Case 1 – Large cell calcifying Sertoli tumour
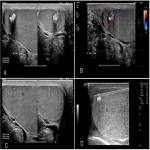
26-year-old male presented to his general practitioner with 6-month history of right scrotal swelling and intermittent pain. Physical examination was unremarkable. Scrotal ultrasound detected two hyperechoic lesions at the superior pole of the right testis, measuring 9 mm and 5 mm respectively (Figure 1 A-C). There is posterior acoustic shadowing associated with the larger lesion, in keeping with intralesional calcification. Both lesions demonstrate vascularity on doppler assessment. Serological tumour markers were within normal limits. The lesion was deemed indeterminate following multidisciplinary review, although stable size and morphology on repeated ultrasounds over 18 months were reassuring features. An ultrasound guided core biopsy of the larger right testicular lesion was performed (Figure 1 D). Histopathology confirmed the presence of a sex cord stromal tumour with features of large cell calcifying Sertoli cell tumour. Staging CT scan was negative for nodal or metastatic disease. The patient opted for active surveillance rather than right orchidectomy given a low malignant potential.14 The lesion remained stable in size and morphology on subsequent follow up 12 months post-biopsy.
Case 2 – Incidental imaging finding – Leydig cell tumour
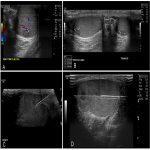
34-year-old presented to General Practitioner with left scrotal discomfort. Ultrasound demonstrated normal appearance of the left testis. However, an incidental hypoechoic and avascular small 4 x 3 x 3 mm lesion was detected in the right testicular upper pole. The lesion was followed up over serial ultrasounds, where gradual growth of the lesion over a period of two years occurred, to a maximal size of 7 x 5 x 4 mm. Tumour markers remained within normal limits. An initial right testicular core biopsy yielded non-diagnostic core samples, noting that the peripheral location and small size were contributing factors to a challenging biopsy. A second right testicular biopsy was performed after optimising biopsy tract and manual external stabilisation of the right testis by a procedural assistant. The specimen demonstrated Leydig cell tumour based on histologic and immunohistochemical features. Staging CT scan was negative. The tumour was deemed to be of low risk of locoregional or metastatic spread following multidisciplinary review, given the cytological and histologic features (absence of cytologic atypia, frequent mitoses and necrosis), current size and slow historical growth.15 The patient opted for a surveillance strategy.
Case 3 –Discrepancy in imaging findings – Seminoma
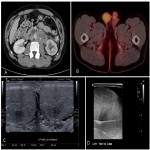
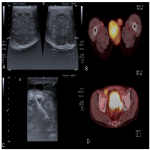
32-year-old male presented with 1-week history of left flank pain, nausea and loss of appetite. Scrotal examination was unremarkable. CT was arranged for possible renal colic, which detected a large lobulated left paraaortic retroperitoneal soft tissue mass with associated left ureteric obstruction. A differential diagnosis of lymphoma, germ cell tumour and retroperitoneal fibrosis was considered. FDG PET/CT confirmed high tracer uptake in the retroperitoneal mass and the right testis. There was no abnormal uptake associated with the left testis.
However, scrotal ultrasound detected a 6 mm poorly defined hypoechoic lesion in the inferior pole of the left testis with associated vascularity. There was reversed diastolic flow in the right testis but no focal intratesticular lesion was evident to correlate with the FDG PET/CT finding.
The patient underwent CT guided core biopsy of the retroperitoneal mass. Histopathology confirmed metastatic germ cell tumour with features of seminoma. Due to the discrepant findings between the FDG PET/CT and ultrasound, ultrasound guided core biopsy of both testes was performed. Core biopsies of the left testicular lesion and the right testis were separately performed. Histopathology of the left testicular tissue confirmed germ cell neoplasia in situ. Histopathology of the right testicular tissue was negative for malignancy. The patient underwent neoadjuvant BEP chemotherapy, followed by left radical orchidectomy. The right testis was preserved. Subsequent surveillance imaging studies were negative for disease recurrence.
Case 4 – Fibrosis secondary to foreign material
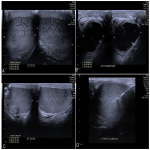
A 37-year-old presented with bilateral testicular enlargement and night sweats with a distant history of hydrocele surgery. Physical examination confirmed grossly enlarged and extremely firm testes. Tumour markers were within normal limits. Ultrasound revealed bilateral enlarged testes, with the left approximating 52 cc and the right 28 cc in respective volumes. A curvilinear anechoic pattern was observed throughout bilateral testicular parenchyma. A 39 mm left epidydimal cystic lesion with thin septations was evident. FDG PET/CT study was performed, which did not reveal abnormal tracer uptake. Ultrasound guided core biopsy of the left testis was performed. Histopathology demonstrated dense fibrotic reaction to foreign material, likely sutures.
Case 5 – Seminoma and leukaemia/lymphoma
60-year-old presented with three-week history of right scrotal swelling on background of chronic lymphocytic leukaemia and right inguinal hernia surgery 16 months ago. Examination confirmed the presence of a firm right testis extending along the spermatic cord. Tumour markers were within normal limits. Ultrasound revealed an 87 x 72 x 94 mm lobulated and heterogeneous right testicular mass, and normal appearance of the left testis. There was additional right inguinal lymphadenopathy. Intense FDG uptake was demonstrated in the right testicular lesion and moderate FDG uptake was present in the right inguinal canal. Ultrasound guided core biopsy of right testis was performed. Histopathology revealed seminoma infiltrating the rete testis. Ultrasound guided core biopsy of the right inguinal lymph node confirmed concurrent chronic lymphocytic leukaemia and small lymphocytic lymphoma.