Learning objectives
To provide a systematic approach and scheme to narrow the differential diagnosis of primary retroperitoneal masses,
based upon the predominant cross-sectional imaging appearance.
Background
INTRODUCTION
Primary retroperitoneal neoplasms are a diverse group of benign and malignant tumors that arise within the retroperitoneum but outside the major organs.
Of the primary retroperitoneal neoplasms,
70%–80% are malignant in nature,
and these account for 0.1%–0.2% of all malignancies in the body.
One-third of malignant retroperitoneal neoplasms are sarcomas; 15% of all sarcomas originate within the retroperitoneum.
Although computed tomography and magnetic resonance imaging can demonstrate important characteristics of these tumors,
diagnosis is often challenging for radiologists.
Diagnostic challenges include precise localization of...
Findings and procedure details
Approach to retroperitoneal masses
The majority of retroperitoneal masses arises from retroperitoneal organs and is therefore not considered primary retroperitoneal mass.
Diagnosis of a primary retroperitoneal mass may be made once the location is confirmed as within the retroperitoneal space and after an organ of origin is excluded.
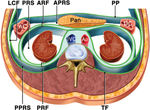
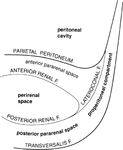
1.Tumor location (Determining tumor location into the retroperitoneal spaces)
Displacement of normal retroperitoneal structures,
such as retroperitoneal organs or vascular structures,
suggests that a mass is retroperitoneal in location(Fig.
5).
Nevertheless,
determining retroperitoneal tumor location could be...
Conclusion
The differential diagnosis of primary retroperitoneal masses may be based on the predominant cross-sectional imaging appearance as either cystic or solid and neoplastic and non-neoplastic.
Characteristic imaging findings,
such as the composition (Fat,
calcification and necrosis),
enhancement pattern,
vascularity,
location,
and relationship to adjacent structures,
may be combined with clinical information and assisted by diagnostic scheme to help narrow the differential diagnosis.
Personal information
Dr.Ahmed Hassan Ali Mohamed
Demonstrator of radiology,
National cancer institute,
Cairo university,
Egypt.
E-mail:
[email protected]
[email protected]
Asst Prof.Hisham S.Wahba Mikhael
Assistant professor of radiology,National cancer institute,
Cairo university, Egypt.
Fellow of McGill University,
Canada
Prof.Sameh Abdel Aziz Hanna
Professor of radiology,
Faculty of medicine,
Cairo university,
Egypt.
References
References:
Bhargavi D.,
Avantsa R.
andKala P.
"MDCT signs differentiating retroperitoneal and intraperitoneal lesions- diagnostic pearls" ECR 2015.
Austria Center Vienna,
Vienna,
Austria,
ECR 4 Mar.
2015.
Poster presentation.
Burkill,
G.
J.
C.,
and J.
C.
Healy.
"Anatomy of the retroperitoneum."Imaging12.1,
10-20,
2000.
Carbognin,
Giovanni,
Lucia Pinali,
and Carlo Procacci.
"Retroperitoneal tumors." Radiologic-Pathologic Correlations from Head to Toe.
Springer Berlin Heidelberg; 619-643,
2005.
Cardone,
Messina,
Vergnaghi,
et al.
"Retroperitoneal tumors: Computed Tomography (CT) and Magnetic Resonance (MR) patterns" ECR 2011.
Austria Center Vienna,
Vienna,
Austria,...