All cases below were collected from our public and private clinical practice over the last 12 months.
Fig.
1 & 2
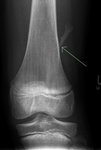
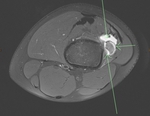
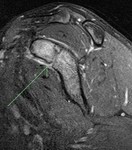
High Grade surface osteosarcoma (histologically proven).
Clinical: 20 year old male with pain in distal left femur.
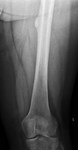
Case imaging findings: X-ray showed partially calcified surface based mass with spiculated periosteal reaction indicating an aggressive lesion.
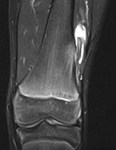
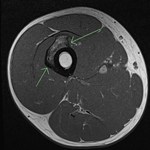
MRI demonstrated a heterogeneous,
high signal,
avidly enhancing surface based mass.
A partially calcified/low signal matrix,
and adjacent spiculated/sunburst periosteal reaction were present.
Cortical destruction,
medullary oedema/enhancement were also demonstrated.
The soft tissue mass involved a large percentage of the cortical circumference.
General imaging features of high grade surface osteosarcoma: Radiographs show a dense soft tissue ossification,
periosteal reaction,
cortical erosion and thickening.
MRI shows high T1 and T2 signal intensities with avid enhancement post gadolinium.
Tips: The tumour often surrounds a majority of the shaft circumference,
a feature which favours high grade surface osteosarcoma over the main differential of periosteal osteosarcoma.
Fig. 3,
4 & 5
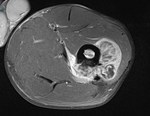
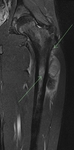
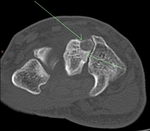
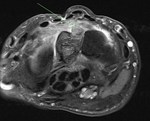
Osteochondroma with stalk fracture and bursal formation.
Clinical: Adolescent male with distal femoral mass and pain.
Case imaging findings: X-ray showed pedunculated osseous lesion extending away from joint at the distal femur.
Fracture noted at base of lesion. MRI demonstrated an osteochondroma of the distal left femur with stalk fracture and adjacent bone oedema.
Hyperintense bursal formation adjacent to the lesion deep to quadriceps and iliotibial band was noted.
The cartilaginous cap was smooth and measured less than 1cm.
General imaging features of osteochondroma: X-rays demonstrate a stalk like protuberance growing away from the physis.
The younger the patient the closer it is to the growth plate.
Tips: Most common around the knee.
A thickened cartilage cap (>2cm adults and >3cm in children) is suggestive of malignant transformation (approx 1-2% of cases). Large soft tissue mass or growth of cap post skeletal maturity is also concerning for malignant transformation. Caveat - do not mistake high signal,
peripherally enhancing bursa for malignant transformation.
Fig.
6
Parosteal osteosarcoma (histologically proven).
Clinical: Distal left femoral mass in an adult female incidentally found on CT arthrogram performed to assess menisci.
Case imaging findings: CT arthrogram of the left knee demonstrated a well defined surface based lesion with hyperdense matrix.
Intramedullary extension was seen posteriorly.
There was the classic 'string sign' anteriorly as demonstrated by a cleft between the lesion and bone surface.
General imaging features of parosteal sarcoma: x-rays - lobulated,
oval and exophytic mass with central dense ossification in continuation with the bone.
A clear cleavage plane between the tumour and normal cortex (string sign) is characteristic but not a constant finding.
On MRI low grade lesions show low T1 & T2 signal.
Fluid sensitive sequences show high signal involvement of the cortex and marrow.
Tips: If predominantly high T2 signal more likely to be high grade. Important to mention intramedullary extension to allow adequate surgical resection.
These have a better prognosis than conventional osteosarcoma.
Fig. 7 & 8
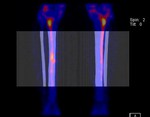
Medial tibial stress syndrome (shin splints/MTSS).
Clinical: Chronic anterior lower leg pain in young athelete.
Case imaging findings: MRI showed soft tissue oedema,
periosteal and cortical oedema in the anteromedial tibia bilaterally. SPECT/CT on delayed images demonstrated linear symmetrical uptake in a cortical distribution of both tibia.
General imaging features of medial tibial stress syndrome: Plain radiography is limited in diagnosis.
It may show periosteal elevation.
3 phase bone scan can show focal hyperaemia and delayed increased uptake but cannot differentiate between stress fracture.
This distinction can be improved with SPECT/CT.
MRI shows periosteal and bone marrow oedema.
Tips: On MRI pretibial oedema should not be mistaken for MTSS,
look for associated cortical oedema.
Fig.
9
Coracoid apophysitis (proven on serial imaging)
Clinical: Teenager with anterior shoulder pain.
Case imaging findings: MRI demonstrated coracoid apophysitis/stress response with high T2 signal/bone oedema,
widened physis and periosteal reaction. The short head of biceps brachii origin attaching to the coracoid appeared normal.
This resolved with conservative management as demonstrated on serial imaging.
General imaging features of apophysitis: X-ray may show avulsed apophysis or periosteal reaction.
MRI demonstrates high T2 signal at apophysis and physis.
Physis may be widened.
High T2 signal periosteal reaction and soft tissue oedema may also be evident.
Tips: Apophyseal avulsions and apophysitis should always be considered in adolescents with musculoskeletal pain as the apophysis is the weakest link in the chain of the teno-ossoeus unit. The associated periosteal reaction can mimic aggressive bone lesions.
Fig. 10 & 11
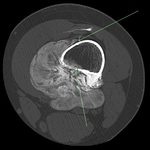
Osteoid osteoma wrist
Clinical: Hand pain and swelling.
Case imaging findings: CT showed the osteoid osteoma nidus in the capitate with adjacent scerosis. MRI revealed bone,
periosteal and soft tissue oedema adjacent to nidus.
General imaging features of osteoid osteoma: Commonly located in long tubular bones with thick and dense periosteal reaction that blends with thickened cortex.
Central lucent nidus usually evident.
CT shows location of lesion and nidus.
On MR the nidus appears hyperintense to skeletal muscle on T1WI and enhances avidly. Bone scan shows focal intense uptake at the site of nidus and the classic 'double density' sign.
Tips: Look for central nidus. Classic clinical scenario of night pain and relief with NSAIDS has often proven true in the authors experience.
When performing marker placement prior to CT guided ablation,
the author has found that the patient's are often able to pin point the nidus very accurately based on site of pain.
(The nidus must be ablated to effectively treat the lesion.)
Fig.
12
Surface osteoma
Clinical: Incidental finding on femur x-ray post trauma.
Case imaging findings: AP x-ray showed well defined,
dense surface lesion in the proximal femur in keeping with non aggressive osseous lesion/surface osteoma.
General imaging features of surface osteoma: Radiographs show a lesion with homogenous bone denisty,
sharply defined borders and no periosteal reaction. CT appearance is similar to radiographs. MR shows low signal intensity on all sequences due to lack of protons in cancellous bone.
Tips: Rarely involve long bones so when present suspect Gardner Syndrome (osteomas,
soft tissue tumours and colonic polyposis).
Fig.
13
Stress fracture
Clinical: Middle aged woman with foot pain.
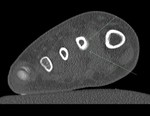
Case imaging findings: X-ray and CT image through right foot demonstrated periosteal reaction of second metatarsal shaft related to chronic stress response.
General imaging features of stress fracture: In early stress fracture,
radiographs may show faint cortical resorption or periosteal reaction. Linear sclerosis or focal periosteal reaction is usually seen in subacute or chronic stress fracture. CT may show the fracture as a lucency. MR in early stress fracture shows mild marrow oedema with adjacent soft tissue oedema. 3 phase bone scan can show hyperaemia and increased focal uptake on delayed images. Bone scan is highly sensitive but less specific than MR.
Tips: MR is sensitive and specific for stress fractures.
In the foot 90% occur in 2nd & 3rd metatarsals. Subtle periosteal reaction may be all you see.
Serial imaging is key in confirming diagnosis.
Fig.
14
Heterotopic ossification/myositis ossificans
Clinical: Male in third decade with history of thigh trauma.
Case imaging findings: MRI through the distal femur demonstrated a well defined surface bone lesion with low signal rim and central fat signal matrix in keeping with mature heterotopic ossification/myositis ossificans which resembles normal bone.
General imaging features of myositis ossificans: Relate to the age of the lesion.
Early radiographs may show a soft tissue mass with amorphous osteoid matrix. This progressively organises with more mature cortical bone peripherally and less mature bone centrally (termed zoning).
In the early stage, CT findings are of a low density soft tissue mass.
On MRI early lesions usually appear isointense to muscle on T1 and hyperintense and heterogenous on T2. MRI may show marrow oedema,
periosteal reaction and peripheral oedema which can mimic periosteal sarcoma.
Late stage appearances such as in figure 14 are of a well defined heterogenous mass with low signal rim (cortical bone like),
high T1 signal centre (medullary bone like) and no oedema or periosteal reaction.
Tips: Gradual ossification seen on serial imaging from the periphery towards the centre with more mature bone peripherally and less mature bone centrally (zoning) is a characteristic radiographic finding and helps to differentiate from periosteal osteosarcoma.
Fig.
15
Gout
Clinical: Middle aged man with ankle swelling.
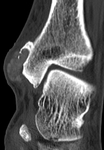
Case imaging findings: CT demonstrated an erosion with overhanging edge at the medial malleolus. The slight increased density of the soft tissue component suggests gouty tophus.
General imaging features of gout: Radiographs show normal bone density,
juxtaarticular erosions with "overhanging edge" and sclerotic margins. Tophi may be present as somewhat high density material. MR shows joint effusion with low T1 and high T2 signal. May have adjacent soft tissue/bone marrow oedema. Gouty tophus on MR have homogeneous intermediate T1 signal and enhance post contrast.
Tips: Gout is common!! Radiographs and CT are more helpful than MR. Look for tophi with juxtaarticular overhanging edge type erosions.
Fig.
16
Nora lesion/Bizzare Parosteal Osteochondromatous Proliferation (BPOP,
histologically proven).
Clinical: Left elbow mass in a young women.
Recurrent periosteal excision.
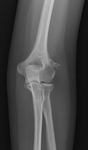
Case imaging findings: Left elbow radiograph demonstrated a cortical based exophytic outgrowth above the lateral epicondyle.
This was resected and histologically proven to be a Nora/BPOP lesion.
General imaging features of BPOP: Radiographs show a pedunculated or sessile surface mass that lacks periosteal reaction. CT shows the cortex and medullary space are not in continuity with the surface mass. MR is non-specific with variable signal on T1WI and high signal on fluid sensitive sequences. Heterogeneous signal post contrast.
Tips: Although the aetiology is thought to relate to trauma,
this benign lesion often occurs without a history of trauma.
It can be difficult to distinguish this lesion from an osteochondroma,
with the latter classically growing away from the joint.
If growth is toward the joint then consider a Nora lesion in the differential.
Histological diagnosis is often required to confirm the diagnosis and differentiate from osteochondroma.
Fig.
17
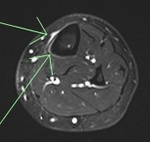
Periostitis ossificans (florid reactive periostitis,
histologically proven)
Clinical: 32 year old male with 4 year history of lumps on right tibia which had been progressively enlarging.
Case imaging findings: X-ray and CT showed a well defined surface based lesion with central soft tissue density surrounded by a thin calcified rim.
Some internal thin calcified septations perpendicular to cortex were evident.
Histology confirmed florid reactive periostitis (periostitis ossificans).
General imaging features of periostitis ossificans: Radiographs show periosteal reaction associated with a soft tissue swelling.
CT may reveal a benign appearing periosteal reaction and shows the lesion to be confined to the external cortex with preservation of the internal cortex.
On MRI however,
the appearance may be more aggressive with periosteal elevation,
oedema and enhancement of the adjacent soft tissue mass post contrast.
Tips: This lesion is a rare benign inflammatory process of the periosteum of uncertain aetiology (trauma has been proposed).
Awareness of this lesion and careful radiographic evaluation is required to help prevent unnecessary surgical intervention.
Fig. 18 & 19
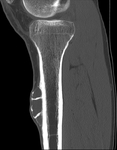
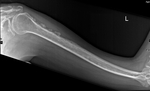
Voriconazole induced flourosis/ periostitis deformans
Clinical: 39 year old female underwent liver transplant secondary to autoimmune hepatitis.
Postoperative period complicated by Aspergillus infection requiring Voriconazole treatment.
The patient complained of widespread bone pain and myalgia.
Case imaging findings: X-ray showed a multifocal,
feathery periosteal reaction along the humerus.
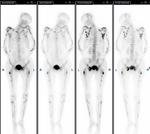
The whole body bone scan demonstrated multifocal predominantly appendicular skeletal uptake corresponding to the sites of periostitis with the low grade uptake in the skull due to recent surgery.
General imaging features of fluorosis: Osteoporotic or osteosclerotic metaphyseal dense lines.
Periosteal reaction is dense,
irregular and 'feathery'.
May be hyperaemic on bone scan with multiple foci of increased uptake on delayed images.
Tips: Triad of imaging findings is key in diagnosis of fluorosis- osteosclerosis,
osteophytosis and ligametous calcification.
In this case medication history is the key to diagnosis.
On bone scan pattern of uptake in the appendicular skeleton is atypical for metastases.
Flouride has a biological half life of 8 years thus improvement may be slow post cessation of offending agent.