Type:
Educational Exhibit
Keywords:
Abdomen, Colon, Gastrointestinal tract, CT, Ultrasound, Surgery, Hernia
Authors:
W. Awal, J. De Groot, T. Singh, P. Caleo
DOI:
10.26044/ranzcr2023/C-45
Imaging findings OR Procedure details
An 81-year-old female presented to a major tertiary emergency department in Queensland with fevers, lower abdominal pain and nausea. On examination, the patient was febrile and had right iliac fossa tenderness and a palpable right inguinal lump. She had no clinical features of peritonitis. Relevant background included a distant history of bilateral inguinal hernia repairs.
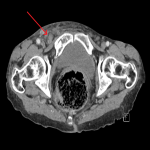
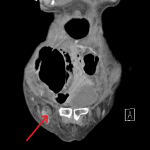
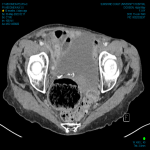
A CT of the abdomen and pelvis with portal venous phase IV contrast was performed. Typically, the appendix can be seen to have entered the inguinal sac on CT, confirming the Amyand hernia.[1] However, in this case, the appendix could not be confidently visualised and instead only a small fat-containing right indirect inguinal hernia was detected (indicated by the red arrows in Figure 1 and 2). There was fat stranding and oedema of the cecal wall (Figure 3). The rest of the abdominal organs were unremarkable and no prior images were available for comparison. It was recognised that the inflammatory changes in the right iliac fossa could be obscuring an appendix within the inguinal canal. As a result, the reporting radiologist recommended further imaging in the form of an ultrasound or CT with oral contrast.
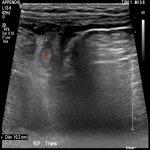
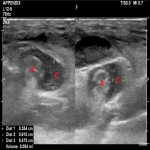
An ultrasound was performed later that day. It revealed that the appendix was indeed located in the right inguinal canal alongside a small fat-containing hernia. The appendix (label A in Figure 4) was enlarged and non-compressible with probe tenderness and increased periappendiceal echogenicity, consistent with appendicitis. A 6x5x4mm anechoic collection was also seen adjacent to the appendix (label C in Figure 5).
Losanoff and Basson proposed a classification system to guide the management of Amyand hernias:[4]
- Type 1: Normal appendix in an inguinal hernia; managed with hernia reduction and mesh repair.
- Type 2: Acute appendicitis in an inguinal hernia with no abdominal sepsis; managed with appendicectomy and primary repair of hernia without mesh.
- Type 3: Acute appendicitis in an inguinal hernia with abdominal or abdominal wall sepsis; managed with laparotomy, appendicectomy and primary repair of hernia without mesh.
- Type 4: Acute appendicitis in an inguinal hernia with concomitant abdominal pathology; managed as type 3 plus management of the concomitant disease.
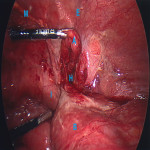
The present case involved a Type 2 Amyand hernia. An emergent laparoscopic appendicectomy was performed (Figure 6) and histopathology revealed perforated appendicitis with a sessile serrated neoplasm. The surgeon did not repair the inguinal hernia as the defect was small.