Learning objectives
The goal of this exhibit is to prepare practicing radiologists and trainees to recognize benign circumstances where air can be found in atypical locations. Additionally, we will provide tips to distinguish these benign conditions from true pathology, when possible.
Background
The presence of air in numerous locations (pleural space, peritoneum, parenchyma of various organs) is a cause for concern in the emergency setting. However, numerous benign conditions can result in air in unusual locations. It is important for the practicing radiologist to be aware of these pitfalls to avoid unnecessary alarm and to prevent additional unneeded imaging or procedures. The purpose of this presentation is to demonstrate numerous cases where air can present in unusual locations, which are associated with benign etiologies. Through this educational...
Imaging findings OR Procedure details
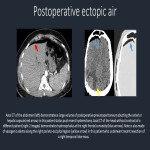
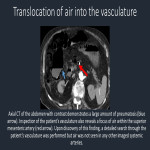
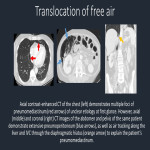
In the emergency radiology setting, ectopic air can frequently be a cause for alarm, such as with pneumothorax, pneumomediastinum, and portal venous gas. However, there are many benign conditions which may present radiographically with air in unusual locations. As a practicing radiologist, it is critical to be able to recognize these benign entities as such to avoid additional, unnecessary procedures or imaging.
Here, we will present numerous benign conditions which can produce air in unusual locations that we have encountered in our practice. Some conditions...
Conclusion
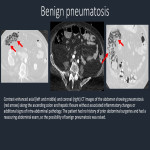
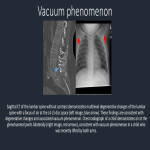
Ectopic air can frequently be a harbinger of pathology. Conditions such as portal venous gas, pneumatosis, and pneumoperitoneum appropriately raise alarm for associated pathology. However, ectopic air is not always indicative of an underlying problem and can be associated with numerous benign entities. Here we present benign causes of ectopic air to demonstrate important radiologic concepts, such as the vacuum phenomenon and the continuity of fascial planes. We stress the importance of relating the patient’s history and clinical status to imaging findings to increase confidence...
References
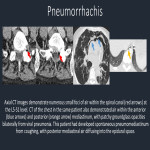
Valiyakath, D., Al Busaidi, T., Al Shamsi, S., & Al Sawafi, Y. (2018). Pneumorrhachis with Spontaneous Pneumomediastinum: Should It Raise Special Concerns? Oman Medical Journal, 33(3), 256–259.
Sandstrom, C. K., Osman, S. F., & Linnau, K. F. (2017). Scary gas: intravascular, intracranial, and intraspinal ectopic gas (part III). Emergency Radiology, 24(4), 411–416.
Leturia Etxeberria, M., Biurrun Mancisidor, M. C., Ugarte Nuño, A., Arenaza Choperena, G., Mendoza Alonso, M., Esnaola Albizu, M., Serdio Mier, A., Gredilla Sáenz, M., & Gomez Usabiaga, V. (2020). Imaging Assessment of...