Type:
Educational Exhibit
Keywords:
CNS, Neuroradiology brain, Vascular, CT, CT-Angiography, Thrombolysis, Embolism / Thrombosis
Authors:
T. Skalina, B. Travers, R. Grimley, S. Dupre; Sunshine Coast, QLD/AU
DOI:
10.26044/ranzcr2021/R-0315
Background
CVT encompasses both thrombosis of the cortical or deep cerebral veins and dural venous sinuses.1,2 It is an uncommon cause of stroke, accounting for 0.5-1% of all adult population strokes.1,3 Contemporary stroke treatment emphasizes time to intervention as a major determinant of patient outcomes. The diagnosis of CVT is challenging owing to its rarity, varied clinical presentation and often subtle radiological features. These factors combined with the time critical nature of stroke, may lead to CVT being overlooked on initial rapid CT stroke imaging (NCCT/CTA/CTP) and result in institution of incongruous empirical management for assumed arterial stroke.
Radiologists play a crucial role in early diagnosis of CVT, thus influencing patient outcome. We present a case of CVT, clinically and radiologically masquerading as acute arterial stroke.
Case
A 61-year-old male with no known previous medical history awoke from sleep at 0200 with headache and right-sided weakness. At initial assessment he had right arm weakness and incoordination, right sided visual and sensory neglect, and fluent aphasia. His National Institute of Health Stroke Scale (NIHSS) score was 5. Stroke imaging, including NCCT followed by CTP of the brain and CTA of the neck and cranial vessels was performed.
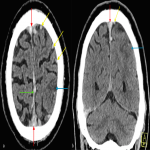
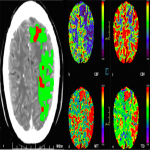
NCCT demonstrated gyral swelling, loss of grey-white matter differentiation and hypodensity involving the left superior parietal lobe and mild gyral swelling of the left frontal lobe. Automated CTP processing (using MIStar) calculated a 12 mL core infarct and 78mL area of relative ischaemia corresponding to left anterior cerebral artery (ACA) and left middle cerebral artery (MCA) territories. The CTA showed normal opacification of the intra- and extra-cranial arterial vessels.
Acute arterial stroke was diagnosed on the basis of the clinical presentation and CTP imaging. Thrombolysis was administered using tenectaplase 0.25 mg/kg. Clinical deterioration several hours later warranted repeat NCCT of the brain showing an acute left intraparenchymal haemorrhage. Following intensive rehabilitation the patient progressively recovered to independent function with a final modified Rankin Scale of 1 and NIHSS of 0. A prothrombotic screen was performed. A genetic panel for thrombophilia identified heterozygosity for a prothrombin gene variant 20210G>A. The patient was placed on lifelong anticoagulation.
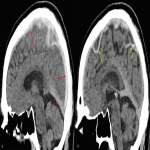
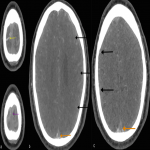
On retrospective review of the NCCT acute thrombus can be seen as a hyper-attenuating superior sagittal sinus, known as the “filled delta” sign (Figure 1). The tributary surface cortical veins draining into the superior sagittal sinus are seen as engorged, hyperdense, linear/serpiginous, left sided cortical veins known as the “cord” sign (Figure 1). There is dural thickening and enhancement of the falx secondary to venous stasis and hyperaemia (Figure 1). The “empty delta” sign is evident on contrast enhanced CT with dural wall enhancement of the superior sagittal sinus and a complete filling defect within this (triangular shaped) dural venous sinus (Figure 4). On CTP, the perfusion abnormality appears to involve two arterial territories (left ACA and left MCA). This may be the result of left internal carotid artery emboli however the distribution at the vertex, adjacent to the superior sagittal sinus and draining cortical veins along with the normal CTA findings are a useful clue to the CVT aetiology on CTP (Figure 3).