Purpose
Stereotactic radiosurgery (SRS) demonstrates excellent local control for melanoma brain metastases (MBM) in the order of 75-95% [1-4]. This study aimed to assess toxicity and local control outcomes in patients receiving combined modality immunotherapy and Gamma Knife® SRS for melanoma brain metastases at a single tertiary institution. Immunotherapy agents such as cytotoxic T-lymphocyte-associated protein 4 (CTLA-4) inhibitors, anti-programmed death 1 (PD-1) inhibitors and targeted therapy agents such as BRAF and MEK inhibitors (MEKi) have independently demonstrated various degrees of intracranial efficacy for metastatic melanoma [5-8].
Methods and materials
A retrospective single-institution analysis was performed of patients who received single- or multi-fraction Gamma Knife® SRS for melanoma brain metastases from January 2016 to June 2019. Predictive factors relating to patient age, gender, nature and timing of systemic therapy,BRAF status,treatment dose, baseline lesion size, number of lesions, development of new metastases in the follow-up period, extracranial disease status, baseline lactate dehydrogenase (LDH), baseline dexamethasone use and performance status were collected. SRS was delivered on the Gamma KnifePerfexionTMand ICONTMmodels. Brain metastases were treated without a margin...
Results
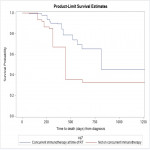
101 patients with a total of 435 melanoma brain metastases were treated with Gamma Knife stereotactic radiosurgery. Median follow-up was 29.2 months (IQR 19.7-39.8). Median dose was 20Gy (IQR 18-20) for single-fraction treatment and 24Gy/3# for multi-fraction SRS. Median cumulative GTV per patient was 2.3cc (IQR 1.1-5.1). There was a median of 3 lesions per patient treated (IQR 1-6). Baseline median individual lesion size was 0.24cc (IQR 0.96) and baseline median diameter was 0.77cm (IQR 0.76). 53% of patients were BRAF mutant with 65% having...
Conclusion
This study demonstrates combined modality immunotherapy and SRS provides a high degree of local control for melanoma brain metastases with a low rate of symptomatic RN. There was no significant association between concurrent systemic therapy use and the development of symptomatic RN outcomes.
References
Long, G.V., et al., A randomized phase 2 study of nivolumab and nivolumab combined with ipilimumab in patients (pts) with melanoma brain metastases: The Anti-PD1 Brain Collaboration (ABC Study). 2016, American Society of Clinical Oncology.
Tawbi, H.A., et al., Combined nivolumab and ipilimumab in melanoma metastatic to the brain. 2018. 379(8): p. 722-730.
Lehrer, E.J., et al., Treatment of brain metastases with stereotactic radiosurgery and immune checkpoint inhibitors: an international meta-analysis of individual patient data. 2019. 130: p. 104-112.
Petrelli, F., et al., Combination of...