Premature birth and neurodevelopmental delay
- Brain injury in premature infants is of enormous public health importance because of the large number of such infants who survive with serious neurodevelopmental disability”(1)
- Of Australian births in 2008
- 6.1% were low birth weight (LBW,
<2.5kg)
- 1% were very low birth weight (VLBW,
<1.5kg)
- 8.2% were preterm (<37 weeks gestation)(2)
- While survival rates of VLBW infants have improved,
this has been accompanied by an increase in the number of those survivors who have long term neurological deficits(3)
- Preterm birth and low birth weight is associated with higher rates of cerebral palsy,
intellectual disability and sensory impairment than in babies born at term(4)
- MRI studies are revealing that a higher proportion of this patient group suffers from a broader spectrum of subtle structural abnormalities that underlie the neurodevelopmental disabilities of school and behavioural problems including minor neuromotor dysfunction,
specific learning disability,
and language,
visual-perceptual and attention deficits(4)
Pathology in brief
Periventricular white-matter injury (PWMI)
- The most common form of brain injury and,
therefore,
the leading cause of chronic neurological morbidity in preterm infants(5)
- Includes both diffuse myelination disturbances and focal cystic necrotic lesions (periventricular leukomalacia; PVL)(5)
- The incidence of PVL appears to be declining,
while focal or diffuse noncystic injury is now the predominant lesion(1,
5)
- In terms of clinicopathological correlation,
it appears that cystic PVL accounts for the small group of infants who show spastic diplegia,
while non-cystic PVL is linked to those who display predominantly cognitive deficits(1)
Neuronal/axonal disease and deficits in volumetric development is likely to contribute to the spectrum of cognitive,
attentional,
behavioural and socialization deficits that have been observed(1).

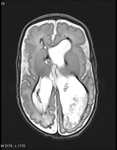
Fig. 0: Axial T2 weighted MRI of a 2 month old showing widespread intraventricular and periventricular haemorrhage and cystic periventricular leukomalacia
References: A.Lane, Royal Brisbane and Women's Hospital

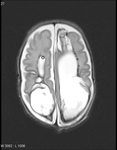
Fig. 0: Axial T2 weighted MRI of a 2 month old showing widespread intraventricular and periventricular haemorrhage and cystic periventricular leukomalacia.
References: A.Lane, Royal Brisbane and Women's Hospital
Imaging of preterm infants
- Ultrasound (US) is effective for detecting severe white matter lesions in preterm infants
- MRI
- is superior at detecting less severe damage(6)
- is more sensitive for detecting the diffuse,
non-cystic form of PVL than US(7,
8)
- demonstrates the site and extent of abnormalities more precisely and shows maturational processes in detail(9-11)
- Infants with diffuse white matter injury have been shown to be at risk for motor and cognitive impairment,
as well as behavioural problems(12)
- In a Swedish study by Horsch et.
al.
18% of infants born before 27 weeks gestation had moderate to severe white matter abnormalities on brain MRI at term(13)
Indications for neonatal MRI
Van Wezel-Meijler et.
al.
(14,
15) recommend neonatal MRI in the following conditions:
- Prematurity,
<30 weeks’ gestational age
- Hypoxic-ischaemic encephalopathy (HIE) stage 2 or 3 in (near) full term neonates
- US diagnosis of significant parenchymal brain injury,
such as inhomogeneous periventricular echodensities,
cystic periventricular leukomalacia,
periventricular haemorrhagic infarction,
arterial infarction
- US diagnosis of severe post-haemorrhage ventricular dilatation
- Traumatic delivery
- Clinical or US suspicion of abnormalities in the posterior fossa
- Clinical or US suspicion of abnormalities at the brain’s convexity
- Severe and/or symptomatic hypoglycaemia
- (suspected) metabolic disease
- Clinical or US suspicion of brain inflammation (meningitis,
encephalitis,
brain abscess)
- Congenital malformations with possible involvement of the brain
- Neurological signs of encephalopathy,
such as seizures,
abnormal consciousness,
and/or asymmetry,
not sufficiently explained by US findings
In addition to conventional (T1 and T2 weighted) MRI,
more advanced techniques such as diffusion tensor imaging,
function connectivity MRI,
volumetric analysis,
and surface-based morphometry are also being applied,
albeit some only in a research setting,
to the field of prematurity and neurodevelopmental disability(16).

Fig. 0: A research application. Right panel: tractography in term brain showing tracts in X axis (red), y axis (green) and z-axis (blue). Left panel: shows the difference in term born infants versus very preterm born infants studied at term age. Blue represents an increased density of fibre tracts (in the corticospinal tracts) and a reduced density of fibre tracts (in the callosal tracts) in the preterm born babies.
References: Rose SE, Hatzigeorgiou X, Strudwick MW, Durbridge G, Davies PS, Colditz PB. Magn Reson Med. 2008;60:761-7
Safety and quality issues with neonatal MRI
MRI advantages:
- Relatively safe technique
- Non-invasive
- Does not involve radiation
- Superior at detecting more subtle,
diffuse brain pathologies than other imaging modalities
MRI risks/limitations:
- Requires transportation of vulnerable patients out of the NICU to the radiology department
- Newborn infants are prone to hypothermia,
may be haemodynamically unstable,
may require respiratory support,
and are vulnerable to noise and other side effects of handling and transport
- Due to their small head size,
the use of standard MR head coils can result in suboptimal picture quality.
These risks or limitations can be significantly reduced with the use of the MRI compatible neonatal incubator (MRIcNI),
and the use of smaller dedicated head and body coils yields excellent image quality(17-20). MRI compatible neonatal incubators have made it possible to carry out safely the MR examination on younger,
smaller and more unstable infants(17).

Fig. 0: MRI compatible incubator (LMT Nomag Incubator)
References: Imaging Solutions Pty Ltd