Keywords:
Oncology, Urinary Tract / Bladder, MR, Ultrasound, Biopsy, Cancer
Authors:
S. J. Pattiarachchi, W. Thambavitage, M. Lozinskiy, Y. Yuminaga, Y. Weerakkody; Perth, WA/AU
DOI:
10.26044/ranzcr2021/R-0469
Purpose
Prostate cancer causes significant morbidity to the elderly male population.
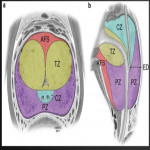
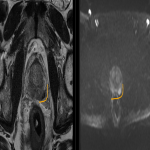
In those with clinical concern for prostate cancer, MRI is often used as a preferred method for initial detection of a specific lesion prior to tissue sampling (e.g. see figure below).
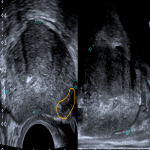
Once such a lesion is detected, image-guided biopsies can be performed either with ultrasound (free-hand or with grid) or with MRI. A corresponding lesion can sometimes be visible on ultrasound although overall detection sensitivity for lesions on ultrasound is low.
If no lesion is detected, a systematic non-targeted set of biopsies can still be performed if there are sufficient clinical grounds.
When using ultrasound-guided freehand biopsies (currently used in our institution), there are 3 broad strategies in carrying out a biopsy; which are:
- A targeted biopsy of a pre-detected lesion (usually with preceding MRI).
- Systematic sampling without prior diagnostic imaging.
- Combination of above (mostly targeted biopsies but with additional random systematic sampling through the prostate elsewhere)
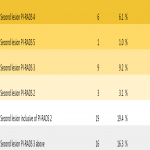
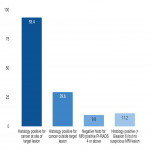
The justification for "additional" random (non-targeted) sampling even in those with a distinct MR detected lesion is the probability of radiologically occult tumour sites elsewhere in the prostate gland.
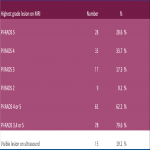
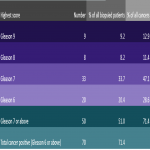
The purpose of this study was to analyse histology results of targeted (with respect to MRI detected location) vs additional non-targeted systematic sampling as well as to assess the yield of cancer in additional systematic samples even in those with an index MR detected lesion.