Purpose
Image guided percutaneous renal biopsy is the principal investigation in achieving a histological diagnosis of kidney diseases. However, renal biopsies carry significant risk of complications, due to extensive renal vascularity [1, 2].
At our regional secondary centre, the choice of image guidance modality, either CT or US, is made by booking staff without a clear selection process. There is a relative lack of consensus demonstrating outcomes based on selection of imaging guidance. CT is potentially selected as first line in those patients who are obese...
Methods and materials
A quantitative clinical audit of image guided renal biopsies was performed for biopsies conducted at a regional hospital between 1st of January 2018 and 30th of June 2021.
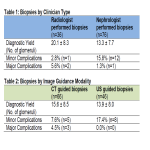
Diagnostic yield, measured in average number of glomeruli, and safety, measured in frequency of major and minor complications, were compared based on clinician type, either nephrologist or radiologist, and choice of image guidance, either CT or US. Major complications were defined as those requiring intervention such as arterial coil embolisation or blood transfusion.
Results
112 encounters of 99 unique patients were included, of these, 53 patients were male and 46 were female. The median age was 45.8 years (range 15-84 years).
Clinician Type:
Radiologist performed biopsies (n=36) yielded a mean of 20.1 ± 8.3 glomeruli, compared with nephrologist performed biopsies (n=76) which yielded a mean of 13.3 ± 7.7 glomeruli (p=0.001). All radiologist biopsies were considered adequate by pathologists, compared with 86.8% of nephrologist performed biopsies.
Radiologists experienced a rate of minor complications of 2.8% (n=1) and major complications...
Conclusion
When comparing approaches to biopsies, radiologists demonstrated a statistically significant, higher diagnostic yield and lower rate of minor complications, but a higher rate of major complications than nephrologists.
There was no significant difference in measures based on choice of imaging modality. Discussions on selection of image guidance and collaboration between specialty groups to improve patient outcomes are ongoing.
References
Hogan JJ, Mocanu M, Berns JS. The native kidney biopsy: update and evidence for bestpractice. Clin J Am Soc Nephrol. 2016;11(2):354-362. doi: 10.2215/CJN.05750515
Whittier WL, Korbet SM. The kidney biopsy. In: Glassock RJ, Rovin BH, eds. UpToDate.UpToDate; 2021. Accessed February 1, 2022. https://www.uptodate.com/contents/the-kidney-biopsy#topicContent