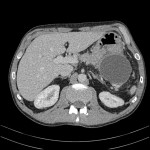
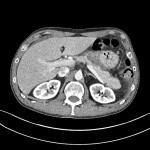
Two weeks prior to this patient's presentation to the emergency department, a routine CT abdomen and pelvis with contrast was performed, as follow up for a known pancreatic pseudocyst. The pseudocyst had developed as a consequence of acute interstitial pancreatitis, secondary to alcohol. This CT scan demonstrated a rim-enhancing lesion, arising from the tail of the pancreas. Note that this lesion is compressing the greater curvature of the stomach. The pancreas at this time enhances homogeneously. There does not appear to be any region of focal necrosis. Overall, findings are consistent with a pancreatic pseudocyst, without evidence of acute pancreatitis.
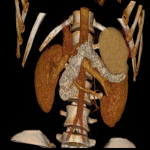
A 3D reconstruction of this CT scan provides a useful reference point for the size and morphology of this pseudocyst, at this point in time
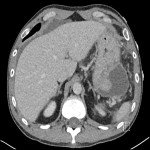
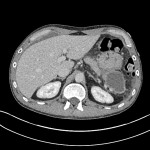
The patient presented to the emergency department, two weeks following this scan due to sudden onset abdominal pain. Serum lipase at this time was 118units/L (reference range <60). Contrast enhanced CT abdomen and pelvis at this time demonstrated partial decompression of the known pancreatic tail pseudocyst, with mild to moderate volume of abdominal free fluid. These imaging findings, in conjunction with a history of acute abdominal pain raised concerns for a pancreatic pseudocyst rupture.
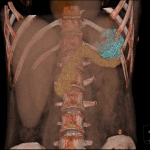
3D reconstruction of the pseudocyst, created based on the CT abdomen and pelvis at presentation demonstrates an interval reduction on the size of the pseudocyst, again raising concerns for a rupture.
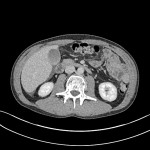
A CT pancreas multiphase was conducted to better evaluate the pancreas. This scan demonstrated oedema equivocal for early pancreatitis.
This scan again demonstrated an increase in free fluid within the abdomen, compared to the scan two weeks prior to admission, supporting the theory of pseudocyst rupture. Free fluid can be seen below the right hemidiaphragm and anterior to the liver.
Additionally, free fluid can be seen within Morrison's pouch (Hepato-renal recess).
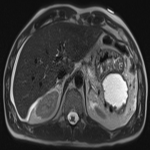
Magnetic Resonance Cholangiopancreatography (MRCP) clearly demonstrates this fluid fill pseudocyst. Additionally, non-specific free fluid within the abdomen is again demonstrated anterior to the liver and within Morrison’s pouch. This fluid may have been due to leakage from the pseudocyst, as previously suggested. However, absence of fluid directly around the pseudocyst favoured against a pseudocyst rupture.
In short, the consensus was that this individual's presentation may have been secondary to a rupture of the pseudocyst, as suggested by the initial CT abdomen and pelvis with contrast, at presentation to the ED. However, this could not be claimed with complete certainty, considering further imaging (MRCP), did not necessarily support this. Ultimately, given the patient had remained hemodynamically stable, and their symptoms had started to resolve, it was decided that surgical intervention was not necessary at this stage in time. Close follow up, including repeat imaging, was arranged.