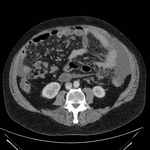
Acute Appendicitis
Acute appendicitis refers to acute inflammation of the appendiceal wall.
It is most common in adolescents and young adults but may occur at any age.
The presentation is more likely to be atypical in the very young and very old,
with the diagnosis made more difficult due to the increased likelihood of alternate diagnoses in these age-groups.
The lifetime risk of appendicitis is approximately 7%.
Most commonly,
the inflammed appendix is positioned retrocaecally.[3]
Pathogenesis
Acute appendicitis is thought to be caused by increasing intraluminal pressure compromising venous outflow,
leading to ischaemic injury,
bacterial perforation and neutrophilic infiltration.[4] Approximately 50-80% of cases are associated with overt luminal obstruction,
usually by a small stone-like mass of stool (“appendicolith”),
and less commonly a gallstone,
tumour or parasite (oxyuriasis vermicularis).[4]
Typical Clinical Features
- Periumbilical pain that later localises to the right lower quadrant.
- Nausea,
vomiting,
fever
- Elevated WBC
- Peritonitic tenderness at McBurney’s point (McBurney’s sign)
Up to a third of patients have atypical findings that may warrant radiological assessment.[2]
Secondary Appendicitis
Secondary appendicitis is caused by an adjacent inflammatory or infective process.
This may be due to causes such as caecal diverticulitis,
terminal ileitis,
active Crohn disease,
colitis or pelvic inflammatory disease.[5] CT findings may include a normal diameter appendix with adjacent fat stranding and possible appendiceal wall thickening.[6] Given the non-obstructive nature of such causes,
oral contrast may be used to demonstrate patency of the appendiceal lumen.
Correct prospective identification of the cause of the secondary appendicitis is crucial to avoid unnecessary appendicectomy,
as treatment is usually medical.[6]
TYPICAL ACUTE APPENDICITIS
Ultrasound
US is a fast,
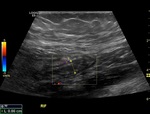
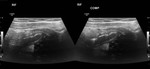
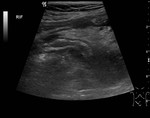
safe and cost-effective modality for evaluation of the appendix and is the most commonly used imaging modality to assess for appendicitis ( Fig. 1 ,
Fig. 2 ).[7] Ultrasound carries a sensitivity and specificity for detecting acute appendicitis of 71-97%.[8] Limitations of ultrasound include inter-operator variability and difficulty visualising the appendix due to high body-mass-index,
anatomical variation,
severe pain or overlaying bowel gas.[7] Ultrasound is the preferred imaging modality in paediatric,
pregnant and breast-feeding patients owing to its lack of ionising radiation.
US features in acute appendicitis may include:[9]
- Appendiceal diameter >6mm
- Appendiceal mural thickening
- Appendiceal wall hyperaemia on colour Doppler
- Intact echogenic submucosal layer (uncomplicated appendicitis)
- Presence of an appendicolith
- Adjacent hyperechoic fat
- Adjacent mesenteric lymphadenopathy
Computed Tomography
CT carries a sensitivity and specificity for diagnosing appendicitis of 83-98%.[7] Since the introduction of CT,
negative appendicectomy rates have decreased to <10%,
previously 21.5% in the pre-CT era.[7] Limitations of CT include cost,
ionising radiation and contrast reactions.
Relatively recent studies have shown comparable negative appendicectomy rates and perforation rates between low-dose CT protocols and standard CT protocols.[10]
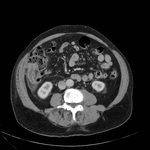
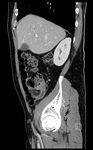
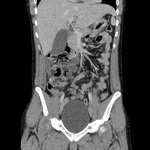
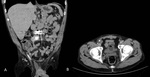
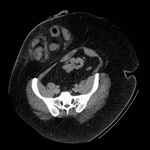
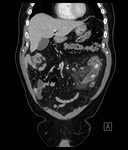
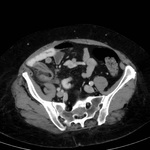
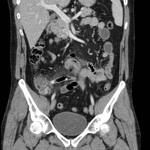
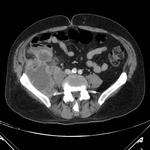
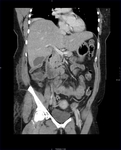
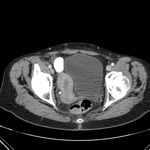
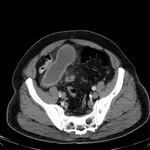
CT features of acute appendicitis ( Fig. 3 ,
Fig. 4 ) may include:[11]
- Appendix diameter >6 mm**^
- Appendiceal mural thickening**
- Appendiceal mural enhancement**
- Peri-appendiceal fat stranding**
- Focal caecal apical thickening
- Presence of an appendicolith
- Intramural air (pneumotosis)
- Extraluminal air
- Phlegmon
- Adjacent mesenteric lymphadenopathy
** Represent the four most useful signs for diagnosing appendicitis on CT.[11]
^ The original cut-off of >6 mm was an early extrapolation from ultrasound findings with application of right lower quadrant compression.
Some authors consider an appendiceal diameter on CT of 6-10 mm indeterminate,
as there is considerable overlap between the normal and abnormal appendix diameter.[12] Consequently,
appendiceal diameter on CT is best interpreted in the context of clinical and other CT findings.[12]
An increase in appendiceal caliber between serial CT examinations with supporting clinical features may signal early-stage acute appendicitis.
Oral contrast material within the appendix conflicts with a diagnosis of acute appendicitis and can be used as supporting evidence for a non-obstructed appendix.
Magnetic Resonance Imaging
MRI may be utilised in the paediatric or pregnant population,
in addition to ultrasound,
where the diagnosis remains uncertain.
One study demonstrated a sensitivity and specificity of 100% and 99% respectively when using an ultrasound – MRI pathway.[13] Limitations of MRI include cost,
availability and long scan times which may not be appropriate in the context of an acute abdomen.[7]
ATYPICAL ACUTE APPENDICITIS
Atypical Location
An atypical location of the appendix may give rise to an atypical clinical presentation ( Fig. 5 ,
Fig. 6 ).
For example,
the appendix may be contained within the inguinal canal (Amyand hernia [ Fig. 7 ]) or femoral canal (De Garengeot hernia) or be left-sided in malrotation or situs inversus ( Fig. 8 ).[5]
Stump appendicitis:
Stump appendicitis represents acute inflammation of an appendiceal remnant following appendicectomy.
This is due to inadvertent partial appendicectomy at the time of surgery.
Larger appendiceal stumps are associated with an increased risk of subsequent stump appendicitis.[6] CT findings in stump appendicitis involving a long stump remnant are similar to those in typical appendicitis,
with an inflammed blind-ended tubular structure associated with the caecum.[14] In the case of a short stump,
only secondary findings such as inflammation at the expected location of the appendix and localised caecal wall thickening may be present.[15] Stump appendicitis is associated with a higher likelihood of perforation (59%),
compared to primary acute appendicitis (17%),
possibly due to delays in diagnosis given the altered differential diagnosis in the setting of previous appendicectomy.[16]
Tip appendicitis:
Tip appendicitis describes an uncommon presentation where the inflammatory process is focally confined to the distal appendiceal tip ( Fig. 9 ).
In contrast to the imaging appearance of typical appendicitis,
the proximal portion of the appendix in tip appendicitis appears normal.
The true prevalence of tip appendicitis is unknown but has been cited to be up to 5% of appendicitis cases.[17] There is some evidence that a greater proportion of these cases can be managed conservatively compared to typical appendicitis.[18]
COMPLICATED ACUTE APPENDICITS
Gangrene,
Perforation and Abscess Formation
Delays in diagnosis of uncomplicated appendicitis may lead to the development of complications,
including the development of gangrene,
perforation ( Fig. 10 ) and abscess formation ( Fig. 11 ,
Fig. 12 ,
Fig. 13 ).
Gangrenous appendicitis is the result of arterial and intramural thrombosis.[12] Sonographically,
gangrenous appendicitis may be seen as a loss of the usually echogenic submucosal layer and absent colour flow on Doppler ultrasound.[9] CT evidence of gangrenous appendicitis includes pneumatosis,
an irregular appendiceal wall and patchy mural enhancement defects.[12]
Sonographic features suggestive of perforation include loculated pericaecal fluid,
hyperechoic pericaecal fat and circumferential loss of the submucosal layer.[9] On CT,
perforation is suggested by localised periappendiceal inflammation,
although this is non-specific.[12] The presence of appendicoliths increased the likelihood of perforation.[19] Horrow et al found the CT finding with highest sensitivity for perforation was a mural enhancement defect.[20]
Abscess formation is the most frequent complication of perforation.[12] Sonographically,
this may appear as a loculated fluid collection.
CT may demonstrate rim enhancement of the loculated fluid collection.
Treatment of large appendiceal abscesses by percutaneous drainage,
followed by delayed appendicetomy,
is a preferred treatment approach.[21]
Peritonitis
Early perforation of the appendix prior to formation of inflammatory adhesions may lead to bacterial peritonitis.[12] Appendicitis complicated by peritonitis tends to be more common in young children.[22] CT features include relatively diffuse free fluid,
mesenteric fat stranding,
engorged mesenteric vessels and enhancing thickened peritoneal reflections.[12]
Pyelophlebitis,
Pyelothrombosis and Hepatic Abscess
Haematogenous spread of infection along the draining portal venous system may lead to superior mesenteric and portal vein thrombosis,
infection and seeding of the liver with subsequent abscess development.
Hydronephrosis
Right sided hydronephrosis secondary to appendicitis which resolves on short-term follow-up imaging is a rare complication,
occurring in approximately 3.5% of patients with acute appendicitis.[23] It is associated with a retrocaecal location of the appendix and pregnancy.[23] Seventy-one percent of these patients have associated haematuria.[23]
Bowel obstruction
Rarely,
a peri-appendiceal inflammatory mass from appendicitis may lead to a mechanical obstruction of the terminal ileum.[12] More commonly,
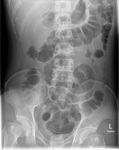
post-operative adhesions produce small bowel obstruction as a late complication of appendicectomy.[12] An acutely inflammed appendix may produce a localised ileus of adjacent bowel loops ( Fig. 14 ),
evident as adynamic bowel on ultrasound,
and as prominent loops on abdominal radiographs or CT.
APPENDICEAL MIMCS OF APPENDICITIS
Appendiceal neoplasms
Acute appendicitis is the most frequent clinical manifestation of appendiceal tumours,
occurring in 30-50% of patients [24],
however,
often the tumours may be overlooked on imaging.
Overall,
primary and secondary appendiceal neoplasms are found in approximately 1% of appendicectomy specimens.[25] The majority of these tumours consist of primary epithelial neoplasms and neuroendocrine tumours (NETs).
Primary Epithelial Neoplasms
Epithelial adenocarcinoma is the most common malignant primary appendiceal tumour ( Fig. 15 ).
There are mucinous and non-mucinous types (mucin evident radiologically and pathologically).
Epithelial neoplasms tend to be larger than NETs and are more likely to show peritoneal and metastatic spread.
Mucinous epithelial neoplasms:
Non-mucinous epithelial neoplasms:
- Less common than mucinous type.
- Manifest as focal soft tissue masses,
similar to colonic malignancies,
with possible regional lymph node involvement and metastases to the peritoneum,
liver or lung.[26]
Neuro-endocrine Tumours
- Represent 57-80% of appendiceal tumours (combining benign and malignant histological types).[25]
- May not be identifiable on imaging and are more often discovered incidentally on pathological examination post-operatively.
- Tend to be small and non-aggressive.
If detected,
they are often a small mass localised at the appendiceal tip.
Uncommonly they involve regional lymph nodes and rarely do they metastasise.
Other Tumours
- Are rare tumours of the appendix.
- Include lymphoma,
sarcoma,
metastatic disease to the appendix.
Summary of Modalities for Imaging Appendiceal Neoplasms
Ultrasound may detect secondary signs of appendiceal neoplasms such as a mucocele,
regional lymphadenopathy or ascites.
CT offers a sensitivity of up to 95% for detection of appendiceal tumours and is advantageous in its staging capability.[26] MRI is,
however,
the recommended modality for staging and follow-up of appendiceal carcinoma due to its higher sensitivity and specificity for detecting peritoneal spread.