Information about the use of imaging in patients with suspected or confirmed COVID-19 was collected in order to assess current imaging practices in different clinical scenarios related to COVID-19. The survey gathered responses from 52 institutions settled in 34countriesrepresentingsixcontinents as follows: 10 institutions from six countries in Africa, nine institutions from seven countries in Asia, one institution from Australia, 22 institutions from 15 countries in Europe, five institutions from two countries in North America and five institutions from three countries in South America (Table 1).
Two radiology departments, one institution in Poland and one in the Netherlands, completed the survey, but since they have not been involved in the management of COVID-19 patients, data from those two institutions were excluded from further analysis. Finally, responses from 50 radiology departments from 33 countries were analyzed. The response rate was 88%.
The questions in the survey referred to the use of imaging in patients with suspected or confirmed COVID-19 from asymptomatic to critically ill and at the end of confinement. For diagnostic workup and management purposes in patients with suspected or confirmed COVID-19 chest imaging was performed both on an outpatient basis and during the hospitalization, depending on the specific clinical scenario. Important variations in imaging practices related to COVID-19 across the world have been revealed for different disease severity and various clinical scenarios.
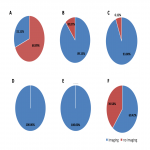
In the majority of institutions (69%) imaging is not performed in asymptomatic subjects. Of those who use imaging for detection of lung disease related to COVID-19, 50% use chest X-ray (CXR), 36% chest CT and 14% both modalities (CXR and CT). The rationale for use of imaging is easy access (57%) and because the results of imaging are faster than molecular test results (36%), while in 7% of the institutions molecular tests were not available.
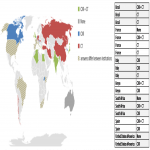
In symptomatic patients with suspected COVID-19 the vast majority of imaging departments perform imaging (89%), of which 37% use chest X-ray, 34% chest CT and 29% both modalities (CXR and CT). Faster results than molecular tests (51%) and easy access (39%) were the main reasons for imaging use, while in 5% of the institutions there was no access to molecular tests. Geographical variations in the use of imaging in symptomatic patients with suspected COVID-19 are presented in Figure 1.
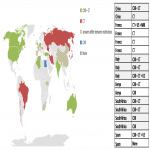
In patients with confirmed COVID-19 imaging is performed in the vast majority of imaging departments (94%), of which 22% use chest X-ray, 28% chest CT, and 43% both CXR and CT. In some institutions the combination of three modalities (CXR, CT and lung ultrasound [LUS] or CT, LUS and MRI [4% and 2%]) is used. The purpose of imaging use in patients with confirmed COVID-19 was detection of lung disease (96%) or thrombotic complication (52%) related to COVID-19. Geographical variations in the use of imaging in patients with confirmed COVID-19 are shown in Figure 2.
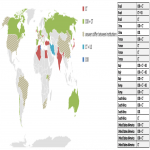
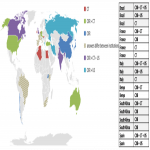
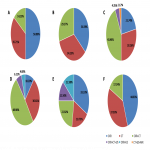
All imaging departments analyzed in this survey reported the use of imaging in patients with COVID-19 showing severe symptoms or who were critically ill. For those reasons, chest X-ray is performed in 10% and 33% of institutions respectively, chest CT in 31% and 19% of institutions, both CXR and CT in 49% and 23% of institutions and three imaging modalities (CXR, CT and LUS) in 6% and 13% of institutions. Additionally, in patients with severe symptoms the combination of chest CT and LUS was used in 4% of institutions, while in 13% of institutions the combination of CXR and LUS was used in patients who were critically ill. The purpose of imaging use in patients showing severe symptoms or being critically ill was the detection of lung disease (98% and 88% respectively) or thrombotic complication (73% and 54% respectively) related to COVID-19. Geographical variations in the use of imaging in patients with COVID-19 showing severe symptoms or who were critically ill are shown in Figures 3 and 4.
At the end of confinement, imaging is used in 60% of institutions (45% CXR, 38% CT and 17% both modalities) in order to follow-up lung disease. Graphical representation of general use of imaging related to COVID-19 and use of different imaging techniques in various clinical scenarios are given in Figures 5 and 6.
The use of imaging is organized in line with guidelines and recommendations in 98% of institutions (70% of those institutions follow national guidelines or recommendations, 55% local guidelines or recommendations and 28% other guidance, e.g. from international professional societies). Structured reporting is performed in 58% of institutions analyzed in this survey. In all institutions, reports were made by radiologists. The vast majority of institutions reported significant impact of the COVID-19 pandemic on the imaging department’s routine activity (83%), 8% reported moderate and 8% low impact.