We performed MDCT after giving water solution of contrast medium per os and before and after i.v. contrast medium.
We examined the patient with suspicion of for example stomach tumor, inflammation of the biliary ducts, dysfunction stent of the bile duct (two patients) and inflammatory bowel disease.
All the patients suffered from purulent processes (hepatic abscess, gangrenous cholecystitis, abscess between small bowel loops, gall bladder empyema).
Case 1.
• 29 year old patient with recurrent fever and abdominal pain suspected of acute cholangitis.
• In ultrasound examinations performed earlier gallbladder was filled with dense bile.
• Laboratory abnormalities:
- elevated transaminase and total bilirubin level, GGTP
- leucocytosis
- CRP elevated level.
• ERCP examinations without stones in bile duct, but the decision of sphincterotomy was made.
• After procedure normality of bile level was obtained, but patients still had fever ( 39 C).
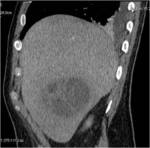
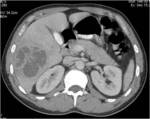
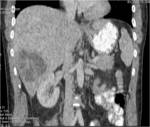
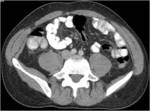
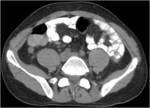
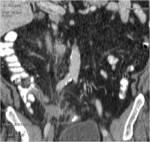
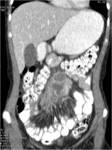
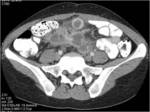
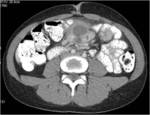
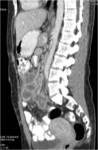
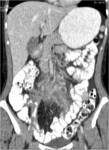
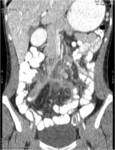
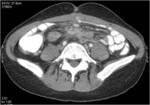
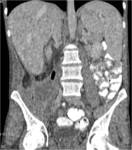
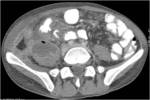
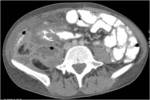
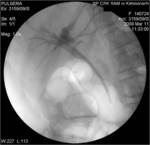
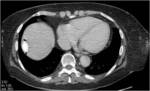
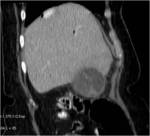
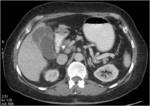
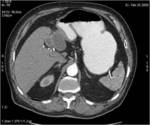
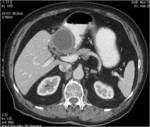
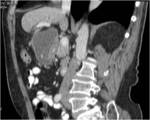
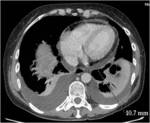
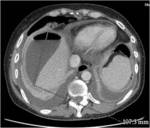
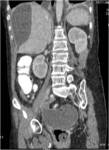
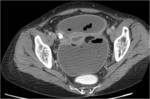
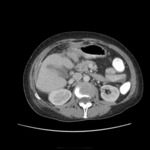
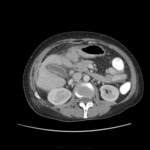
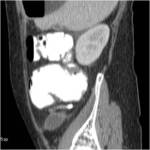
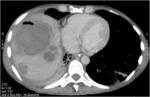
• Patient underwent CT examinations of abdomen (see images 1-3).
Abdominal abscess:
• Collection of pus in liver
• May be solitary or multifocal
• Round, well- defined hypodense lesion
• Large abscess may contain multiple septa
• Capsule and septal enhancement
• May contain air bubbles
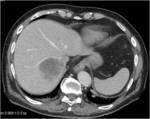
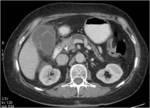
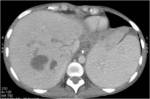
Differential diagnosis:
• Hepatic amebic abscess
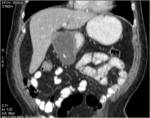
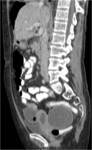
• Metastases (see image 4)
• Hepatic hydatid cyst
• Biliary cystadenocarcinoma
After one month rehospitalisation by reason of fresh blood in stool.
On day of admission to hospital:
• No signs of fever, vomiting, nausea or abdominal pain.
• In laboratory test normal morfology (leucocytosis: 5,32 10e3/ul ).
• After second day in hospital ,patient complained of : pain in RLQ , peritoneal irritation at Mc Burney point.
• In laboratory test:
elevated leucocytosis but normal CRP level.
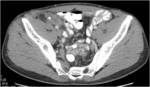
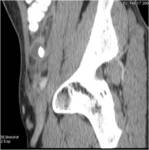
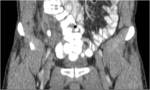
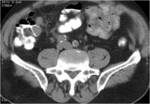
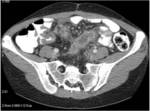
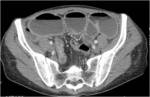
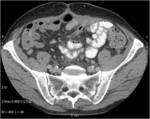
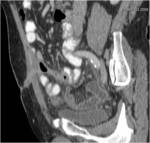
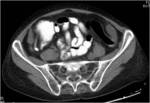
• After surgical consultation patient underwent CT of pelvis (see images:5,6,7)
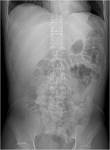
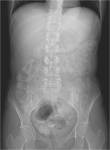
• A retrospective analysis on abdomen CT done during first hospitalisation confirmed decreased density of periappendiceal fat due to inflammatory process on axial scan and appendicolith was visable on frontal scout topogram (see images 8,9,10)
• The diagnosis of appendicitis and liver abscess due to acute inflammation of appendix was made
Appendicitis:acute inflammation of appendix due to obstruction of lumen
• CT is the most sensitive imaging technique to evaluate appendicitis and its complications ( abscess formations , perforations, inflammatory fluid collections)
• Most typical CT findings:
- dilated appendix ( more than 7 mm)
- decreased enhancement of wall with its thickening
- appendicolith may be visible
- decreased density of periappendiceal fat due to inflammatory process
- lymphadenopaty
- fluid collection or abscess formation.
Differential diagnosis:
• Cecal diverculitis
• Inflammatory bowel disease
• Mucocele
• Adenocarcinoma
• Carcinoid
Case 2.
• 26 year old patient with suspected Crohn's disease with fever (38,8 C) and abdominal pain.
• In anamnesis : laparoscopy cyst of ovary removal, since then abdominal pain and subfebrile body temperature.
• Recent gynaecological examination reveals no pathological changes.
• In physical examination : muscular defense in middle and lower abdomen. • In laboratory date : leukocytosis 20,32 10e3/ul, CRP 189,54 mg/l.
• In ultrasound examinations of abdomen between loops fluid collection.
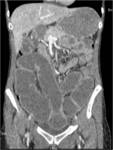
• Abdomen and pelvis CT examination besides big abscess between loops reveals bowel wall thickening areas of ileo – colonic ( see images:
13-21).
• Crohn's disease was confirmed by histological examination.
Imaging findings in Crohn’s disease:
• Bowel wall thickening asymmetric ,discontinuous
• Areas of ileo – colonic
• Enhancement of the diseased wall after iv contrast medium
• Luminal narrowing and prestenotic dilatation
• Fibrofatty proliferation
• Comb sign – increased number of mesenteric vessels
• Double – halo sign ( increased attenuation of mucosa and muscularis connected with inflammatory process and decreased density of submucosa due to edema)
• Fistulas
• Mesenteric lymphadenopaty
• Abscess and plegmons.
Differential diagnosis in Crohn's disease:
• infectious enterocolitis ( yersiniosis, tuberculosis)
• eosinophilic enteritis
• ulcerative colitis
• radiation enteritis
• lymphoma
Complications:
• Toxin megacolon
• Perforation
• Obstruction (see images 22,23)
• Abscess formation (see images 24,25,25)
• Fistulas (see images 26,27)
Case 3.
• Urgent admission to the hospital. 59 year old patient with suspected obstruction of billary catheter and adenocarcinoma of pancreas head
• For two days abdominal pain in upper – right quadrant, without fever and without jaundice
• In physical examination : tenderness in upper – right quadrant
• In laboratory date :
- leukocytosis 21,50 10e3/ul
- CRP level 248 mg/l
- bilirubin 1,03
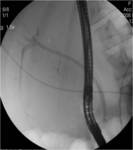
• In ERCP : Common billary duct was constricted, catheter was obstructed (see image 29).
• After filling in billary tract with contrast medium a cavity in right lobe of the liver become visible because of that CT examination was done ( see images 30-33).
Gangrenous or necrotizing cholecystitis is a severe advanced form of acute cholecystitis.
• Increased intraluminal pressure may produce gallbladder wall ischemia and ultimately necrosis, resulting in gangrenous cholecystitis.
• Clinical and laboratory characteristics are often nonspecific and indistinguishable from those in patients with acute cholecystitis without gangrene
CT findings:
• gas in the wall or lumen
• intraluminal membranes
• asymetric wall thickening
• pericholecystic abscess or fluid
• hemorrhage into the lumen
• inflammation in pericholecystic fat.
Complications of gangrenous or necrotizing cholecystitis:
• Perforation is more common than in uncomplicated cholecystitis, leading to increased morbidity and mortality.
Case 4.
• 85 year old male admitted on gastrological ward in order to diagnostic tumor in upper abdomen.
• Previous history of hypertonia arterialis, ischemic heart disease, chronic obstructive pulnonary disease, atherosclerosis, hypertrophy of prostate, varicose veins of the lower extremities.
• During previous hospital admission esophagogastroduodenoscopy was performed. It showed mass on greater curvature of the stomach bulding into the lumen o f the stomach and pressed on pylorus. Also ulcer in corpus of stomach was present.
• CT of abdomen was performed (see images 34-37).
• After surgical consultation patient was immediately qualified to operation.
Gallbladder empyema:
• occurs when pus fills the distended and inflamed gallbladder
• typically occurs in diabetic patients-it may give similar symptoms to intra-abdominal abscess
• computed tomography reveals this pus-filled gallbladder content to have greater attenuation than bile
• but US and CT findings are not specific for empyema
• at MR imaging heavily T2-weighted imaging is sensitive to demonstrate purulent bile
• in same cases percutaneous needle aspiration of the gall-bladder may be necessary to establish the diagnosis
• Data from operating card: gallbladder empyema containing gallstone infiltrating of pylorus and duodenum.
Case 5.
• 57 year old female with abdominal pain and low grade fever.
• In blood test high leukocytosis, elevated level of plates, bilirubin, ALAT.
• In physical examination : tenderness in upper abdomen without symptoms of peritonitis.
• X-ray picture of abdomen was performed, in order to explain the changes seen on the plain radiograph the CT scan was performed ( see images 38-49).
CT examinations of abdomen and pelvis reveal:
- air bubbles adjacent to pylorus and decreased density of fat around stomach due to inflammatory process which suggest perforation of gastrointestilnal tract in pylorus area
- liver-abscess
- large abscesses within pelvis
The patient was urgently operated:
• Diagnosis: rupture of stomach ulcer with peritonitis, abscesses within abdominal cavity: between diaphragm and right lobe of liver and in pelvis, Meckel’s diverticulum.
CT Findings in perforation of stomach ulcer :
• Wall thickening or luminal narrowing of stomach
• Infiltration of surrounding fat
• extraluminal intra or retroperitoneal gas
Case 6.
• 33 year old male was urgently admitted to hospital because of dysfunction of biliary stents
• Since June she was undergoing medical treatment and diagnosed for jaundice and skin pruritus.
• Diagnosis of stricture of bilary duct vague etiology and cholangitis was made.
• State post endoscopic retrograde cholangiopancreatography and the insertion of a stent to assist the drainage of bile
• Since 4 days: fever, rising jaundice, vomiting, RUQ pain
• In physical examination :
- tenderness in upper abdomen
- yellowish skin and sclera
• Laboratory data:
- abnormal liver function:
AspAT 45 U/L ,ALAT 57 U/L , GGTP 192 U/L , ALP 741 U/L , bilirubin 24.76 mg/dL
-leukocytosis 25.01 10e3/uL
- CRP 226.88 mg/l
In urine : bilirubin, urobilinogen
• After endoscopic retrograde cholangiopancreatography and exchanging stent ( see image 50), CT of abdomen was made (see images 51-52).
Ascending cholangitis:
• most commonly results from infection of an obstructed bile duct due to bile duct stones
(less common with a malignant obstruction)
• less often caused by biliary constriction from other causes (trauma or primary sclerosing cholangitis.
CT findingsi in ascending cholangitis:
• Dilatation of intra or extra hepatic bile ducts
• Intraductal material : stone or purulent bile
• Inhomogeneous enhancement of hepatic parenchyma was reported
Complications :
• Liver abscess - jaundice and marked elevation of alkalinephosphatase are common with a biliary tract abscess origin.