (74%) (Figure 3 and 4).
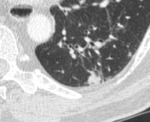
Concerning the “interstitial” pattern,
we described condensations (37%) (Figure 5),
interlobular septal thickening (23%) (Figure 6),
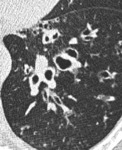
cysts (14%) (Figure 7) and ground glass (19%) (Figure 8),
with possible combination of signs (Figure 9).
After a mean follow-up of 3.14 years (3 months-11 years),
no significant regression was observed under treatment whatever the type of amyloidosis or the initial pattern.