METHOD
We performed a search on our database for all fetal MRIs performed over a 5 year period with mention of a CFC in the report.
All of these cases had been referred for MRI following detection of an intracranial cyst on the mid-trimester obstetric ultrasound.
We then retrospectively reviewed the antenatal and postnatal imaging of the patients (where available) along with their clinical records to determine clinical outcome.
RESULTS
Five cases with pre and post natal MRI imaging were identified with a further sixth case in which termination of pregnancy was performed following review of two sequential fetal MRIs.
The findings in these 6 cases are summarised in the following table:
|
Case
|
Sex
|
GA at fetal
MRI (weeks)
|
Side
|
Maximal diameter at diagnosis (mm)
|
Maximal diameter postnatally (mm)
|
Associated anomalies
|
Treatment
|
Clinical outcome
(age in years)
|
|
1
|
F
|
31+4
|
L
|
37
|
82
|
LTA,
CC dys
|
Fen,
CPS
|
RSI,
NNS (4)
|
|
2
|
M
|
28+4
|
L
|
29
|
37
|
LTA
|
Medication
|
Focal seizures (1)
|
|
3
|
F
|
24
|
L
|
25
|
78
|
LTA,
HC
|
VPS,
CPS
|
HC/RI,
NNS (1.5)
|
|
4
|
M
|
34
|
L
|
20
|
29
|
LTA,
Hippo
|
None
|
Seizure now well (7)
|
|
5
|
M
|
31+2
|
R
|
24
|
29
|
None
|
None
|
NNS (2)
|
|
6
|
F
|
32
|
L
|
62
|
na
|
LTA,CC dys,
EH
|
na
|
TOP
|
GA gestational age,
F female,
M male,
L left,
R right,
LTA left temporal atrophy,
CC dys corpus callosum dysgenesis,
HC hydrocephalus,
Hippo Hippocampal compression,
EH enlarged hemicranium,
Fen fenestration of cyst,
CPS cystoperitoneal shunt,
VPS ventriculoperitoneal shunt,
RSI recurrent surgical intervention,
NNS no neurological sequelae,
RI recurrent infection,
TOP termination of pregnancy
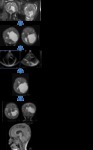
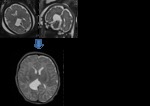
Case 1: Fig. 1
A left CFC measuring 37x36x25mm was identified on fetal MRI (FMRI) at 31 weeks and 4 days gestation with mass effect on the left mesial temporal and occipital lobes (Figure 1a) .
Postnatal imaging at 16 days demonstrated an increase in size and mass effect of the left CFC (Figure 1b).
Following initial successful endoscopic cyst fenestration for increased mass effect on the adjacent left hemisphere,
the cyst reaccumulated and a cystoperitoneal shunt (CPS) was placed.
The cyst reduced in size.
The patient was left with some atrophy of the temporal lobe and posterior corpus callosum (Figure 1c-e).
He is currently 4 years old and has so far demonstrated normal development with no neurological sequelae.
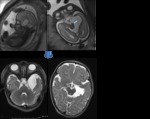
Case 2: Fig. 2
A left CFC measuring 29x25x24mm was identified on FMRI at 28 weeks and 4 days gestation.
It was causing compression of the ipsilateral temporal lobe and cerebral peduncle (Figure 2a).
Following birth,
the patient developed focal seizures for which a post-natal MRI was performed at 57 days.
This demonstrated ongoing left temporal lobe compression but decrease in the relative size of the CFC (Figure 2b).
At time of writing,
the child is 6 months old and the focal seizures have persisted requiring anti-epileptic medication.
No neurosurgical intervention has been performed.
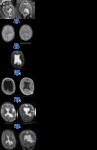
Case 3: Fig. 3
A left CFC measuring 25x20x16mm was identified on FMRI at 24 weeks gestation.
There was no significant mass effect (Figure 3a).
Postnatal MRI at 2 days demonstrated an increase in cyst size with evidence of new direct communication with the cavum vergae (Figure 3b).
The lateral ventricles were normal.
MRI at 1 month demonstrated marked size increase of the cavum vergae with significant mass effect and new ventriculomegaly (Figure 3c).
A VP shunt was inserted at 5 months.
Initial positioning was incorrect with further ventricular enlargement demonstrated; repositioning was successful (Figure 3d).
MRI at 8 months showed decompression of the cyst and ventricular system but persistent atrophy of the left temporal lobe (Figure 3e).
The most recent MRI (at 13 months) demonstrated stable ventricular size but reaccumulation of the CFC (Figure 3f).
Whilst this child has,
to date,
no evidence of developmental delay or focal neurological deficit,
she has had two admissions to hospital with ventriculoperitoneal shunt infection and has persistent hydrocephalus confirming cyst-related morbidity.
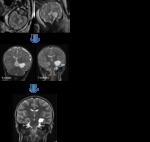
Case 4: Fig. 4
A left CFC measuring 20x19x19mm was identified on FMRI at 34 weeks gestation (Figure 4a).
Postnatal MRI at 6 weeks and 7 months demonstrated a stable relative size of the CFC but with compression of the left temporal lobe and hippocampus (Figure 4b).
The most recent MRI at 7 years of age demonstrated a relative reduction in size of the CFC but unchanged hippocampal compression (Figure 4c).
Other than a single afebrile seizure in infancy,
the child has remained well.
Case 5: Fig. 5
A right CFC measuring 24x20x19mm was identified on FMRI at 31 weeks (Figure 5a).
Postnatal MRI showed relative stability of cyst size with minimal compression of the occipital horn of the right lateral ventricle (Figure 5b).
Ultrasound assessment at 14 months showed a relative reduction in size of the CFC and no significant mass effect.
The child remained well and has been discharged from neurological/radiological follow up.
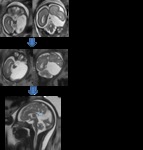
Case 6: Fig. 6
A large left CFC (42x23x21mm) was demonstrated on FMRI at 27 weeks gestation (Figure 6a).
A follow up study performed at 32 weeks gestation demonstrated cyst enlargement (62x45x38mm) with expansion of the left hemicranium and displacement of the left temporal lobe (Figure 6b).
In addition,
there was dysgenesis of the posterior body and splenium of the corpus callosum (Figure 6c).
Following counselling and multi-disciplinary team discussion,
a termination of pregnancy was performed at 33 weeks gestation.