BACKGROUND:
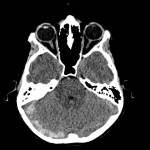
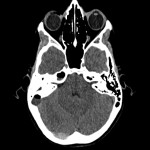
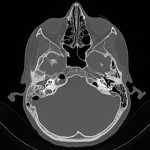
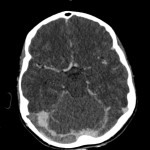
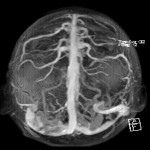
The intracerebral complications of acute mastoiditis are well documented and include cerebral venous sinus thrombosis (CVST), intracranial abscesses, cranial nerve palsies, meningitis and osteomyelitis.1 CVST is a well-documented complication of acute mastoiditis in the paediatric population, with a recently published retrospective cohort study reporting the incidence as high as 25%.1 The varying aetiologies of CVST are extensive and are classified as either genetic or acquired. Despite the broad differential in causative pathologies, there is a shared underlying pathological prothrombotic state. The basic pathophysiological principles of Virchow’s Triad describe the three factors predisposing to a prothrombotic state and include endothelial injury, static or turbulent blood flow and blood hypercoagulability.2 Once formed, venous thrombosis results in outflow obstruction, venous congestion, and an increase in hydrostatic pressure with subsequent interstitial shift in fluid with resulting cerebral oedema.3 CVST poses a diagnostic dilemma, as clinical presentation is often non-specific and related to subsequent raised intracranial pressure (ICP) and includes headache, nausea, vomiting, reduced GCS or seizure activity.4 Acquired CVST secondary to a central infection has further diagnostic difficulty, as symptoms are often masked by the primary pathology.
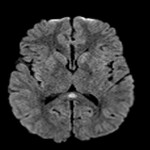
Cytotoxic Lesions of the Corpus Collosum (CLOCC) are secondary lesions of the corpus collosum that typically affect the splenium.5 They represent an active cytotoxic oedema. The proposed underlying pathophysiology is an inflammatory cascade mediated by cytokines interleukin-1 and interleukin-6, resulting in a significant increase in extracellular glutamate and subsequent intracellular shift into surrounding astrocytes and neurons, manifesting macroscopically as cytotoxic oedema.6,7 The splenium of the corpus collosum is typically affected given the density of oligodendrocytes expressing large number of Glutamate affected receptors.8
Given the underlying pathophysiology, there is a broad differential in aetiologies.Central infection, including encephalitis, meningitis and central abscesses are the most common cause of CLOCC lesions in children.5 Viruses are the most common pathogen and include rotavirus, Influenza virus (A, B) parainfluenza virus, mumps virus, adenovirus, human herpes virus (6, 7), cytomegalovirus, Human-parvovirus b19, enterovirus and Epstein-Barr virus.9 Recently, there have been documented cases of covid-19 associated CLOCC.5 Mycobacterial (mycoplasma pneumoniae) and bacterial causes are also well documented, and include Escherichia coli, enterococcus faecalis, salmonella and campylobacter jejuni.9 Excluding infection, trauma, epilepsy and metabolic conditions are the most common causes of CLOCC.5
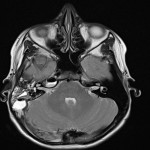
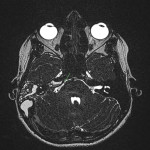
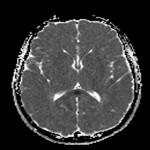
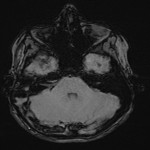
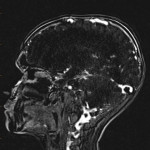
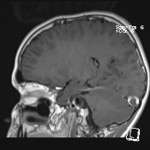
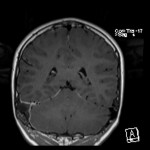
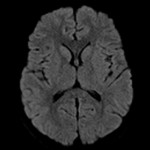
The neuroradiological features of CLOCC will be consistent with features of cytotoxic oedema; T2-weighted hyperintense signal, T2-weighted hyperintensity and Restriction diffusion on diffusion-weighted imaging, without contrast enhancement.7 These lesions will often be small oval lesions located restricted to the splenium; however, may extend into adjacent white matter.10 With appropriate treatment of the primary pathology and resolution of the inflammatory process, follow up imaging will typically depict complete radiological resolution with no resulting clinical neurological sequalae.10