Keywords:
Contrast agents, Genital / Reproductive system female, Veins / Vena cava, Fluoroscopy, Contrast agent-other, Health policy and practice, Hysterosalpingography, Education and training, Obstruction / Occlusion, Quality assurance
DOI:
10.26044/ranzcr2022/R-0089
Methods and materials
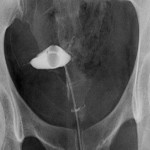
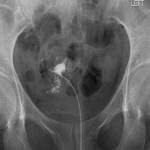
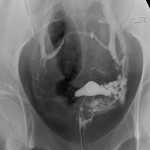
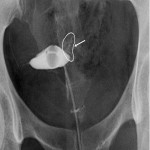
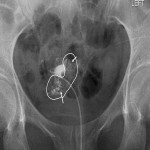
Intravasation on HSG is defined by the flow of injected contrast from the uterine cavity into adjacent myometrial vessels (usually the veins).[1] Intravasation events can affect safe usage of contrast mediums in HSGs and have implications on periprocedural symptoms for patients. Additionally, severe intravasation can cause an image artefact, obscuring tubal filling and affecting the diagnostic quality of HSGs.[2]
A novel classification system has been proposed in 2013 to grade intravasation severity based on regional spread; however, no standardized grading prevails in everyday clinical practice.[3]
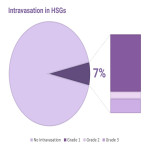
Reported prevalence ranges from 0.4% to 13%, with higher rates reported in oil-soluble contrast medium (OSCM) compared with water-soluble contrast medium (WSCM).[4] Recent evidence of OSCM’s fertility-enhancing benefits has prompted rapid clinical uptake by fertility specialists throughout the world.[5] This growing interest in utilising OSCMs in HSGs may have implications for patient safety given intravasation has been reported to cause embolisms.[6] In recent literature, serious consequences such as cerebral and retinal embolisms have resulted from oil intravasation in patients undergoing HSGs for infertility. However, adverse events are poorly recorded across studies.[7] This instigates an increased concern towards intravasation risk and warrants further research to understand intravasation and its associated sequelae.
A two-year retrospective analysis of HSGs was conducted in a community general hospital in Perth, Western Australia from March 2020 to March 2022. This period was selected accordingly with the emergence of intravasation awareness in regional obstetric and gynaecological imaging specialists. 315 HSGs were performed in this period; these were retrieved from the Picture Archiving and Communication Systems (PACS) and reviewed by researchers independently to determine intravasation rate, cannulation success and proportion of definitive results.
Definitive results were defined by peritoneal spillage in ≥ 1 fallopian tube or characteristic findings of tubal occlusion. Non-definitive results included studies with unsuccessful cannulation, obscured tubal spillage due to intravasation artefact, and poor visualisation of fallopian tubes with overall inconclusive tubal spillage.
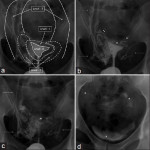
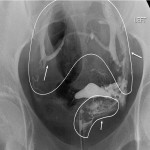
A blinded method was utilized to verify the presence and grade of intravasation in captured HSG still images. Grading was determined in accordance with the classification system proposed in 2013 in which the severity was attributable to anatomical landmarks; grade 1 being confined to the myometrium, grade 2 to the parametrium and grade 3 to the para-iliac region.
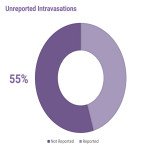
All interpretations were matched across researchers to ensure concordance prior to analysis.[3] Results were subsequently compared with reported intravasation to assess for discrepancies and under-reporting.