This poster was originally presented at the RANZCR Annual Scientific Meeting 2011, October 6-9, in Melbourne/AU.
Congress:
RANZCR ASM 2011
Keywords:
Musculoskeletal bone, Musculoskeletal joint, Emergency, Digital radiography, Conventional radiography, Decision analysis, Athletic injuries, Trauma
Authors:
N. Kutaiba1, J. Cruickshank1, D. Arhanghelschi1, A. Al Joboory2; 1Ballarat/AU, 2Melbourne/AU
DOI:
10.1594/ranzcr2011/R-0104
Results
Literature review:
We found 3 retrospective and 5 prospective primary studies evaluating the use of x-rays for shoulder dislocation in the acute setting for pre- and post-reduction (Table 1).
Similar clinical factors were identified in these articles mainly involving age,
mechanism of injury and recurrence.
Three algorithms were suggested from three research groups studying this topic.
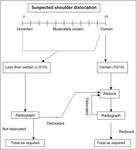
Figure 1 represents the Banff Shoulder Dislocation Guideline proposed by Shuster et al4.
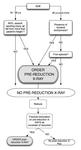
Figure 2 represents the algorithm suggested by Hendey et al for management of patients with suspected shoulder dislocation10.
Figure 3 represents the refined Quebec shoulder dislocation rule suggested by Emond et al6.
Table 1 Studies Evaluating Pre- and Post-Reduction Radiography for Shoulder Dislocations
|
Study
|
Purpose
|
Type
|
Setting
|
Conclusion
|
|
Harvey 19927
|
To evaluate the need for post-reduction X-rays in uncomplicated anterior shoulder dislocations.
|
Retrospective
|
Chart review of 69 shoulder dislocations from one ED over 18 months
|
Routine post-reduction x-rays are not needed to confirm shoulder reduction when clinically apparent.
|
|
Hendey 19968
|
To determine the incidence of clinically significant fractures or other abnormalities seen on post-reduction
shoulder radiographs
|
Retrospective
|
chart review of 131 patients who presented
with a total of 175 anterior shoulder dislocations from one ED over 4 years
|
Post-reduction x-rays rarely reveal any clinically significant abnormality after an anterior shoulder dislocation has been reduced.
|
|
Shuster 19993
|
To determine if emergency physicians can identify patients with anterior shoulder dislocation for whom pre-reduction x-rays do not alter management
|
Prospective
|
97 patients (mostly young males) with suspected shoulder dislocation from skiing/other sports activities in a rural ED over 7 months
|
When an experienced emergency physician is certain of the diagnosis of anterior shoulder dislocation,
pre-reduction radiographs delay treatment and do not alter management.
|
|
Hendey 20009
|
To determine necessity of pre-and post-reduction x-rays compared to physician’s certainty of diagnosis and reduction
|
Prospective
|
104 patients with suspected shoulder dislocations from one ED over 18 months
|
Emergency physicians are often certain of diagnosis and reduction.
Algorithm for ordering x-rays is suggested.
|
|
Shuster 20024
|
To determine,
through a proposed guideline,
whether emergency doctors are certain of diagnosing anterior shoulder dislocations without x-rays,
based on
|
Prospective
|
63 patients with suspected shoulder dislocation from skiing/other sports activities in a rural ED over 6 months
|
Emergency physicians are frequently certain of the diagnosis on clinical grounds alone and selective elimination of pre-reduction x-rays can be safely used following a guideline
|
|
Emond 20045
|
To identify risk factors for fractures associated
with an anterior shoulder dislocation
|
Retrospective: Case-Control
|
334 patients from one ED over 5 years
|
Age,
first episode and mechanism of injury predict clinically significant shoulder fracture-dislocations
|
|
Hendey 200610
|
To validate an algorithm for selective elimination of x-rays in suspected shoulder dislocations
|
Prospective
|
100 patients with suspected shoulder dislocations – 94 dislocations from one trauma centre ED over 22 months
|
Selective radiography reduces x-rays and length of stay in ED without missing significant fractures.
|
|
Kahn 200711
|
To determine whether post-reduction
radiographs add clinically important information to what is seen on pre-reduction X-rays
|
Prospective
|
55 patients with both pre- and post-reduction x-rays from one ED over a period of 18 months
|
Foregoing post-reduction X-rays will miss almost one-third of fractures associated with anterior shoulder dislocation,
but will not affect ED management
|
|
Emond 20096
|
To validate a clinical decision rule for predicting clinically significant fracture-dislocations
|
Prospective
|
222 patients from 4 ED’s over 3 years
|
Following a proposed decision rule would reduce pre- and post-reduction x-rays without missing significant fractures.
|
Retrospective evaluation:
There were 82 presentations to our ED from January to December 2010 with a diagnosis of shoulder dislocation.
66 were shoulder dislocations while 16 were other shoulder problems,
mostly acromio-clavicular joint disruption or shoulder pain.
17 were eliminated because reduction was achieved,
spontaneously or by someone else,
prior to presentation or clinical examination.
2 had missing records,
4 had failed reductions in ED and were taken to theatre,
and 2 patients had multiple presentations from which the first presentations were taken.
39 patients with anterior shoulder dislocations were eligible for this evaluation.
Mean age was 34.69 (95% CI 31.15 to 38.22) with 84.6% males.
51.3% (20/39) had recurrent dislocations,
23% (9/39) had first time dislocation and 25.6% (10/39) were not documented.
Clinical characteristics evaluated for these patients are outlined in Table 2.
Table 2 Clinical characteristics of patients
|
Characteristic
|
Number
|
Percentage %
|
|
Gender (Male)
|
33
|
84.6
|
|
Presentation
|
|
|
|
Recurrent
|
20
|
51.3
|
|
First episode
|
9
|
23.1
|
|
Not mentioned
|
10
|
25.6
|
|
Affected side (Right)
|
25
|
64.1
|
|
Alcohol Intoxication
|
3
|
7.7
|
|
Mechanism of Injury
|
|
|
|
Atraumatic
|
8
|
20.5
|
|
Fall < patient’s height
|
7
|
17.9
|
|
Fall > patient’s height
|
3
|
7.7
|
|
MVA
|
5
|
12.8
|
|
Sport
|
9
|
23.1
|
|
Assault
|
1
|
2.6
|
|
Collision
|
2
|
5.1
|
|
Not mentioned
|
4
|
10.3
|
|
Associated fractures
|
|
|
|
Hill-Sachs
|
8
|
20.5
|
|
Bankart
|
5
|
12.8
|
|
Hill-Sachs and Bankart
|
3
|
7.7
|
|
Greater tuberosity
|
2
|
5.1
|
|
Humeral head
|
1
|
2.6
|
X-rays were ordered for 46.2% (18/39) pre-reduction and 89.7% (35/39) post-reduction.
46.2% (18/39) had both pre-reduction and post-reduction x-rays with 3 patients requiring repeat x-rays after failed reduction.
10.3% (4/39) had no x-rays with reduction deemed successful clinically.
3 of which had recurrent shoulder dislocations and the fourth one had an atraumatic first dislocation.
8% (3/39) had clinically significant shoulder fracture-dislocations; greater tuberosity,
greater tuberosity and Hill-Sachs,
and humeral head fractures.
These 3 patients had both pre- and post-reduction x-rays.
8 patients had Hill-Sachs fractures on post-reduction x-rays,
5 of which had pre-reduction x-rays with 3 of these fractures not reported on the pre-reduction images.