Purpose
Paediatric stroke is an acute condition that is frequently delayed in its diagnosis and associated with significant lasting morbidity[1-4]. Current guidelines suggest the establishment of immediate response protocols may reduce diagnostic delays of paediatric stroke and facilitate timely access to reperfusion therapies[5-9]. Our tertiary paediatric institution sought to quantify the potential demand that an acute stroke protocol would place upon the imaging department and examine the current access to imaging services of patients who met criteria.
Methods and materials
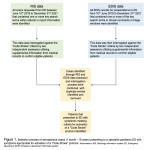
A retrospective observational cohort study was conducted on patients aged 1 month to 18 years presenting with symptoms of an acute atraumatic intracranial event to a specialist tertiary paediatric hospital emergency department (ED) over a 3.5-year period from June 2018 to end of 2021 (Figure 1).
An analysis of the radiology department information system was performed to identify scans requested through the ED during the time period that contained key terms within the referrals and/or report text (Table 1). These presentations were interrogated against criteria...
Results
Sixty children (33 female/ 27 male) presented to ED with symptoms that met acute stroke protocol activation criteria with a mean age of 10.3 years (SD 3.8). Forty-three (72%) children underwent urgent imaging in ED (35 computed tomography [CT], 8 Magnetic Resonance Imaging [MRI]), with twenty-one (49%) scans being performed out-of-hours (CT 19, MRI 2) (Figure 2).
Fourteen positive findings were noted (6 haemorrhagic strokes, 5 acute ischaemic stroke [AIS] and 3 other neurological causes). Median time for imaging to be performed after ED presentation...
Conclusion
This study highlighted that in a paediatric setting without an acute stroke protocol, 70% of patients presenting to the ED with symptoms warranting activation of such a pathway received urgent imaging. While these images were acquired promptly after referral, the need for earlier recognition of paediatric patients with acute neurological symptoms in the ED setting was highlighted. For patients with AIS, imaging was performed within the guideline recommended therapeutic window for thrombectomy of 6 hours.
References
Mallick AA, Ganesan V, Kirkham FJ, Fallon P, Hedderly T, McShane T, et al. Diagnostic delays in paediatric stroke. J Neurol Neurosurg Psychiatry. 2015;86(8):917-21.
Srinivasan J, Miller SP, Phan TG, Mackay MT. Delayed recognition of initial stroke in children: need for increased awareness. Pediatrics. 2009;124(2):e227-34.
Perkins E, Stephens J, Xiang H, Lo W. The cost of pediatric stroke acute care in the United States. Stroke. 2009;40(8):2820-7.
deVeber GA, Kirton A, Booth FA, Yager JY, Wirrell EC, Wood E, et al. Epidemiology and Outcomes of Arterial...