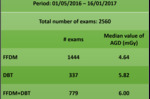
A total of 2560 breast studies (FFDM 1444,
DBT 337,
FFDM+DBT 779) were performed between May 1,
2016 and January 16,
2017 on adult female patients using the same device that provides digital 2D and 3D images of the breast (Selenia Dimensions; Hologic,
Bedford,
MA,
USA).
Once stabilized the breast,
the DBT system acquires 15 projections over a 15° angular range (from -7.5° to +7.5°).
At the central projection,
the source to detector distance is 70 cm,
with 2.5 cm air gap between the detector and the breast support plate.
When performing DBT procedures the anode/filter combination is fixed (W/Al) and the tube voltage (kVp) is automatically selected by the system based on breast thickness.
When performing FFDM the anode/filter combination (W/Rh,
W/Ag) and the tube voltage (kVp) are automatically selected by the system based on breast thickness.
Automatic exposure control system is used to determine the tube current and exposure time (mAs) for both DBT and FFDM.
Dose assessment was performed by means of a radiation dose-tracking tool developed in our department that extracts data from the DICOM Header produced by the equipment and archived in our PACS (Synapse Fujifilm,
Japan).
Average Glandular Dose (AGD) as evaluated by the system was extracted by our dose-tracking tool together with technical scan parameters.
Figure 1 shows a scatter time plot which indicates the different use over time of DBT either alone or in combination with FFDM,
suggesting some doubts among radiologists about how and when to use DBT in consideration of the recent introduction of this technique in their clinical practice.
Table 1 shows the median values of AGD observed: 4.64 mGy for FFDM,
5.82 mGy for DBT and 6.00 mGy for FFDM plus DBT.
These dose values are reffered to the whole procedure which includes at least four views.
Mean breast thickness value is 4.9 cm.
In Figure 2 and Table 2,
a comparison between FFDM and DBT is reported,
taking into consideration the different breast thickness.
Data clearly show that patients receive much more radiation dose when DBT is used,
and the gap between DBT and FFDM increases with the increasing breast thickness.
AGD median values were 0.70 mGy and 1.17 mGy with breast thickness lower than 35 mm,
1.01 mGy and 1.42 mGy with breast thickness between 35 and 54 mm,
1.37 mGy and 2.13 mGy with breast thickness between 55 and 74 mm,
and 1.71 mGy and 3.15 mGy with breast thickness higher than 74 cm,
for FFDM and DBT respectively.
Therefore,
the percentage increase of the radiation dose value with DBT versus FFDM goes from 41% (for breast thickness of 35-54 mm) to 84% (for breast thickness higher than 74 mm).
No significant dosimetric difference was observed between CC and MLO views for both DBT and FFDM.
In Figure 3,
mean AGD values of FFDM and DBT at different patient age are shown.
Here too,
DBT indicates to expose patient at a steady higher radiation dose compared to FFDM.
Radiation dose due to DBT goes up by 54% (mean percentage variation,
min/max 41% - 67%) for CC projection and goes up by 40% for MLO projection (mean percentage variation,
min/max 31% - 49%).
The curve trend of the two scan modalities is similar,
with a decreasing dose exposure in elder patients as breast density gradually decreases after menopause.