Imaging features
Abnormal features of peripheral nerves include increased signal on fluid sensitive imaging and increased cross-sectional area of the nerve. Denervation muscle oedema is an important secondary feature of entrapment neuropathies [11]. An additional technique which is increasingly investigated in MR neurography is diffusion tensor imaging (DTI) [12]. This technique allows accurate visualisation of nerves by means of their fractional anisotropy (FA) and microstructural properties [12,13]. Pathologic conditions of peripheral nerves lead to decreased FA values [12]. Features of high-resolution ultrasound such as increased cross-sectional area and decreased echogenicity are useful indicators of pathology [14].
Normal anatomy
The lumbosacral plexus provides motor and sensory innervation to the pelvis and lower limb [15]. This is comprised of a lumbar and sacral plexus. The lumbar plexus is formed from the anterior rami of L1-L4 nerve roots with occasional contribution from T12 [16]. The sacral plexus is formed from the anterior rami of L4-S4 nerves [16]. The two plexuses are connected by the lumbosacral trunk, formed by the L4 and L5 nerve roots, to form the lumbosacral plexus [16].
Specific nerves
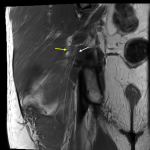
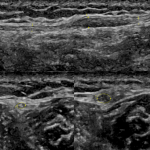
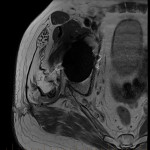
The sciatic nerve arises from the L4 to S3 nerve roots' ventral divisions and leaves the pelvis through the greater sciatic foramen at the inferior border of the piriformis muscle [15,17]. Entrapment of the sciatic nerve can occur in the hip region and less commonly in the thigh. The various causes include fibromuscular entrapment, trauma and extrinsic compression from space-occupying lesions [9,11,18]. Piriformis syndrome, a rare entrapment neuropathy is a controversial diagnosis (Figure 1), with no consensus regarding the diagnostic criteria, and this entity remains a diagnosis of exclusion [14,19,20].
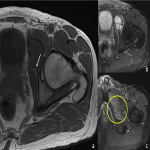
The obturator nerve arises from the ventral L2-L4 rami of the lumbosacral plexus and descends along the iliopectineal line and exits the pelvis via the obturator canal at the superior aspect of the obturator foramen [11]. The nerve is most commonly entrapped in the obturator canal. The most common causes of entrapment include pelvic trauma, periarticular cysts, perilabral cysts or obturator hernia [11,15,21]. Rarely entrapment can occur from space-occupying lesions (Figure 2) [11,15,21].
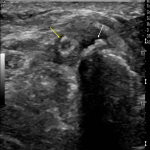
The lateral femoral cutaneous nerve is a sensory nerve arising from L2 to L3 and supplies the anterolateral thigh. It emerges from the lumbar plexus on the lateral aspect of the psoas and descends obliquely on the anterior surface of the iliacus muscle. It exits the pelvis deep to the inguinal ligament and medial to the anterior superior iliac spine [15]. Entrapment typically occurs as the nerve travels inferior to the inguinal ligament or as it pierces the fascia lata [22,23]. There are multiple causes of entrapment, including trauma, iatrogenic, external compression from space-occupying lesions (Figure 3) and compression from tight clothing [24–26].
The intrapelvic course of the nerve is not readily demonstrable on imaging. The extra-pelvic course of the nerve can be visualised on MRI and US.
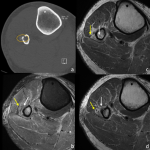
The common peroneal nerve arises from the sciatic nerve at the superior aspect of the popliteal fossa. It travels distally posteromedial to the short head of the biceps femoris and superficial to the lateral head of the gastrocnemius muscle. The nerve then wraps around the fibular neck before entering the peroneal tunnel between peroneus longus and the fibula, where it divides into the superficial and deep peroneal nerves. Common peroneal neuropathy is the most common mononeuropathy in the lower limb [2]. The two most common sites of entrapment are, as it crosses the fibular neck, given its superficial location, and as it travels deep to the peroneus longus muscle [2]. Entrapment can occur from external compression, intraneural ganglion from proximal tib-fib joint or traumatic injury (Figure 4) [2,23].
.
Superficial peroneal nerve can be entrapped as it courses through the leg fascia
whilst deep peroneal entrapment associated with midfoot osteophytes, ganglia or scarring from prior ankle surgery
.
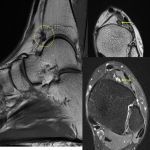
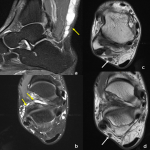
The tibial nerve arises from the sciatic nerve and descends into the posterior compartment of the lower leg deep to the soleus, plantaris, and gastrocnemius muscles. It then enters the tarsal tunnel, which is formed by the calcaneus, talus, medial malleolus and the flexor retinaculum. Tibial nerve neuropathy is also called tarsal tunnel syndrome and is caused by compression of the tibial nerve at the tarsal tunnel [29]. Common aetiologies of tarsal tunnel syndrome include posttraumatic fibrosis, fracture, and tenosynovitis [30]. Entrapment can also occur from external compression from space-occupying lesions such as ganglion cysts, and anomalous muscles (Figure 5) [2,30].
Foot deformities have also been implicated, including hindfoot valgus and less commonly with forefoot pronation, pes planus, and tarsal coalition [2,30].
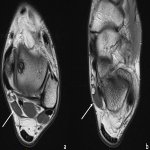
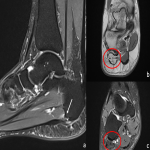
The medial plantar nerve arises from the tibial nerve at the tarsal tunnel. It crosses to the mid-foot at the level of the talonavicular joint through the deep fascia of the abductor hallucis muscle to enter the medial plantar tunnel [29]. Entrapment can occur at the tarsal tunnel or distal to it (depending on where it originates) or at the level of the knot of Henry, which is between the navicular tuberosity superiorly and the abductor hallucis muscle belly inferiorly. Entrapment at the level of the knot of Henry commonly occurs in runners and is called “Jogger’s Foot" (Figure 6) [2,31,32].
Other causes include extrinsic compression from space-occupying lesions, tenosynovitis of adjacent tendons, and structural foot abnormalities [32].
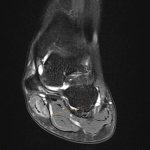
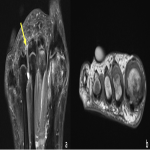
The medial plantar nerve terminates as the digital hallux nerve and the common digital nerves for the second, third, and medial fourth digits. The lateral plantar nerve provides the digital nerve for the fifth toe and the common digital nerve for the fourth and fifth digits. The digital nerves travel in narrow fibro-osseous tunnels formed by the metatarsal heads and intermetatarsal ligaments [29]. Entrapment of the digital nerves occurs in the intermetatarsal space between the metatarsal heads, plantar to the intermetatarsal ligaments [33]. The entrapment leads to perineural fibrosis of the digital nerve, a condition known as Morton’s neuroma (non-neoplastic) (Figure 7) [34].
. The most common nerves that are affected are the second and third common digital nerves. This is thought to be due to the second and third intermetatarsal spaces being narrower compared to the first and fourth spaces [35]. Additionally, the third common digital nerve is thicker due to its dual origin from the lateral and medial plantar nerves, this also tethers the nerve with less longitudinal mobility during dorsiflexion [36].
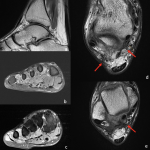
The lateral plantar nerve arises from the tibial nerve in the distal tarsal tunnel. Entrapment can occur at the tarsal tunnel or distal to it [37]. The aetiology of entrapment includes external compression from space-occupying lesions, tenosynovitis, and fibrosis of the tarsal tunnel (Figure 8) from prior injury and insult [37]
. A clinically important branch of the lateral plantar nerve is the first branch, the
inferior calcaneal nerve. Entrapment of this nerve, called Baxter Neuropathy, can occur at three sites, deep to or adjacent to the fascial edge, along the medial edge of the quadratus plantae muscle, and adjacent to the medial calcaneal tuberosity [2,38].
.
The sural nerve is a pure sensory nerve. It is formed by the joining of the medial sural nerve (branch of the tibial nerve) and the lateral sural cutaneous nerve (branch of the common peroneal nerve) at the level of the mid-leg. The nerve courses downward between the two heads of the gastrocnemius and pierces the deep fascia in the upper calf. More distally, it courses along the posterolateral aspect of the leg, behind the lateral malleolus and along the lateral aspect of the foot [23,39]. The nerve supplies sensation to the lateral aspect of the ankle and foot up to the base of the fifth toe [2]. The aetiology of entrapment includes trauma, iatrogenic causes and external compression from space-occupying lesions (Figure 10) [40–42]. There is no denervation oedema as the nerve is purely sensory [23].