Keywords:
Cardiac, CT-Angiography, Computer Applications-3D, Hyperplasia / Hypertrophy
Authors:
D. K. Kang, J. S. Sun, J. Y. Cho, Y. K. Sur, J. S. Park; Suwon/KR
Methods and Materials
We retrospectively enrolled 490 consecutive individuals (383 males; mean age,
35.2 ± 4.4 years) who underwent cardiac CT.
CV risk factors for the entire study population were obtained through review of medical records at the time of cardiac CT examinations.
10-year CHD risk based on the Framingham risk score (FRS) was calculated for each patient.
Image acquisition was performed using a dual source 128-slice CT (Somatom Definition FLASH; Siemens Healthcare,
Forchheim,
Germany).
- First,
all patients underwent non-enhanced imaging to calculate the coronary artery calcium (CAC) score before contrast enhanced cardiac CT.
- Contrast enhanced cardiac CT was acquired using the retrospective ECG-gating spiral scan protocol.
The prospective tube current modulation technique was used with a high-dose window of 65-80% of the R-R interval (if heart rate > 75,
then the window was between 35% and 50% of the R-R interval) and with the Mindose® protocol (Siemens) in the remaining phases of the cardiac cycle.
Cardiac CT image analysis was performed using picture archiving and a communication system (PACS).
If a reader visually identified the diseased segment,
further evaluation of the coronary artery was performed using Syngo.via (Siemens Healthcare).
- The 15-segment model based on the American Heart Association classification with the addition of the ramus intermedius as segment 16 was used.
- The total plaque severity score (or extent of coronary plaque burden; range,
0-16) per person was determined by summing the number of diseased coronary segments.
- For each coronary atherosclerotic plaque,
the composition (calcified,
mixed,
or non-calcified),
and stenosis were visually classified.
- Any coronary segment in which ≥ 50% or greater of the diameter appeared stenosed was classified as having significant stenosis.
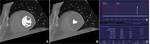
LV function was evaluated using a semi-automated LV endocardial and epicardial contour detection technique and threshold-based blood volume mode (Syngo.via,
Siemens Healthcare) (Fig.
1).
- With this method,
papillary muscle was excluded for LV chamber volume and included for LV mass.
- LVMi was derived by adjustment for the patient’s body surface area (BSA).
Transthoracic echocardiography was performed using a Philips iE33 (Philips Medical Systems,
Andover,
MA,
USA) or a GE Vivid 7 (GE-Vingmed Ultrasound,
Horten,
Norway) ultrasound system.
An attending cardiologist (J.S.
Park) with five years of experience in echocardiography evaluated each examination in a blinded fashion.
A comparison of patients with and without CT-detected CAD was performed using an independent t-test for continuous variables and the x2 test for categorical data.
Variables that achieved significance in univariate analyses were selected for logistic regression analysis to evaluate the relationship between CV risk factors and CAD.