Aims and objectives
Computed tomography (CT) imaging is widely used for diagnosis,
staging,
treatment response assessment,
and surveillance in oncology.
In the past few years,
with the advent of more effective cancer treatments,
long-term survival of patients with malignant diseases has increased [1].
As a consequence,
patients receive multiple ct examinations during the course of their disease and increasing radiation exposure has become a matter of concern.
In fact,
there is reasonable epidemiological evidence that effective doses below 100 mSv result in non-negligible increase in cancer risk [2,...
Methods and materials
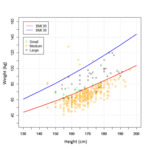
A BMI-based table (see Figure 1) was proposed to adjust CT CAP acquisition protocol according to patient BMI.
For patients “Small” (BMI < 26 kg/m2),
“Medium” (26 < BMI < 36) and “Large” (BMI > 36 kg/m2),
100 kVp,
120 kVp and 140 kVp should be used,
respectively.
Protocols have been implemented on a GE Discovery 750HD: other minor differences regard bow tie filter and tube rotation time,
complete recap of acquisition parameters can be found in Table 1.
Protocol Small
Protocol Medium
Protocol Large...
Results
Compliance to suggested table
In phase I,
949 patients were examined: 650 were “Small”, 277 “Medium” and only 22 “Large”.
248 examinations were performed with the “Small Protocol” (100 kVp),
641 with the “Medium Protocol” and 60 with the “Large Protocol”.
As shown in table 2,
481 out of 949 acquisitions (50.7%) were not optimized,
i.e.
proper protocols were not chosen according to patient BMI,
as proposed in the suggested chart (Figure 1).
In particular,
412 Small patients out of 650 (63.4%) were imaged with...
Conclusion
In this study we showed a possible framework to optimize chest-abdomen-pelvis examination for oncological patients.
A BMI-based table was suggested to choose a proper protocol according to patient body size.
Results of the first period were not promising,
since more than 50% of all patients and more than 60% of patients with BMI lower than 26,
were not scanned with the optimized protocol.
Written reminder and continuous monitoring allowed use to reduce the percentage of non-optimized examinations to 28% and 35% respectively.
Differences in image...
Personal information
P.
De Marco,
Medical Physicist
IEO,
European Institute of Oncology,
IRCCS,
Milan
Unit of Medical Physics
Department of Radiology
e-mail:
[email protected]
References
1.
Siegel RL,
Miller KD,
Jemal A.
Cancer statistics,
2015. CA Cancer J
Clin 2015;65:5-29.
2.
Preston DL,
Ron E,
Tokuoka S,
et al.
Solid cancer incidence in atomic bomb survivors: 1958-1998. Radiat Res 2007;168(1):1-64
3.
National Research Council.
Health risks from exposure to low levels of
ionizing radiation: BEIR VII—phase 2.National Academies Press,
2006.
4.
Mc Collough CH,
Primak AN,
Braun N,
et al.
Strategies for reducing radiation dose in CT.
Radiol Clin North Am 2009; 47(1):27-40
5.
Nelson RC,
Feuerlein S,
Boll DT....