2021 ASM / R-0013
Neuroimaging of patients presenting with first episode psychosis: a two-year retrospective review
Keywords:
Neuroradiology brain, CT, Audit and standards, Patterns of Care
Authors:
K. L. Yaxley; Adelaide, SA/AU
DOI:
10.26044/ranzcr2021/R-0013
Purpose
- Most current local and international clinical guidelines do not recommend neuroimaging should be used as a routine investigation of all patients presenting with a first-episode psychosis (FEP),1-4 although controversy persists5
- Imaging should only be performed if there is clinical suspicion of intracranial pathology, likely to be identifiable on imaging and known to be associated with psychosis, such as a space occupying lesion, infarction, infection (e.g. encephalitis or cerebral abscess), trauma, autoimmune disorders (e.g. lupus cerebritis) or metabolic disorders (e.g. Wilson Disease)
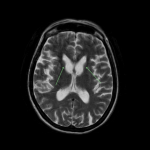
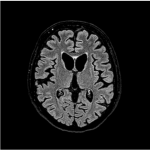
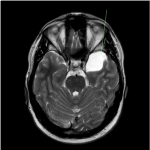
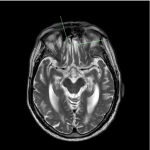
- Although there is some evidence that CT is comparable to MRI in detecting structural causes of FEP,6 MRI is recommended as the first line imaging modality, since it has better soft tissue contrast resolution with higher sensitivity for areas of interest (e.g. white matter changes, hippocampal changes and vascular pathology) and does not use ionising radiation (an important consideration given this patient group comprises a high prevalence of young adults)2,5
- The purpose of this work was to retrospectively review neuroimaging performed for all patients admitted with a first episode psychosis at a large mental health unit (Armadale Health Service, WA) to evaluate compliance with these guidelines and diagnostic yield