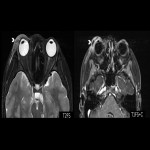
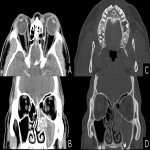
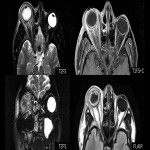
Anatomical considerations
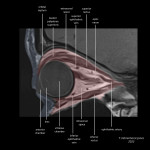
Conceptualizing the orbit as a house, the walls of the orbit form a pyramidal-shaped space enclosed by the frontal, sphenoid, ethmoid, zygomatic, lacrimal, maxillary, and lacrimal bones [2]. Intimately related, the paranasal sinuses may act as a source of infection. While other paranasal sinuses may act as a nidus, the ethmoid sinus is most commonly accountable. Neurovascular perforations or dehiscence of the thin lamina papaya of the ethmoid bone account for this propensity [3,4].
Anteriorly the orbit is confined by the orbital septum. This fibrous membrane is draped from the periosteum of the orbital rim to the levator palpebrae aponeurosis in the superior eyelid and the inferior border of the tarsal plate in the lower eyelid [1]. Acting as the “front door” of the orbit, the orbital septum acts to divide the preseptal (periorbital) and postseptal (orbital) spaces. In separating these spaces, the orbital septum acts as a barrier to prevent the transmission of infections of the face into the orbit proper. This barrier however is incomplete, as much like the lamina papyacea, it is perforated by neurovascular bundles [4].
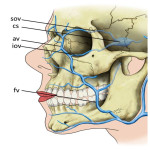
Spread of infection deep to the orbital septum may occur in an indirect manner via the valveless veins of the face [4]. Hematogenous spread occurs due to bidirectional flow in the ophthalmic veins that cross the orbital septum into the postseptal space before draining into the cavernous sinus.
The Chandler Classification
Originally a clinical classification, Chandler et al classified orbital infections into five types relative to the orbital septum and extent of disease [5]. While not necessarily demonstrating a natural progression of disease [4,6], the Chandler classification is useful in conceptualizing infections of orbit anatomically and clinically. The types are as follows:
Type I - periorbital (preseptal) cellulitis
Most commonly due to an infection of the skin (often secondary to insect bite or trauma), inflammation is confined anterior to the orbital septum. Sinusitis is also an attributable cause (especially in children) but is more associated commonly with a postseptal process [1,4].
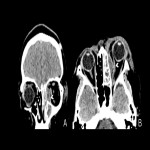
Periorbital cellulitis is visualized on CT as soft tissue swelling and subcutaneous oedema anterior to the orbital septum, separate from the orbit proper [2].
A small crescent-shaped rim-enhancing low-attenuation collection along the anterior globe may be demonstrated. This represents chemosis (conjunctive swelling) that should not be confused with an eyelid abscess [1].
Type II - orbital (periorbital) cellulitis
In developed countries, orbital cellulitis is most commonly secondary to maxillary or ethmoid sinusitis [7]. This process is facilitated in a hematogenous manner and via natural dehiscence (especially in the lamina papyracea) [9]. Therefore, bony destruction while occasionally demonstrated, is uncommonly seen [9]. In developing countries, the most common cause is due to direct inoculation due to trauma, in-situ foreign bodies, or surgery [7].
On CT imaging orbital cellulitis appears as inflammatory stranding posterior to the orbital septum in a diffuse or localized appearance with or without associated periorbital cellulitis [2]. There should be no rim-enhancing lesion to indicate an abscess [4].
If unclear on CT, T2 fat-saturated imaging may be utilized for clarity as well as diffusion-weighted imaging to demonstrate restricted diffusion to delineate the presence of abscess [3].
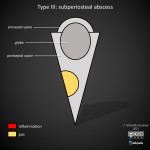
Type III - subperiosteal abscess
A subperiosteal abscess forms as the subperiosteal space fills with oedema and pus. The intact orbital periosteum contains the infectious material. Diagnosis is significant as mass effect may lead to tension on the optic nerve due to displacement of the globe (proptosis) potentially leading to ischemia and blindness [4].
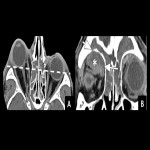
Subperiosteal abscesses appear as a lenticular rim-enhancing fluid collection tracing along the orbital wall [2]. Soft tissue density adjacent to a fluid-filled paranasal sinus should be considered suspicious for subperiosteal abscess [3]. The shape will be typically obtuse in shape as the collection is positioned beneath the periosteum [3]. The most frequent location is along the medial orbital wall in association with ethmoid sinusitis [4,8].
Diffusion-weighted MRI demonstrates restricted diffusion [1].
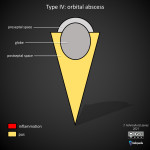
Type IV - orbital abscess
Orbital abscess refers to purulent material within the orbit itself. Pus may be intraconal or extraconal. Extraconal abscess is typically due to orbital cellulitis or subperiosteal abscess rupture while intraconal abscess is more regularly due to trauma or surgical complications. CT imaging may demonstrate a peripherally enhancing fluid collection [2].
In contrast to a subperiosteal abscess, orbital abscess walls tend to be more irregular in shape than a subperiosteal abscess [3]. Diagnosis however can be difficult when the abscess is not clearly separate from the orbital wall.
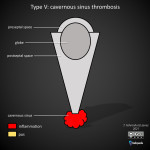
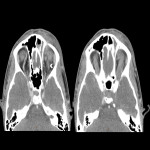
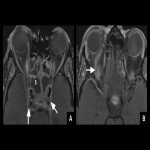
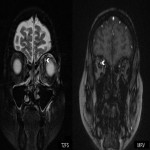
Type V - cavernous sinus thrombosis
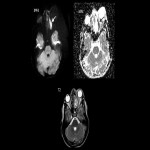
A worrisome complication of orbital infection, cavernous sinus thrombosis carries a significant risk of vision loss and death. Contrast-enhanced MRI is superior to CT (including CT venography) in the early stages of disease with the diagnosis being potentially difficult [2,4]. Changes to look for include a bulky cavernous sinus with convex margins, non-fat filling defects, and associated changes within the orbits. Septic thrombophlebitis of the superior ophthalmic veins often accompanies and can be a clue as to the involvement of the cavernous sinus on both contrast-enhanced CT and MRI [1,3].
Who needs imaging?
While Chandler I (periorbital cellulitis) typically takes a benign course with treatment, Chandler II (orbital cellulitis) and above represent a serious risk of blindness and mortality. Delineating patients as preseptal versus beyond is important as patients with Chandler III (subperiosteal abscess) and greater often require surgical intervention.
On clinical exam, preseptal disease is characterized by soft tissue swelling without ophthalmoplegia. Although in severe cases there may be a mild limitation of eye movement with or without chemosis [1], ophthalmoplegia strongly suggests the spread of infection beyond the orbital septum. Further, central neurological signs are not classic of orbital cellulitis alone and one must consider intracranial extension [7].
Clinical features that require radiological investigation include [7,12]:
- ophthalmoplegia
- decreased visual acuity or colour vision
- central neurological signs
- cranial nerve palsies
- proptosis
- bilateral oedema
- limited clinical exam due to soft tissue swelling
Imaging is not necessary in the absence of the above features as many patients with periorbital cellulitis alone will respond positively to antibiotics within a short timeframe [12]. If there is no improvement or deterioration in the condition of patients following 24 hours of treatment imaging should be performed [7].
A recommendation from Mathew et al [10] following a review of 10 years of paediatric presentations recommends that all patients with a suspected diagnosis of orbital cellulitis receive a post-contrast CT head/orbit. This should be combined with a careful review of the superior ophthalmic veins and cavernous sinus [10]. Further to this, if superior ophthalmic vein thrombosis is detected the patient should proceed to MRI to interrogate the cavernous sinus. Similarly, a study by Kapur et al [10] suggested that MRI should be considered in cases in which there is clinical or CT suspicion for complications intracranially (cerebritis, abscess, empyema).
In the setting of rapidly deteriorating vision (orbital compartment syndrome), surgical decompression of the orbit (lateral canthotomy) should not be delayed by imaging as only 60-100 minutes of elevated pressure may lead to irreversible vision loss [2,12].