Type:
Educational Exhibit
Keywords:
Respiratory system, CT, Comparative studies, Cancer, Infection, Ischaemia / Infarction
Authors:
C.-J. Perrins, B. Cumming, K. Lau
DOI:
10.26044/ranzcr2022/R-0114
Imaging findings OR Procedure details
This pictorial review presents the clinical benefits of RSI created from CT Chest that could be used as baseline imaging in clinical scenarios that normally require follow-up Chest Radiographs or comparison with previous chest radiographs. Illustrative clinical applications include chest infection, lung collapse, benign and malignant pulmonary masses, interstitial lung disease, pleural effusion/collection, pulmonary infarction and medical device positioning.
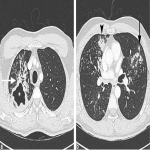
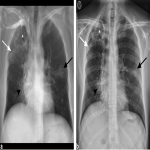
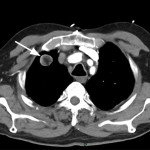
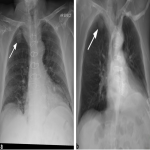
Pulmonary Tuberculosis
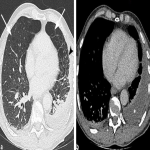
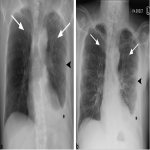
A 38 year old male recent migrant to Australia presented with haemoptysis on a background of 2 month history of non-productive cough and increasing fatigue. Sputum was positive for acid fast bacilli. CT chest demonstrated active post primary tuberculosis infection with cavitation. He was admitted for respiratory isolation and commenced anti-tuberculous therapy. CT chest was the initial investigation confirming appearances of post primary TB (Figure 1). Chest x-ray was performed after 1 week of therapy (Figure 2b) which showed moderate improvement of the right upper lobe airspace density as compared to the Ray Sum image created from the initial CT dataset (Figure 2a).
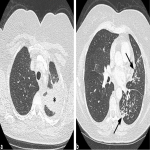
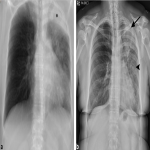
Lung Carcinoma
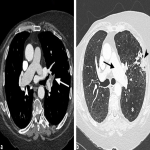
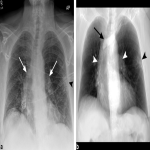
A 58 year old female with a remote smoking history presented to her local doctor with a dry cough. An external chest x-ray report stated a left upper zone opacity, which did not improve with antibiotics. She was referred for CT which showed an obstructing endobronchial mass in the left upper lobe resulting in segmental collapse of the left upper lobe, lymphangitis carcinomatosis in the lingula and left lower lobe, and hilar lymphadenopathy (Figure 3). Metastatic non‐small cell lung cancer was diagnosed with endobronchial biopsy. Palliative radiotherapy was commenced with follow-up chest x‐ray performed during the course of treatment which demonstrated increasing lymphangitis as compared to the ray sum image created from the initial CT (Figure 4).
Chronic pleural effusion
A 59 year old current smoker with severe emphysema and a history of rheumatoid arthritis was referred for CT to investigate worsening dyspnoea with clinical concern for pulmonary manifestations of his rheumatoid disease. CT demonstrated bullous emphysema, fibrosis, unilateral left pleural effusion and nodules (Figure 5). Follow up chest x-ray was performed to determine if the pleural effusion was part of rheumatoid disease or due to a superimposed infection (Figure 6). The left pleural effuions appear unchanged.
Pulmonary infarction
A 79 year old female presented to the Emergency Department with acute hypoxia and haemoptysis, three days unilateral leg swelling after a recent admission for emphysema when she had been immobilised for a prolonged period. She had a past history of breast cancer treated with mastectomy. Arterially phased thoracic CT was requested with clinical concern for haemorrhage due to metastasis or infection. Multiple occlusive pulmonary emboli were instead demonstrated with likely pulmonary infarction in the left upper lobe (Figure 7). The patient was admitted to ICU. Ray sum image was created which served as a baseline for the subsequent ICU portal chest radiograph (Figure 8).
Pulmonary Hamartoma
A 74 year old man was brought to the Emergency Department by ambulance after a fall at home. Trauma CT chest was performed for clinically suspected rib fractures. There was an incidental finding of pulmonary nodule which contained macroscopic fat density favouring a pulmonary hamartoma on the CT (Figure 9). This was a solitary nodule and there were no other worrisome findings. Based on the CT features, this was elected to be further investigated. 12 months later, the patient was referred by GP for follow-up chest x-ray to ensure stability of this nodule which was compared to the ray sum image created from the initial CT (Figure 10). The nodule was shown to be stable.