Purpose
1. To determine the time course and degree of liver hypertrophy resulting from portal vein embolisation (PVE).
2. To ascertain the complication rate of PVE.
Methods and materials
Hepatic tumours such as colorectal liver metastases and cholangiocarcinoma may be treated with hepatic resection. A sufficient volume of residual liver, or future remnant liver (FRL) after resection, is required to avoid complication of liver failure, which is a major cause of death following liver resection. The aim of PVE is to hypertrophy the FRL in patients with insufficient FRL to allow surgical resection of the affected liver lobe [1, 2, 3].
A retrospective analysis of prospectively collected data on all patients who underwent PVE...
Results
Patient Data:
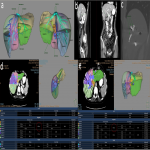
36 patients underwent PVE between 2009 and 2021 prior to planned liver resection. 11 patients were excluded from the study due to incomplete data as the liver volumetry CT was either performed externally and unable to be retrieved. Of the remaining 25 patients, 12 were female and 13 were male, with an average age of 59 (ranging from 29 to 74 years old).
[Fig 1]
Choice of Embolisation Material:
Embolisation was performed using polyvinyl alcohol particles (PVA) and coils in 17 patients (except...
Conclusion
PVE is a safe and effective procedure in inducing hypertrophy of the future remnant liver (FRL) preoperatively. In our series, right PVE resulted in adequate hypertrophy of the FRL in 83% of the cases, with a mean increase in volume of the FRL of 35% at an average of 30 days.No significant complications were encountered.
References
Denys A, Prior J, Bize P, et al. Portal Vein Embolization: What Do We Know? CardioVascular and Interventional Radiology. 2012;35(5):999.
Vyas S, Bent C, Partelli S, et al. Portal Vein Embolisation for Extended Hepatectomy: Single-Centre Experience. Journal of Gastrointestinal Cancer. 2012;43(3):413.
van Lienden KP, van den Esschert JW, de Graaf W, et al. Portal Vein Embolisation Before Liver Resection: A Systematic Review. CardioVascular and Interventional Radiology. 2013;36(1):25.