Keywords:
Abdomen, Gastrointestinal tract, MR, Education, Diagnostic procedure, Inflammation
Authors:
G. Noe1, A. Galvin2, M. Goodwin1, S. Esler1; 1HEIDELBERG/AU, 2MELBOURNE/AU
DOI:
10.1594/ranzcr2014/R-0060
Results
- The assessment of disease activity is complex,
but vital for treatment planning and to guide the clinician in the use of immune-modulating,
biologic and surgical therapies.4,5
- Assessing disease activity and severity remains difficult as there is a lot of overlap between stages of disease activity.
Within individual patients,
and even within lesions,
active and inactive disease may co-exist.
Accurate assessment requires a combination of clinical,
biochemical,
endoscopic,
histological and radiological measures.5
- There are numerous tools to assess the disease activity,
including: Crohn’s disease activity index,
faecal calprotectin, ileocolonoscopy,
imaging,
surgery and histopathology.
- The role of imaging is ever increasing in the assessment of disease activity in Crohn's disease in which CT enterography/enteroclysis (CTE) and MR enterography/enteroclysis (MRE) play dominant roles.
The signs in the MR enterography and MR enteroclysis studies are the same.
CTE and MRE have similar diagnostic accuracies and imaging findings and can image areas of the small bowel that are difficult to reach with ileocolonoscopy.2,6
- MRI has become the preferred imaging modality as there is no ionising radiation involved.
It also allows multiplanar and dynamic interrogation,
has a high soft tissue contrast and has a high sensitivity of 88-89% and specificity of 78-100% for assessing disease activity.
1,2,7
The clinician wants to know:
- if there is active disease
- the location of disease,
and how much normal small bowel is present proximal to the diseased segment.
- the extent of the disease
- if there are strictures/stenoses
- presence of fistulas to adjacent organs
- if there are obstructions/adhesions
- about other complications e.g.
abscess formation
All these questions can be answered with an adequate MRI small bowel study.
We will now mainly focus on how to assess the disease activity (active versus inactive disease) through the assessment of common MRI signs seen in the different stages of disease activity in Crohn's disease,
illustrating the key findings with the use of numerous imaging examples from MRI small bowel studies.
Active versus inactive disease
There are many signs to look for on MRI when assessing disease activity,
but try and keep it simple and subdivide the disease into active (acute active or chronic active disease) versus inactive disease (fibrostenosing disease).1,2,4,5,8,9
1.
Active disease signs (acute/chronic):
Acute
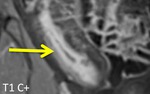
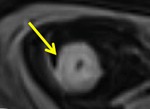
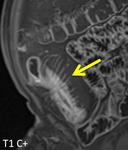
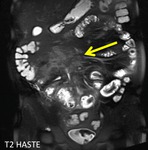
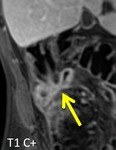
- Bowel wall thickening and edema in active inflammatory lesions (fig.1-3)
- Layered/stratified enhancement of the bowel wall (fig.4-7)
- Comb sign indicating mesenteric engorgement/hyperemia (fig.8 and 9)
- Mesenteric edema and enhancement (fig.10)
- Restricted diffusion (fig 11) 3,6,10
- (abscess/phlegmon) (fig.12)
Chronic (perforating)
- Deep ulcerations/sinuses/fistulas (fig.13,14,21-23)
- Fat halo sign (fig.15-17)
- Cobblestoning (fig.18)
- Fatty proliferation (fig.19 and 20)
2.
Inactive disease (signs):
- Fibrostenotic stricture (fig.24 and 25)
- Pseudosacculations (fig.26)
- Adhesions/obstructions (fig.27)
- Reparative stage (pseudopolyps and filliform polyposis) (fig 28)
As mentioned before,
there is a lot of overlap between the different stages of disease activity (fig 29).
We ideally look for multiple MRI signs that can be seen in the different stages of disease activity to help us decide if active disease is present.
The above described signs should merely be used as a guide to establish the activity, knowing and remembering that there is a lot of overlap and that lesions may show features of both active and inactive disease.1