Hospital Set-up,
CT Scanner Specifications and IT Set-up
Data for a period of two years (between January 1st 2014 and December 31st 2015) was automatically tracked with a RTS (Radimetrics,
Bayer HealthCare,
Whippany,
NJ) from seven CT scanners installed at five medical institutions located in North-western Switzerland.
There were three regional hospitals,
one private hospitals focusing on geriatric care and a university hospital.
Data from all hospitals came from one CT scanner except the university hospital (University Hospital Basel),
which has three CT scanners installed.
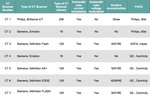
The CT scanners represented a broad range in regards to geometry (16 to 256 slice) and dose reduction capabilities (e.g.
five of seven have iterative reconstruction technique installed) (Fig. 1).
The same RTS (Radimetrics,
Bayer HealthCare) was installed at all five participating hospitals.
The RTS was connected to PACS systems from four different vendors and extracted the radiation exposure details,
stored in the Digital Imaging and Communications in Medicine (DICOM) header or Radiation Dose Structured Report.
The dose-data was then relayed to three local servers,
where it was anonymized before being uploaded to a single master server called the patient dose repository.
A dose-team was created in the university hospital,
which consisted of a radiologist,
technologist,
medical physicist and IT specialist.
The technologist from the dose-team visited the different facilities to standardize the nomenclature of all protocols and created ‘master protocols’.
The protocol standardization was performed with the help of the Radlex playbook published by RSNA (3).
This was done to link the various device protocols to a standard unified protocol and avoid comparison of ‘apples with oranges’.
The radiologist (with 11 years of experience with CT dose optimization) confirmed the matching of all device protocols with the master protocols to avoid mismatching and ensure reliable analyses of doses.
Data was collected for the five most commonly performed single phase diagnostic CT examinations in adults; head (to rule out intracerebral hemorrhage),
chest (to rule out pulmonary nodules or pneumonia),
abdomen-pelvis (e.g.
assessment of an acute abdomen),
renal-colic protocol and CT pulmonary angiogram (to rule our embolism).
The RTS provided values (mean,
median and interquartile range; IQR) for the different dose metrics- volumetric dose index (CTDIvol),
dose-length product (DLP),
size-specific dose estimate (SSDE) and effective dose (ED).
Results and Analyses
Overall,
82,580 diagnostic CT examinations were performed in adults in the two-year period.
Of these,
15,539 scans were of CT head (18.8% of all examinations),
7,343 scans were of CT thorax (8.8 % of all),
5,828 scans were for abdomen-pelvis (7% of all),
3,364 examinations for CT pulmonary-angiogram (4% of all examinations) and 2,433 examinations were for urolithiasis (3% of all scans).
The five protocols (34,507 examinations) amounted to 41.7 % of all examinations.
Inter-institutional Benchmarking
Fig. 2 enumerates the interquartile range (25th,
50th and 75th percentile) of CTDIvol (in mGy) and DLP (in mGycm) values for all five protocols by the seven CT scanners.
It reveals a wide variation in doses between the seven scanners.
The most significant difference is noted for CT thorax. Fig. 3 depicts a four-fold difference in the median value of CTDIvol for CT thorax between scanner 3 and 7,
which are the same scanners at two different institutions.
This indicates the need for protocol optimization and rigorous review of clinical workflow.
CT 2 and CT4 are also same scanners at two different institutions,
however,
in addition to 65% difference in the median doses between the two,
CT 4 also shows less variability in doses as compared to CT2.
This indicates a more harmonized and standardized dose distribution in the hospital with CT4.
National Benchmarking
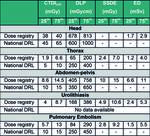
A local dose registry from the data of the two-year period was created (25th and 75th percentile values listed in Fig. 4.
Comparison of radiation doses with published national DRLs for Switzerland (published in 2010) was also carried out (4). Comparison of radiation doses with published national DRLs for Switzerland (published in 2010) was also carried out (4).
Except for CT abdomen-pelvis,
the 75th percentile DLP values for our regional registry has lower values as compared to the national DRL of Switzerland for all other protocols (4).
The greatest difference is noted for CT thorax,
where the DRL (75th percentile) values in our study is 50% lower than national DRL.
For CT head,
our study shows 18% lower values than national DRL. Fig. 5 shows the CTDIvol for CT head by the seven scanners for the two years.
All seven scanners have 75th DRL values lower than 65 mGy (the national DRL),
the largest value in our registry was 64 mGy.
While one scanner had 25th percentile CTDIvol of 45 mGy (same as published national ‘target’ 25th percentile value),
the rest of the six scanners were less than 45 mGy.
Such results indicate that the rapid advancements in dose-efficient technology (such as iterative reconstruction) and their use are rendering the previously published DRLs outdated.
There is a need to update the pre-existing registries,
especially for CT thorax.
Also,
the previously published DRL’s do not prescribe values for the new dose-metric SSDE.