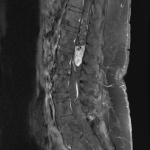
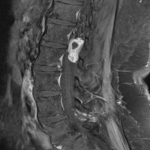
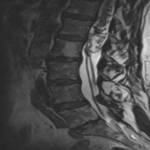
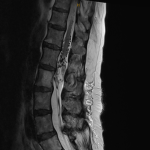
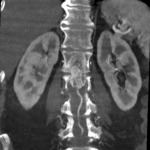
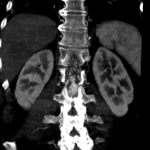
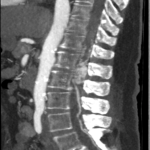
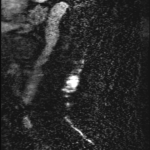
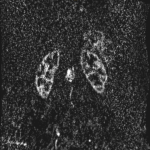
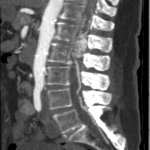
The MRI showed a 3.6cm heterogeneously enhancing intramedullary conus mass lesion with intratumoural T2WI-hyperintense cyst.
No cord signal change, syrinx/syringomyelia or hemosiderin deposition were seen.
CTA and MRA showed predominant feeders from lumbar arteries and a prominent draining vein.
There was no calcification on CT.
Intramedullary tumours
60% of spinal cord tumours (SCT) in adults are Ependymomas.1 Myxopapillary Ependymoma (ME) is a subtype of Ependymoma that exhibits a certain predilection for conus medullaris, filum-terminale and cauda-equina (90%).1
Hemangioblastoma are benign WHO-grade-1 lesions accounting for 6% of SCT.1 32% of Hemangioblastoma cases are associated with VHL disease and the remainder are sporadic.
There may be radiological clues to delineate Ependymomas and Hemangioblastomas, however, if the lesion involves the conus exclusively, they may be indistinguishable.1,3 Both tumours are1,3
- Usually isointense on T1WI and hyperintense on T2WI (to the cord)
- Associated with peritumoural cord edema, syrinx/syringomyelia and cyst formation
- Heterogeneously (unencapsulated Ependymoma, >/=2.5cm Hemangioblastoma) or homogenously enhancing
On contrary, an Astrocytoma usually shows heterogenous/infiltrating contrast enhancement pattern with cord expansion and is uncommon at conus location.1,5
Radiological features include1
- Calcification and vertebral remodelling in ME/Ependymoma
- Prominent tortuous vasculature, large draining vein and presence of arteriovenous shunting in Hemangioblastoma. An enhancing solid mass also helps distinguishing Hemangioblastomas from Arteriovenous-Malformation/Fistula.
In our patient the presence of both cranially arterialised vessels and caudal high-flow drainage indicated high-grade arteriovenous shunting.
Interestingly, there was lack of cord/conus edema which could be attributed to large perimedullary draining vein with a low-pressure gradient (direct drainage into iliac vein), favourable venous anatomy (anatomical variant of anterior median vein accompanying sacral nerve-root)
6 and conus arterial-basket compensating for cord perfusion deficits via collateralisation.
7 Long segment cord/conus edema is almost always seen in Dural-Arteriovenous-Fistula (DAVF).
1 Also, patient had no progressive lower limb weakness (a relevant clinical finding in DAVF).