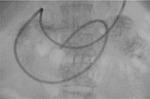
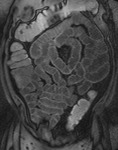
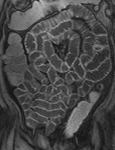
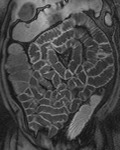
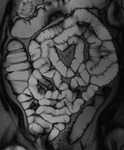
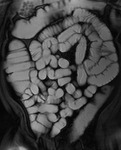
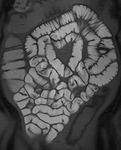
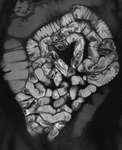
Technique of MR Enteroclysis
Imaging protocols and technique may vary due to differences in available equipment,
time constraints and personal preference.
A 1.5 T Siemens MRI scanner with a 12-channel,
phased array torso receiver coil is used at our institution.
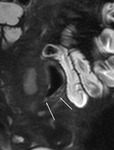
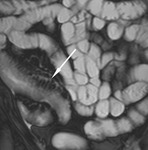
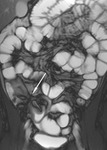
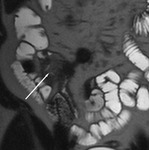
Naso-jejunal intubation
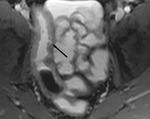
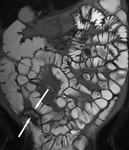
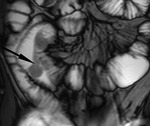
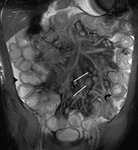
Under fluoroscopic guidance a naso-jejunal catheter is placed in an optimal position just beyond the duodenal-jejunal flexure in order to decrease the chance of luminal contrast refluxing back into the stomach (Fig.
1). The patient is offered sedation and analgesia to minimize discomfort during the procedure.
Administration of Luminal Contrast
The patient is then positioned prone in the MRI scanner.
The prone position facilitates separation of small bowel loops and decreases the volume of peritoneal cavity to be imaged.
The prone position has also been shown to improve luminal distention [14].
Approximately 1000 to 2000 ml of polyethylene glycol is administered via the catheter using gravity as a driving force.
Using this method a flow rate of around 100-150 ml/min can be achieved.
The aim of an optimal contrast agent is to give high contrast between bowel wall and lumen with minimal absorption and no significant adverse side-effects.
Polyethylene glycol is a bi-phasic enteric contrast with a high intensity signal on T2 weighted sequences and a low intensity signal on T1 weighted sequences.
Other contrast agents used are positive contrast agents (high T1 and T2 signal intensity) and negative contrast agents (low T1 and T2 signal intensity).
Table 2 summarizes the different types of contrast agents available.
|
Biphasic Enteric Contrast Agents
|
Positive Enteric Contrast Agents
|
Negative Enteric Contrast Agents
|
|
Polyethylene Glycol
Water
Methyl Cellulose
Mannitol
Sorbitol
|
Dilute Gadolinium
Milk (high fat content)
Grapefruit juice
Pineapple juice
|
Iron Oxide agents
Dilute Barium
|
Table 2.
Enteral contrast agents.
MR Pulse Sequences
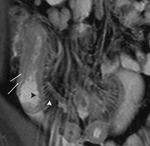
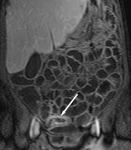
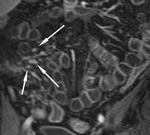
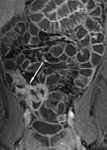
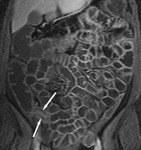
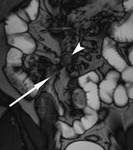
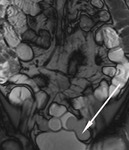
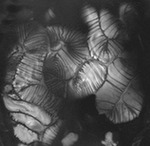
The transit of contrast and distention of the small bowel is monitored with MR fluoroscopy performed with a thick slab (50mm) half-Fourier acquisition single-shot turbo spin-echo (HASTE) sequence with fat saturation (Fig.
2). This is repeated at intervals of around 30 seconds during normal breathing with the interval adjusted according to progression of contrast.
When the contrast reaches the terminal or neo-terminal ileum the infusion of enteral contrast is stopped.
Once the enteral contrast has reached the caecum or the end of the available small bowel 20mg of hyoscine butyl-bromide is administered intravenously to reduce the effect of motion artifact from peristalsis during image acquisition and also to prolong small-bowel distention.
Further pulse sequences are then performed with the aim to balance the effects of the bi-phasic enteric contrast and the intra-venous contrast to produce the maximum amount of diagnostic information.
These sequences are summarized in table 3.
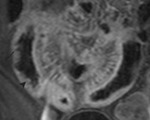
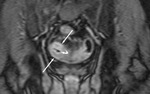
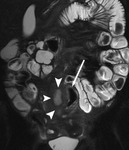
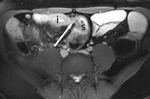
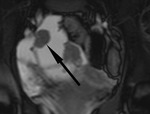
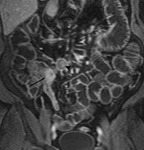
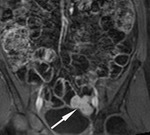
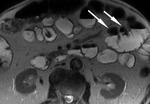
First a pre-contrast three-dimensional fast low angle shot fat saturated T1-weighted sequence is performed during a single breath hold.
This sequence is called volumetric interpolated single breath hold examination (VIBE) on the Siemens scanner (Fig 3).
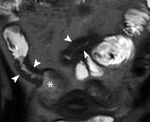
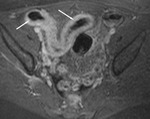
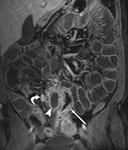
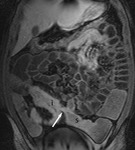
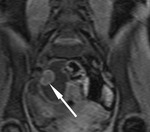
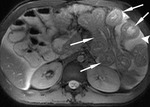
Following injection of a gadolinium intravenous contrast agent (0.2mg/Kg) two further coronal VIBE sequences are performed at 30 (Fig.
4) and 70 seconds (Fig 5).
The VIBE sequences are susceptible to movement artefacts from bowel peristalsis therefore they are performed immediately after the administration of hyoscine butyl-bromide.
The main use of these sequences is to identify areas of abnormal enhancement and to identify areas of active inflammation in Crohn’s disease.
The next set of sequences performed are the steady state gradient-echo sequences.
These sequences are T2 weighted and are called true fast imaging with steady state precession (true FISP) on the Siemens MRI scanners.
Two coronal sequences are performed,
one without (Fig.
6) and one with fat-saturation (Fig.
7). These sequences give a useful overview of the small bowel and good demonstration of mesenteric pathology including lymphadenopathy and mesenteric vascularity.
Axial true FISP acquisition may also be performed at this point.
T2 weighted ultra fast spin echo sequence is then performed in the coronal plane.
This is called half-Fourier acquisition single-shot turbo spin-echo (HASTE) on the Siemens scanner.
These are performed with (Fig.
8) and without fat saturation (Fig.
9) and best demonstrate mucosal and mural pathology.
They are however susceptible to flow artifacts within the lumen.
|
Sequence
|
TR/TE
|
Uses
|
Limitations
|
|
HASTE Thick slab
|
3870/209
|
Monitors contrast progress
Assess bowel dynamics
|
Only two
dimensional
|
|
VIBE
Pre-contrast
|
5.12/2.23
|
3 dimensional acquisition
|
Motion artefact
|
|
VIBE
30s post contrast
|
5.12/2.23
|
Identify areas of abnormal enhancement
|
Motion artefact
|
|
VIBE
70s post contrast
|
5.12/2.23
|
Identify areas of abnormal enhancement
|
Motion artefact
|
|
True FISP
|
3.76/1.88
|
Anatomical overview
Mesenteric evaluation
|
Susceptibility artefact
Black boundary artifact
|
|
True FISP with fat saturation
|
3.76/1.88
|
Focal wall thickening
Assess peri-enteric inflammation
|
Susceptibility artefact
|
|
T2 HASTE
|
1190/148
|
Bowel wall oedema
Ulceration
|
Intra-luminal flow artefact
|
|
T2 HASTE with fat saturation
|
1190/148
|
Mural thickening and oedema
|
Intra-luminal flow artefact
|
Table 3. Summary of MR Enteroclysis Pulse Sequences.
Imaging Findings in Small Bowel Pathology
Crohn’s Disease
Crohn’s disease is an autoimmune disorder of unknown aetiology that affects mainly young people and typically follows a chronic and relapsing course.
It can effect any part of the gastrointestinal tract but more commonly effects the small bowel with a predeliction for the terminal ileum.
The spectrum of imaging findings in small bowel Crohn’s disease can be classified into:
- Active inflammatory disease.
- Penetrating disease (including fistulae and abscess formation)
- Fibrostenotic disease.
Patients may exhibit imaging characteristics of one or more of these subtypes emphasizing the complex nature of the disease [15,16].
1.
Active Inflammatory Disease
Active inflammatory Crohn’s disease is a spectrum of varying degrees of neutrophillic crypt injury ranging from neutrophillic infiltration in mild disease to crypt epithelial necrosis,
crypt abscess formation and eventually ulcer formation. Superficial apthous ulcers form at first which then may progress to deep fissuring ulcers resulting in submucosal inflammation and oedema.
Other pathological features of active inflammatory disease include increased mesenteric vascularity and reactive mesenteric lymphadenopathy.
MR imaging has excellent sensitivity for detection of active inflammatory Crohn disease [10,17-19].
There are several imaging features seen with MRE that are indicative of increased disease activity.
These include,
mucosal enhancement,
mucosal ulceration,
mural thickening,
intra-mural oedema,
wall enhancement,
mesenteric vascular engorgement and hyper-enhancing inflammatory lymph nodes.
[20-24].
Mucosal Ulceration
Early superficial ulceration (apthae) are not consistently demonstrated on MRE when compared to traditional fluoroscopic enteroclysis,
a fact attributed to its inferior spatial resolution.
However with adequate luminal distention deep fissuring ulceration (Fig.10) and cobblestone mucosa (Fig.
11),(Fig.
12) can be readily appreciated with MRE [20,25].
Mural thickening and Submucosal Oedema
A small bowel wall thickness of greater than 3mm is considered abnormal and can indicate active inflammatory disease [24].
Assessment of bowel wall thickness is best performed on the HASTE sequences as the black border artifact seen on true FISP images can cause inaccurate assessment of true wall thickness (Fig.
13).
Submucosal oedema is another feature of active inflammatory disease and is best seen on the fat saturated T2 weighted images as high signal in the submucosa (Fig.
14) In fibrostenotic disease there is low T2 submucosal signal accompanying the mural thickening [26].
The caveat however is that the absence of submucosal T2 hyper-intensity does not exclude active disease and the presence of high T2 wall signal may be from intramural fat depostion found in chronic strictures [13].
Bowel Wall Enhancement
There are three main patterns of enhancement seen in active Crohn’s disease:
1.
Subtle mucosal enhancement may be one of the earliest signs of active inflammation.
This is best appreciated by comparing enhancement intensity to adjacent normal small bowel loops with similar distention [7].
(Fig.
15).
2.
A stratified enhancement pattern is also indicative of disease activity,
its appearance due to submucosal oedema sandwiched between mucosal and serosal enhancement [27] (Fig.
16).
3.
Diffuse homogenous mural enhancement is commonly encountered in transmural inflammation as opposed to inhomogenous low level enhancement which is often seen in fibrosis (Fig.
17).
Increased Mesenteric Vascularity
Vascular engorgement occurs in the mesentery adjacent to the inflamed small bowel loop with distention of the vasa recta giving rise to the comb sign.
This feature of active inflammation is best seen on the true FISP and the post contrast VIBE sequences (Fig.
18).
Lymph Node Enhancement
Lymphadenopathy frequently accompanies active Crohn's disease.
One specific feature of active inflammatory disease is increased nodal enhancement even when the nodes are not enlarged [26,28] (Fig.
19).
2.
Disease Penetration
Progression from deep ulcer formation to transmural inflammation may then lead on to sinus formation.
This culminates as either in an abscess or fistulation to adjacent loops of small bowel,
colon or other viscera such as bladder and stomach.
Entero-cutaneous fistulation may also occur.
Abscess
Abscesses appear as well defined encapsulated collections with a high signal intensity on T2 weighted sequences (Fig.
20) and a low signal intensity on T1 weighted sequences. The T2 signal may be heterogenous due to the presence of solid and gaseous components.
There is usually strong enhancement of the abscess wall on post contrast T1 sequences (Fig.
21).
MRE has a very high sensitivity for identifying abscess (up to 100%) [29,30].
Identifying features of intra-abdominal sepsis is of high importance as this is a relative contraindication to commencing immunomodulating drug therapy [31].
Fistulation
MRI has a sensitivity of around 71-83% in demonstrating enteric fistulae [29,30].
Sinuses and fistulae appear as high T2 signal intensity tracts radiating out from a segment of diseased bowel to surrounding structures and usually demonstrates intense enhancement following intravenous contrast administration [32].
Entero-enteric fistulae typically have a stellate appearance with several loops of bowel being pulled into a central point (Fig.
22). There is associated enhancement of these loops if they are acutely inflamed (Fig.
23). Pelvic loops of diseased small bowel may also fistulate into the adjacent colon (Fig.
24), (Fig.
25).
3.
Fibrostenotic Disease
Persisting mural inflammation of the small bowel with Crohn’s disease will eventually progress to fibrosis.
This may then lead on to stricture formation (fibrostenotic disease).
It is important to recognize this pathology as these chronic strictures will not respond to medical therapy and may require surgical resection if they are causing proximal small bowel obstruction.
Fibrostenotic segments of small bowel will demonstrate abnormal mural thickening but typically there is intermediate or low signal intensity on T2 weighted sequences [26] (Fig.
26).
Bowel dilatation proximal to a fibrostenotic segment implies a high grade stenosis. Fibrostenotic segments tend to demonstrate inhomogenous low level enhancement as opposed to the avid post contrast mural enhancement patterns of active inflamed small bowel (Fig.
27).
MR fluoroscopy can be a useful sequence to assess this pathology with fibrotic strictures appearing as non peristalsing bowel segments with progressive proximal small bowel distention.
Small Bowel Tumours
Peutz-Jeghers Syndrome
Peutz-Jeghers syndrome is an autosomal dominant inherited disease which can effect both males and females and has no racial predominance.
It is characterized by muco-cutaneous pigmentation around the lips,
peri-oral and peri-orbital region and also hamartomatous polyps in the gastrointestinal tract [33].
These polyps can be found anywhere in the GI tract from the stomach to the rectum but most commonly occur in the small intestine [34]. The syndrome carries an inherent risk of developing gastrointestinal adenocarcinoma with estimated frequency of malignancy being around 2% to 3% [35].
Dysplastic changes have been reported in small bowel polyps and therefore malignant transformation remains a potential risk and therefore careful surveillance screening of Peutz-Jeghers patients is advised [35].
Typical imaging findings are of multiple soft tissue polyps seen throughout the gastrointestinal tract appearing as filling defects in the fluid filled lumen which is of high signal intensity on the FISP and HASTE sequences (Fig.
28).
Care must be taken on interpreting the HASTE sequences as luminal flow and air bubble artifact can be mistaken for polyps.
These potential pitfalls can be avoided with cross reference to the true FISP and VIBE images.
Polyps can be quite sizeable (Fig.
29) and show similar enhancement patterns to the adjacent small bowel mucosa and submucosa (Fig.
30).
Long pedunculated polyps are not uncommon (Fig.
31) and can be a lead point for intussusception.
To prevent this from happening endoscopic snaring and removal of the larger polyps is advised (Fig.
32).
Carcinoid
Carcinoid tumours account for 2% of all gastrointestinal tumours and are the second most common small bowel malignancy [36].
They arise from endocrine amine precursor uptake and decarboxylation (APUD) cells that can be found throughout the gastrointestinal tract and other organs such as the pancreas and lung.
The primary tumour usually appears either as a discrete mass or as a segment of uniform bowel wall thickening that is usually iso-intense to muscle on T1 weighted imaging and either hyper or iso-intense to muscle on T2 weighted imaging [37] (Fig.
33).
The primary tumour will demonstrate intense enhancement following administration of gadolinium (Fig.
34). Mesenteric nodal extension appear as iso-intense masses on T1 and T2 which also enhance intensely. The surrounding desmoplastic reaction appears as hypo-intense strands on T2 weighted sequences radiating into the distorted mesentery [37] (Fig.
35).
MR enteroclysis with its superior soft tissue contrast and luminal distention can also demonstrate other small bowel tumours like adenocarcinoma and gastrointestinal stromal tumours (GIST) (Fig.36) (Fig 37).
Other Small Bowel Pathology
Lymphangectasia
Intestinal lymphangectasia is a rare disorder characterized by severe oedema,
small bowel thickening,
protein losing enteropathy,
ascites and pleural effusion [38]. The bowel wall thickening is the result of obstruction of the lymphatic vessels in the mucosa and submucosa [39,40].
Aetiology is classified into congenital lymphatic blockage (primary lymphangectasia) or due to inflammatory or neoplastic involvement of the lymphatic system (secondary lymphangectasia) [41].
There is diffuse thickening of the affected segment of small bowel with submucosal edema seen as hyper-intense signal on T2 weighted sequences (Fig.
38). Other features of the obstructed lymphatic system include mesenteric congestion,
enlarged mesenteric lymph nodes and ascites (Fig.
39).
Scleroderma
Scleroderma (progressive systemic sclerosis) is a systemic disease of uncertain etiology that results in widespread collagen deposition and tissue fibrosis [42] Gastrointestinal involvement occurs in up to 90% of patients with systemic sclerosis.
The pathological process involves smooth muscle atrophy and fibrosis caused by collagen deposition primarily in the tunica muscularis [43,44]. The oesophagus is the most common site of involvement with small bowel involvement seen in up to 50% of cases [45].
The appearance on MRE mirrors that of traditional fluoroscopic barium studies with narrow separation between the valvulae conniventes despite luminal dilatation,
the so called ‘hide-bound’ or ‘stack of coins’ small bowel sign (Fig.
40). MR fluoroscopy can demonstrate the disordered motility and delayed transition of luminal contrast.
Jejunal Diverticulosis
Jejunal diverticulosis is characterized by herniation of of the mucosa through sites of weakening on the mesenteric border of the jejunum.
These diverticulae of varying sizes are associated with a variety of complications including stasis and bacterial overgrowth,
diarrhoea,
malabsorption,
gastrointestinal bleeding,
inflammation and perforation.
Typical findings on conventional barium enteroclysis and CT are also clearly demonstrated on MRE with a well distended proximal jejunum.
These features are of discrete round or ovoid structures containing air or contrast that are found outside of the bowel lumen.
These outpouchings have a barely discernible wall and contain no small bowel folds.
Communication with the bowel lumen can often be demonstrated (Fig.
41).