CNS lymphoma
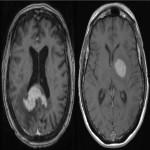
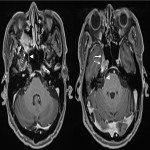
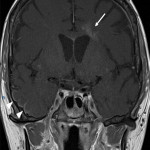
Lymphoma can involve the CNS in isolation (primary CNS lymphoma, PCNSL) or as part of more extensive systemic disease (secondary CNS lymphoma, SCNSL). PCNSL typically involves the brain parenchyma[2], most commonly as a single lesion, though multiple lesions occur in 20-40% of patients[3,4]. The cerebral hemispheres, corpus callosum and deep grey nuclei are the most common sites involved[5] (Figure 1).
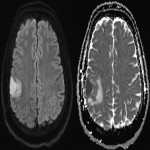
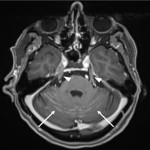
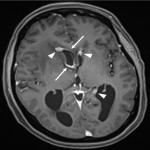
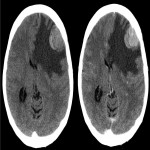
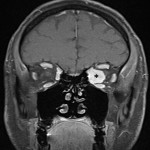
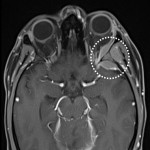
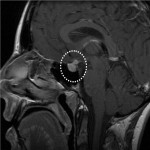
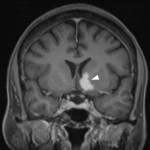
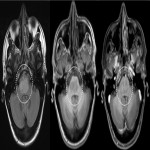
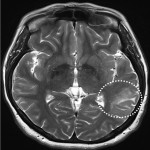
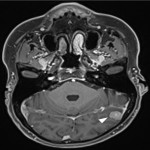
Lesions usually contact the cerebrospinal fluid spaces, but radiologically evident leptomeningeal involvement is uncommon[4-6]. Characteristically, lesions demonstrate hyperdensity on pre-contrast CT and diffusion restriction on DWI, related to dense cellularity, and avid post-contrast enhancement. SCNSL also usually involves the parenchyma[7] (Figure 2), with similar appearances to PCNSL[2,3], but leptomeningeal involvement is relatively more common[2] (Figures 3 & 4).
Neurolymphomatosis and intravascular lymphoma are two uncommon manifestations of CNS lymphoma. Neurolymphomatosis represents isolated nerve infiltration by neoplastic cells[8] (Figure 5), while intravascular lymphoma reflects intraluminal proliferation of clonal lymphocytes within small vessels, with heterogeneous MRI appearances including infarct-like lesions, nonspecific white matter lesions, enhancing masses, meningeal enhancement and T2-hyperintense lesions in the pons[9].
Granulocytic sarcoma
Granulocytic sarcoma, previously known as chloroma, represents an extramedullary mass of leukaemic cells, most commonly in the context of acute myeloid leukaemia (AML). Lesions can involve the brain parenchyma (Figure 6), meninges, nerves and adjacent tissues[10]. Imaging features in the CNS are similar to those occurring in lymphoma, including pre-contrast hyperdensity on CT, diffusion restriction and avid post-contrast enhancement[10].
Multiple myeloma
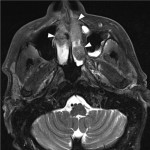
Intracranial manifestations of multiple myeloma (MM) include discrete extraosseous plasmacytomas (e.g. in the orbit or paranasal sinuses) (Figure 7), dural invasion from calvarial plasmacytomas (Figure 8), leptomeningeal involvement and, very rarely, CNS parenchymal involvement[11,12]. Similar manifestations may be seen in the spine, including expansion of plasmacytomas into the central vertebral canal, with the potential for spinal cord or cauda equina compression, and leptomeningeal disease[13].
Bing-Neel syndrome
Bing-Neel syndrome is a very rare complication of Waldenstrӧm macroglobulinaemia, characterised by direct CNS involvement by malignant lymphoid cells[14]. Abnormal leptomeningeal enhancement is the most common imaging feature (Figure 9), occurring in 71% of patients in a recent series[15]. Brain parenchymal involvement, characterised by nodular or ring-enhancement, occurred in 42% of patient in this series, while the dura was involved in 38% and the orbit in 16%[15].
Histiocytoses
The histiocytoses are characterised by the accumulation of malignant cells derived from monocytes and macrophages, or their derived cell lineages[16]. Langerhans cell histiocytosis affects the pituitary gland in 25% of patients (Figure 10) and the remainder of the CNS in 2-4%[16]. Manifestations of CNS involvement include tumour infiltration (Figure 11) and degenerative lesions [16].
Erdheim-Chester disease affects the CNS in 15-37% of patients[16]. The CNS manifestations are similar to Langerhans cell histiocytosis, namely tumoural (Figure 12) and degenerative lesions, with the addition of intracranial vascular infiltration, which can cause ischaemic strokes[16].
Rosai-Dorfman disease involves the head and neck in 22% of patients, most commonly the nasal cavity (Figure 13) followed by the pituitary gland, while intracranial involvement is uncommon[16].
Opportunistic infections
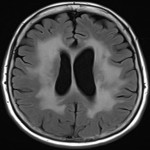
Treatment for haematological malignancies typically involves immunosuppression, thus conveying a risk of opportunistic infections. These may demonstrate characteristic features depending on the organism, such as punctate T2-hyperintensities in PML (progressive multifocal leukoencephalopathy) [17] (Figure 14), or more general features of cerebral abscess such as central diffusion restriction.
Late post-treatment effects
Chemotherapy and radiotherapy are commonly administered for haematological malignancies. Neurotoxicity from chemotherapy can occur acutely, for example posterior reversible encephalopathy syndrome (PRES)[18,19], or further down the track, in particular methotrexate-induced leukoencephalopathy (Figure 15). Radiotherapy may result in white matter changes, radiation-induced neoplasms (Figure 16) and cavernomata[20].