Learning objectives
To review the principal neuropediatric acute syndromes.
To define the best imaging techniques in this setting.
To describe the most important radiological findings.
Background
Even though acute neurological deficits are far more common in adults,
they are also relatively common in the pediatric population.
Neuroimaging is fundamental to get an accurate diagnosis to treat the patient correctly.
Computed Tomography (CT) is the most widely used technique in the emergency setting,
being particularly useful for the recognition of blood.
Magnetic Resonance (MR) is more informative in most of the cases but is not always available and may require sedation.
Ultrasound (US) has a role in the newborn,
since it can...
Findings and procedure details
STROKE
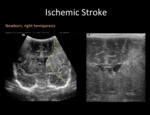
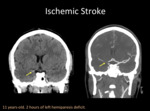
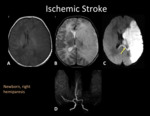
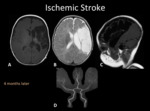
Ischemic Stroke
Pediatric stroke is a relatively uncommon cause of acute neurological deficit.
The reported incidence is 13 cases per 100.000 children when newborns are excluded.
In newborns the reported incidence is 25 to 40 cases per 100.000 children.
Ischemic strokes account for approximately 50% of the cases (versus more than 80% in adults) [1].
They lead to significant morbidity and mortality,
as an example,
over 50% of the survivors of an ischemic stroke will have persistent neurological deficits [2].
The most important risk...
Conclusion
Acute-onset neurological deficits are unusual in children.
Imaging is pivotal for the correct etiological diagnosis,
leading to a timely treatment,
aimed to avoid sequelae.
Causes include: stroke,
inflammatory-infectious diseases,
spinal cord and toxic pathology,
among others.
MRI is the technique of choice in most cases; but ultrasound plays a role in newborns.
CT scan is used to rule out a neurosurgical emergency and when a stroke is suspected.
In this poster we characterized different acute clinical scenarios using multimodality imaging.
Personal information
Contact details:
Dr.
Pablo Alvayay Quilodrán
Neuroradiology Section.
Department of Radiology,
Clínica Alemana de Santiago.
Chile.
Facultad de Medicina Clínica Alemana-Universidad del Desarrollo,
Santiago,
Chile.
Email:
[email protected]
Dr.
Valeria Schonstedt Geldres
Neuroradiology Section.
Department of Radiology,
Clínica Alemana de Santiago.
Chile.
Email:
[email protected]
Dr.
Ximena Stecher Guzmán
Neuroradiology Section.
Department of Radiology,
Clínica Alemana de Santiago.
Chile.
Facultad de Medicina Clínica Alemana-Universidad del Desarrollo,
Santiago,
Chile.
Email:
[email protected]
References
Rich PM,Cox TC,Hayward RD.The jugular foramen in complex and syndromic craniosynostosis and its relationship to raised intracranial pressure.
AJNR Am J Neuroradiol 2003;24: 45–51.
Khanna PC,
Thapa MM,
Iyer RS,
et al.
Pictorial essay: The many faces of craniosynostosis.
Indian J Radiol Imaging 2011;21: 49–56.
Rahman S,
Noujaim SE,
Chaiyasate K.
Craniosynostosis: Diagnosis,
Pitfalls,
and Management.
What the Radiologist Needs to Know.
Neurographics 2017; 7(5): 354 –362.
Benson ML,
Oliverio PJ,
Yue NC,
et al.
Primary craniosynostosis: imaging features.
AJR Am J Roentgenol 1996; 166:...