This poster was originally presented at the RANZCR Annual Scientific Meeting 2011, October 6-9, in Melbourne/AU.
Congress:
RANZCR ASM 2011
Type:
Educational Exhibit
Keywords:
SPECT, PET, MR-Diffusion/Perfusion, MR physics, Neuroradiology brain, Imaging sequences
Authors:
M. McGuiness, A. Lane, A. Coulthard; Brisbane/AU
DOI:
10.1594/ranzcr2011/R-0032
Background
Perfusion of blood into tissues to provide oxygen and nutrients is a fundamental physiological process.
Patterns of hypo- and hyper-perfusion are seen in a myriad of pathological processes.
Current modalities of perfusion imaging in clinical use include Positron Emission Tomography (PET),
Single Photon Emission Computed Tomography (SPECT),
Perfusion Computed Tomography (PCT) and MRI dynamic susceptibility contrast (DCT).
Perfusion imaging
- Can be utilised to access the haemodynamics in all body systems,
detecting abnormalities in tissue perfusion before anatomical changes can be observed.
- Can add important functional information when coupled with more structurally detailed conventional imaging techniques (eg.
more precise quantification of area of infarction and ischaemic penumbra in stroke patients for thrombolysis selection).
Perfusion CT (PCT)
The Good:
- Readily availabe in the emergency setting with rapid acquisition time.
- Can be used in combination with non-enhanced CT and CT Angiogram in diagnosis of acute stroke.
There are two main techniques in PCT; slow/whole brain mapping to access cerebral blood volume and bolus imaging to more quantitatively access blood flow in a region of interest.
The bad:
- Radiation dose is in the vicinity 2-3 mSv and repeated examinations are limited by amount of contrast tolerated systemically.
- MRI has better whole brain coverage and the benefit of diffusion weighted sequences in acute stroke.
Clinical Applications:
- Acute and chronic cerebrovascular disorders,
trauma,
detection of vasospasm and tumour imaging.

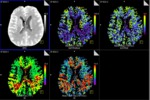
Fig. 0: CT perfusion images of a patient with cerebral vasospasm. Top row: source image; CBF (cerebral blood flow); CBV (cerebral blood volume). Bottom row: TTP (time to peak); MTT (mean transit time)
MRI dynamic susceptability contrast (DCT)
The good:
- Avoids ionising radiation,
suitable for paediatric population.
- Can be used in combination with diffusion weighted imaging (DWI) and MR Angiogram in diagnosis of acute stroke.
The bad:
- Requires gadolinium contrast and is subject to general contraindication to MRI.
- Lacks quantitative accuracy of PCT.
Clinical Applications:
- Acute and chronic cerebrovascular disorders,
detection of vasospasm and tumour imaging

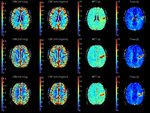
Fig. 0: Example images from MR perfusion study in acute left frontal infarction. Columns show (left to right) CBV (cerebral blood volume); CBF (cerebral blood flow); MTT (mean transit time); Tmax (Time to maximum).
Positron Emission Tomography (PET)
The good:
- Considered ‘gold standard’ in terms of quantative perfusion imaging assessing a variety of haemodynamic parameters.
The bad:
- Clinical use limited by cost,
availability and technical aspects.
- Requires radioisotope injection with radiation dose 0.5-2 mSv.
Clinical Applications:
- Chronic cerebrovascular disorders,
epilepsy,
dementia,
tumour imaging
Single Photon Emission Computed Tomography (SPECT)
The good:
- Repeatable and reproducible.
- Retension tracer (rapid uptake and stable concentration for hours) makes suitable for bedside imaging such as ictal SPECT.
The bad:
- Requires radioisotope injection and radiation dose of 3.5-12mSv.
- Relatively poor spatial resolution.
Clinical Applications:
- Epilepsy,
Dementia and chronic cerebrovascular disorder