Radiation recall is an uncommon, unpredictable condition characterised by an acute inflammatory reaction in previously irradiated areas precipitated by a systemic agent [1, 2]. The time interval between prior radiotherapy and onset of radiation recall ranges from weeks to years [1, 2]. Chemotherapeutic agents are the most common trigger, with doxorubicin, gemcitabine, and docetaxel the most frequently documented [1, 2]. Other drugs have also been implicated including some antibiotics and simvastatin [1, 2]. The condition improves or resolves with withdrawal of the culprit, and in some cases the patient can be successfully rechallenged with the agent [1, 2].
The most frequent presentation of radiation recall is dermatitis of varying severity, from mild erythema to skin necrosis [1, 2]. Inflammatory reactions have also been documented in the lungs, oral mucosa, gastrointestinal system, genitourinary tract, muscle layer, central nervous system, neck, and head [1, 2, 3, 4, 5, 6, 7]. It should be noted that radiation recall is a separate entity from radiosensitisation which occurs immediately after radiotherapy and complications from radiotherapy itself.
Gemcitabine is atypical in that two thirds of Gemcitabine-induced radiation recall (GIRR) are non-cutaneous reactions [1, 3, 5]. The mechanism of action is poorly understood; higher gemcitabine dose and shorter time interval between radiotherapy and gemcitabine administration have been proposed as potential risk factors for the development and increasing severity of GIRR [3, 4].
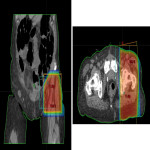
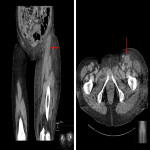
Myositis is a frequently encountered manifestation of GIRR which is often a diagnostic dilemma, partly due to the unusual induction of a focal muscle injury from a systemic agent [3, 4, 8, 9]. Previously reported cases have been associated with elevated creatine kinase and compartment syndrome, thus appropriate recognition of the condition is crucial [3, 4]. In our case of GIRR myositis, MRI demonstrated centrally non-enhancing muscle with a rim of enhancement in keeping with severe myositis with additional myonecrosis. Differentials with similar image findings included muscle metastasis (Figure 6), intramuscular abscess (Figure 7), and intramuscular haematoma (Figure 8).
GIRR myositis is a well-recognised condition in the oncology and radiation oncology specialties, however it has sparse documentation in the imaging community. In a recent literature review by Ravishankar et al (2018), only 2/21 cases of GIRR myositis were published in radiological journals [3]. Radiologic studies play a crucial role to support the diagnosis of GIRR myositis and to rule out other aetiologies. As we have demonstrated, access to radiation port data greatly benefits study interpretation. Clear communication with the referring specialist and radiation oncologist regarding history of radiotherapy and current gemcitabine therapy will also clarify the diagnosis.