Results
A total of 681 scans (616 Chest X-Rays, 59 CTs, 6 V/Q) from 181 patients was reviewed. Of the 181 patients, there were 92 females and 89 males with a mean age of 61.99 (range 16-101).
Chest Radiograph Findings
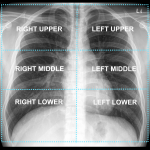
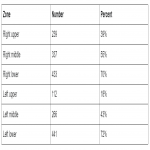
103 (17%) of radiographs performed were normal with no findings. 3 chest radiographs were considered not suitable for evaluation as they did not have the entire chest in view for evaluation. The most commonly involved zones were the left lower zone (n = 441, 72%) and right lower zone (n = 433, 70%). The least involved zone was the left upper zone (n = 112, 18%). The distribution in each lung zone is shown in Table 1. Findings in both lungs (n = 417, 67%) were demonstrated more often than unilateral findings (n = 239, 39%). The most common pattern of distribution was a diffuse pattern (n = 351, 57%) followed by a peripheral pattern (n = 146, 24%) with the least common pattern of distribution being central (n = 13, 2%). In the other findings evaluated, 3% had pleural effusions and 3% has interstitial changes.
CT Findings
Of the 59 CTs, 9 were performed as follow up after the acute episode. 10 (17%) CTs performed were normal with findings of which 2 were in the follow up CT scans. 33 of the scans were CT pulmonary angiograms, with 5 positive for a pulmonary embolism. The most common patterns demonstrated on CT imaging were ground glass opacity (n = 20, 45%) and ground glass with consolidation (n = 20, 34%). The most common patterns demonstrated on CT imaging were peripheral (n=29, 49%) and peribronchovascular (n =16, 27%). The most commonly involved lobe was the right lower lobe (n = 42, 71%) followed by the left lower lobe (n= 41, 69%). Bilateral involvement (n=45, 76%) was more common than unilateral involvement (n = 3, 6%). In the other findings evaluated, 4 demonstrated pleural effusion (n=4, 7%), 2 cases demonstrated lymphadenopathy and 5 cases demonstrated pulmonary nodules. Scarring was observed in 3 cases, 2 of which were in follow up CT scans. An example CT demonstrating peripheral regions of consolidation, ground glass and air bronchograms is shown in Figure 4.
V/Q Findings
Of the 6 V/Q scans performed, 2 (33%) demonstrated findings and 4 (67%) were normal. One V/Q scan was performed 7 days prior to the positive COVID test and 4 days prior to the onset of symptoms to investigate a 6 month history of chest pain. The V/Q scan was negative for pulmonary embolism with bronchopulmonary changes seen in the left apex on both ventilation and perfusion images(Fig. 5). Although CT chest two days later demonstrated no correlative changes, bilateral regions of opacification were subsequently demonstrated on CXR 7 days after the V/Q scan. One other V/Q scan was for follow up of pulmonary emboli demonstrated on the initial CT pulmonary angiogram on admission demonstrating mild heterogeneous tracer distribution in both lung fields.
Evaluation of readers
Moderate agreement was demonstrated between the readers for assessment of distribution on the chest radiograph (peripheral, central, diffuse) with a Fleiss Kappa value of 0.42 (p-value < 0.05). The Fleiss Kappa values of the inter-rater agreement for the distribution of the opacities in zones ranged from fair to substantial agreement with Fleiss kappa values ranging from 0.29 - 0.73 (p-value < 0.05).
A qualitative assessment performed on the CTs read by all consultant radiologists demonstrated consistency in labelling of the lobe involvement. There was a general consensus for the presence of ground glass opacity, air bronchograms and ground glass with consolidation.