Testicular tumours are a heterogeneous group of histopathological entities with different biological behaviours and variable prognosis.1 Although several histological subtypes, such as seminoma, predominate in the appropriate patient population, there are other less common categories, including sex cord stromal tumours and lymphoma. There is an impetus to establish histological diagnosis short of surgical orchidectomy, in certain clinical contexts, including the presence of a single testis, prior orchidectomy, high anaesthetic or surgical risk, and patient preference.2,3,4,5,6,7 Ultrasound guided percutaneous testicular core biopsy has served to be valuable for this purpose in our experience.
Ultrasound guided percutaneous testicular core biopsy has been performed for at least 25 years.4 The advantages are its minimally invasive nature and suitability to be performed as an outpatient procedure with local anaesthesia. A hurdle to the wider adoption of percutaneous testicular biopsy is the theoretical risk of needle tract seeding due to scrotal violation altering the pattern of metastatic lymphatic spread in anatomically separate drainage basins of the testis (retroperitoneal lymph nodes) and scrotum (inguinal lymph nodes).11 Scrotal violation is historically associated with scrotal orchidectomy, which is considered a non-standard surgical approach in contrast to inguinal orchidectomy.3,8,9,10 Although there is evidence of slightly increased risk of local recurrence with scrotal orchidectomy compared to inguinal orchidectomy (2.9% versus 0.4%, respectively), this was observed in advanced tumours. 9,12,13 No statistical differences in distant disease recurrence or overall survival are demonstrated between either surgical approaches.9,12,13 Many authors consider the risk to be overstated, particularly in the case of percutaneous testicular biopsy. 2,3,4,5 There are no well documented cases of tumour seeding due to percutaneous testicular biopsy in the literature. 2,3,4,5
A total of five individual patients underwent ultrasound guided testicular core biopsy in a 16-month period from 2021 to 2022 at an Australian tertiary teaching hospital. All biopsies were performed by a single Consultant Radiologist, after the cases have been subjected to multidisciplinary discussion. Consensus for undertaking biopsy was attained between Radiologist, Urologist, Oncologist and Pathologist for all cases, with review of case history, imaging findings and histopathology results.
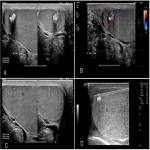
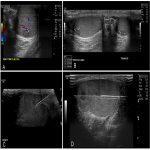
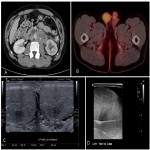
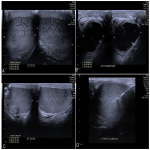
The testicular lesions were optimally visualised with a selection of high frequency linear array ultrasound transducers (GE ML6-15-D Matrix Linear Probe, GE 9L Linear Probe and Phillips L15-7io Transducer). A caudal to cranial approach was utilised to reduce the risk of vasovagal reaction. Minimal ultrasound transducer gel was applied to the scrotum to allow easier manual fixation of the testis by an assistant. Local anaesthesia was achieved with Lignocaine 1% by infiltration of the overlying skin and tunica vaginalis, which are sensitive to pain. No pain fibres are present in the testicular parenchyma, obviating the need for deeper infiltration. This was augmented with patient self-administered Methoxyflurane (Penthrox®) inhaler for further analgesic effect. An 18 gauge core biopsy needle (Temno Evolution) was used. Patients were monitored for 1 hour after biopsy.