Purpose
Development of brain metastases occurs in a significant minority of cancer patients[1]. Whole brain irradiation via simple parallel opposed photon beams was the historical treatment for multiple brain metastases and prophylactic cranial irradiation in small cell lung cancer. However, recent randomised evidence now make hippocampal-avoidance whole brain radiotherapy (HA-WBRT) a new standard of care for these indications[2-4]. Delivery of this treatment is much more complex and thus we have developed an efficient workflow to deliver treatment despite the complexity.
Methods and materials
Firstly, we assessed whether an atlas-based auto-contouring software, Elements V1.5 treatment planning software, would have sufficient conformality to radiation oncologists’ contours using the RTOG atlas[5].
We then created a department-specific auto planning model via the knowledge-based optimization engine, RapidPlan. This model was then validated against 10 manual plans generated by a senior radiation therapist per RTOG 0933 guidelines[3].
Implementation of successful workflow streamlining strategies was then adapted into an updated departmental clinical protocol.
Results
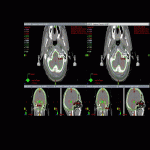
Although reasonable inter-clinician variability of the hippocampal contours was confirmed, there was less spatial overlap between the Elements-based auto-contours and clinician manual contours, with lower Dice co-efficient of 0.523 for the left hippocampus and 0.560 for the right. Variability between manual and auto-contours was also worse, with average maximum Hausdorff distance almost double that between clinicians at 9.213mm for the left and 9.855mm for the right hippocampus.
[Fig 1]
The auto-planning RapidPlan model was, however, successfully generated and validated against 10 manual standard template-based plans...
Conclusion
In an exploration of various workflow streamlining strategies for the complex standard-of-care treatment HA-WBRT, we have tested and validated a department-specific RapidPlan model and integrated this into our clinical protocol for real-world application and successful patient treatment. This has allowed for significant time reduction in treatment planning and delivery.
References
Brown PD, A.M., Khan OH, et al, Whole-brain radiotherapy for brain metastases: Evolution or revolution? J Clin Oncol, 2018. 24: p. 10.
Brown PD, G.V., Pugh S, et al., Hippocampal Avoidance During Whole-Brain Radiotherapy Plus Memantine for Patients With Brain Metastases: Phase III Trial NRG Oncology CC001. J Clin Oncol, 2020. 38(10): p. 11.
Gondi V, P.S., Tome WA, et al, Preservation of Memory With Conformal Avoidance of the Hippocampal Neural Stem-Cell Compartment During Whole-Brain Radiotherapy for Brain Metastases (RTOG 0933): A Phase II Multi-Institutional...