Learning objectives
Highlight and raise awareness of the common imaging findings and diagnostic challenges of heterotopic pregnancy.
Background
Heterotopic pregnancy is a rare entity but with potential for significant morbidity and mortality. It is defined as a condition that involves a simultaneous intrauterine and extrauterine pregnancy. Prevalence ranges from 1:30000 in the general population to 1:100 in the context of assisted reproduction (1,2). Anecdotally, in our institution, we have experienced an increasing incidence of heterotopic pregnancies with varying imaging and clinical presentations. This may be due to increasing use of assisted reproductive techniques, fertility or ovarian factors (3). The diagnosis of heterotopic pregnancy...
Imaging findings OR Procedure details
CASE 1
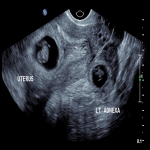
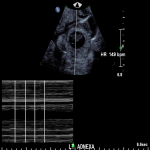
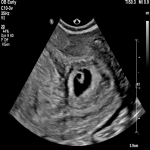
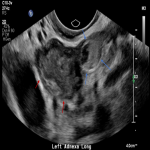
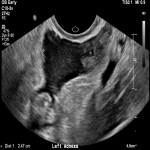
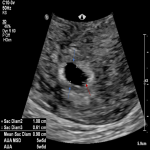
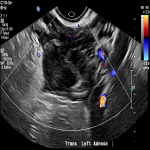
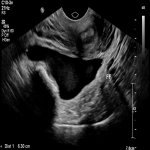
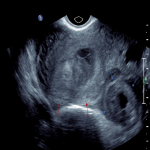
A 32-year-old femalepresented to the emergency department with per vaginal bleeding, lower abdominal pain and a positive beta HCG. Ultrasound imaging demonstrated a live intrauterine gestation with an estimated gestational age of 8 weeks. A further gestational sac with a live foetus was demonstrated within the left adnexa. A small perigestational haemorrhage was also noted adjacent to the intrauterine gestational sac (Fig 1-2).
A left salpingectomy was performed without complication, and subsequently the intrauterine pregnancy was uneventful with natural delivery of a healthy...
Conclusion
The successful recognition of heterotopic pregnancy begins with the awareness of its imaging features and understanding of the diagnostic challenges. A normal live intrauterine gestation should not preclude close examination of the adnexae. Early diagnosis and treatment is important to limit adverse outcomes.
References
Dibble EH, Lourenco AP. Imaging Unusual Pregnancy Implantations: Rare Ectopic Pregnancies and More. AJR Am J Roentgenol. 2016 Dec;207 (6):1380-1392.
Talbot K, Simpson R, Price N, et al. Heterotopic pregnancy. J Obstet Gynaecol 2011;31: 7–12.
Hewlett K, Howell CM. Heterotopic pregnancy: Simultaneous viable and nonviable pregnancies. JAAPA. 2020 Mar;33 (3): 35-38.
Bickell NA, Bodian C, Anderson RM, Kase N. Time and the risk of ruptured tubal pregnancy.Obstet Gynecol.2004;104:789–94.
Busby LP, Courtier JL, Glastonbury CM. Bias in Radiology: The How and Why of Misses and Misinterpretations....