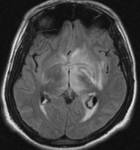
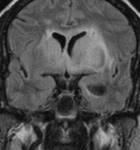
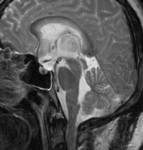
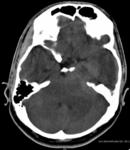
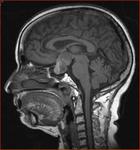
We were able to recognize the clinical manifestations and key MR imaging features of various hypothalamic lesions.
We came across developmental abnormalities (craniopharyngioma,
hamartoma, dermoid and epidermoid cysts, Rathke cleft cyst[RCC], colloid cyst, primary tumors of the central nervous system (CNS) (hypothalamic-chiasmatic glioma, Pituitary adenoma), systemic tumors affecting CNS, inflammatory and granulomatous diseases (lymphocytic hypophysitis) and lesions arising from surrounding structures.
Of the total number of patient studied during 2003-2009, 127 patients had hypothalamic and juxtasellar lesions between the age of 4 -75years .Of this, we excluded 20 patients who did not turn up for follow or refused surgery.107 cases of hypothalamic and juxtasellar abnormalities were pathologically or medically proved on follow up imaging.
Pituitary macroadenoma : 52 cases
Meningioma : 14 cases,
Craniopharyngioma : 13 cases,
Granulomatous disease: 5 cases,
Metastatic disease : 4 cases,
Chiasmatic glioma : 7 cases,
Lymphocytic Infundibuloneurohypophysitis: 3 cases,
Hypothalamic glioma : 3 cases,
Dermoid : 2 cases,
Rathke cleft cyst : 1 cases,
Colloid cyst : 1 cases,
Hypothalamic hamartoma : 2 cases.
The MR imaging characteristics of most common lesions were sufficiently distinct to allow them to be differentiated from each other. Other characteristics such as extrasellar versus intrasellar location, nature of contrast material enhancement, the presence of cystic components, bony changes and clinical findings permitted further differentiation among the various other abnormalities.
Some hypothalamic lesions showed remarkable consistency in location, such as hamartoma. A thickened contrast-enhanced infundibulum is the most typical manifestation of, lymphocytic hypophysitis and sarcoidosis.
Involvement of the optic chiasm and optic nerves by hypothalamic tumors may point to the diagnosis of hypothalamic-chiasmatic glioma. Larger hypothalamic lesions may extend into the pituitary fossa and parasellar region. The differential diagnosis for such lesions includes pituitary adenomas with suprasellar extension. However, the most common masses in the hypothalamic region in our experience were suprasellar pituitary adenoma, craniopharyngioma, and hypothalamic- chiasmatic glioma; other lesions like dermoid and hamartomas were less commonly seen.
Contrast-enhanced MR imaging also helped in differentiating nonneoplastic cysts (eg, arachnoid, epidermoid, and colloid cysts) from cystic neoplasms (eg, RCC, craniopharyngioma, cystic pituitary adenoma) within the hypothalamic region. Unlike nonneoplastic cysts, cystic tumors usually show cyst wall enhancement.
Contrast-enhanced MR imaging also showed a wide variety of enhancement patterns. Classically, hypothalamic hamartomas showed no contrast enhancement. This finding is fairly characteristic and is helpful in differentiating hamartomas from other lesions. Enhancement of other hypothalamic lesions ranged from homogeneous (germinoma) to patchy and irregular (craniopharyngioma, glioma). Associated findings of leptomeningeal enhancement with multiple foci of parenchymal enhancement pointed to infection /sarcoidosis.
Enhancement pattern:
No enhancement
- Hamartoma
- Rathke cleft cyst
- Dermoid cyst
- Epidermoid cyst
- Arachnoid cyst
- Colloid cyst
Homogenous enhancement
Inhomogeneous enhancement
Peripheral enhancement
Individual lesions:
Craniopharyngioma
- Arises from remnant of craniopharyngeal duct
- Anywhere from sella to 3rd ventricle
- Adamantinomatous type - 2nd decade ; calcification and cystic lesions are common
- Solid, papillary type - 5th decade
- Males
- 90% rule – children, cystic, calcification, suprasellar.
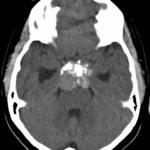
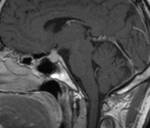
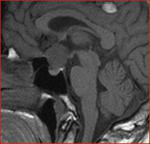
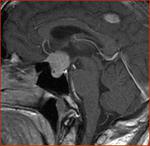
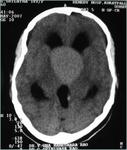
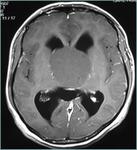
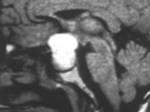
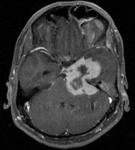
Fig(1-3)
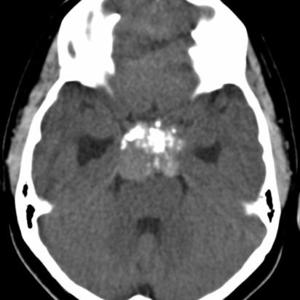
Fig.: Partially calcified sella mass- craniopharyngioma
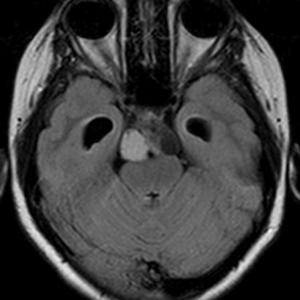
Fig.: Craniopharangioma with cyst and calcification
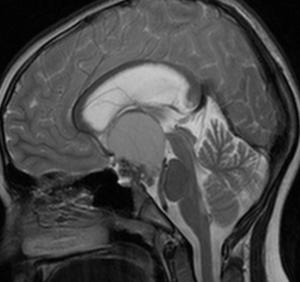
Fig.: Craniopharangioma- Sag T2
Hypothalamic Hamartoma
- Developmental malformation
- Children
- Males
- Intrahypothalamic – gelastic seizures
- Parahypothalamic – tuber cinerum – precocious puberty
- Signals same as grey matter
- Isointense on Ti -weighted images and isointense or mildly hyper intense on T2-weighted images
- No cystic changes, no calcification, contrast enhancement.
- The lesions are stable in size over time.
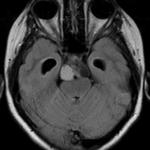
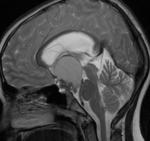
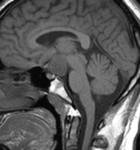
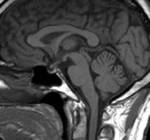
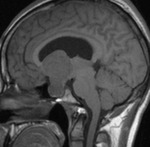
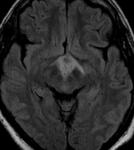
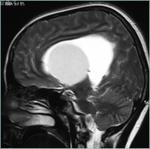
Fig(4,5)
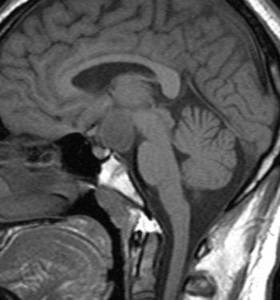
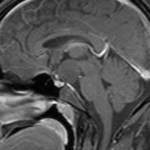
Fig.: Saggital T1-Hypothalamic Hamartoma
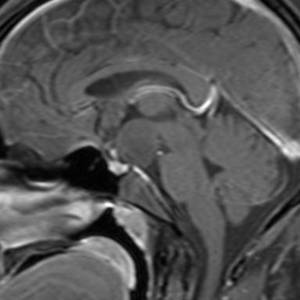
Fig.: Non enhancing Hypothalamic hamartoma
Hypothalamic chiastmatic glioma
- M=F
- 20-40years
- Suprasellar location
- Associated with NF1
- Hypointense in T1, hyperintense in T2
- Inhohogenous contrast enhancemen
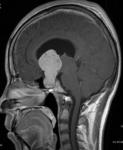
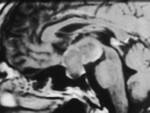
Fig6-7
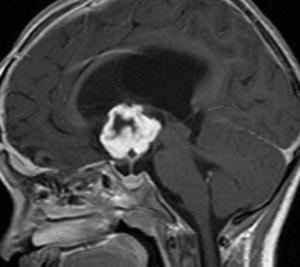
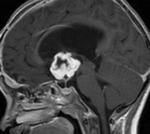
Fig.: Enhancing hypothalamic glioma.
Lymphocytic Infundibuloneurohypophysitis
- Autoimmune inflammatory condition
- Adults,more in females wih hypopituitarism in peripartum period
- MR shows diffuse enlargement of hypothalamus and infundibulum
- Typically shows uniform contrast enhancement
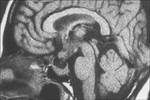
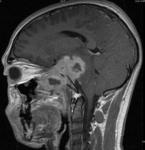
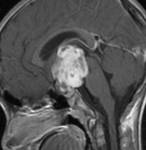
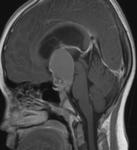
Fig8-10
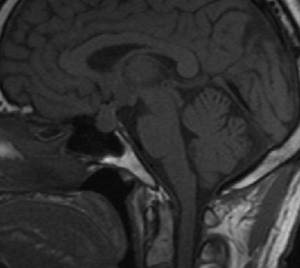
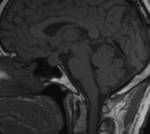
Fig.: Ti sagittal-Diffuse enlargement of pituitary ,infundibulum and hypothalamus.
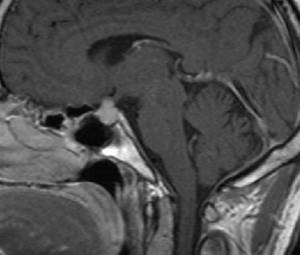
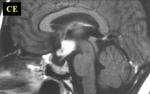
Fig.: CE sagittal T1- lymphocytic hypophysitis.symmetric enlargement of the pituitary gland with homogeneous contrast enhancement.
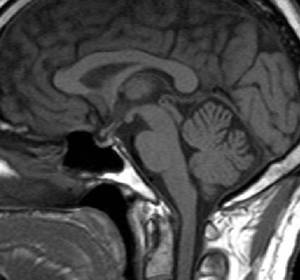
Fig.: Lymphocytic hypophysitis-complete shrinkage of mass after high glucocorticoid dose
Pituitary macroadenoma
- More or less isointense to the normal gland and brain parenchym
- Cystic or hemorrhagic components are present. Hemorrhage is depicted better by MR than CTand the signal characteristics suggest the age of the hemorrhage.
- Pituitary apoplexy , acute hemorrhagic necrosis of a macroadenoma, and patients may present with symptoms related to mass effect of the hematoma or associated subarachnoid hemorrhage
- Macroadenomas - homogeneous enhancement and are clearly demarcated from normal suprasellar structures
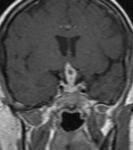
Fig11-12
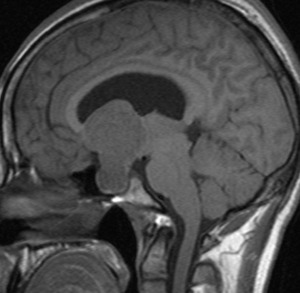
Fig.: Pituitary macroadenoma with suprasellar extension
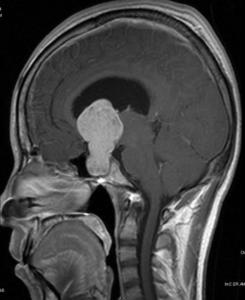
Fig.: Enhancing pituitary macroadenoma with suprasellar extension.
Meningioma-
- Suprasellar mass
- 40 to 50 year olds
- M>F
- Visual loss is the most common symptom
- CT shows a hyperdense lesion originating from the tuberculum sella, planum sphenoidale, or sphenoidal ridge with hyperostosis
- Isointense on precontrast T1-weighted images and with a bright enhancement after gadolinium contrast.
- A dural tail sign, on contrast T1 images, is suggestive of Meningioma.
Fig13-14
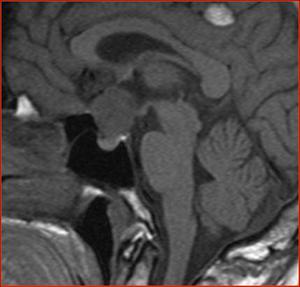
Fig.: T1 isointense Meningioma
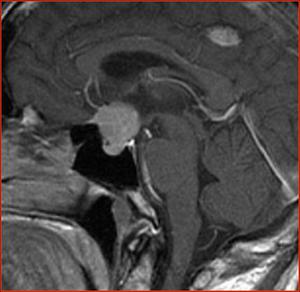
Fig.: Enhancing meningioma with dural tail sign
Tuberculosis-
- Pituitary tuberculomas are rare
- Most patients have other signs of active tuberculosis, Patients are affected at any age and there is female predominance
- Visual loss and headache are the most common symptoms
- MRI shows thickening of pituitary stalk with enhancement with granulomas in brain parenchyma
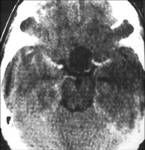
Fig 15-16
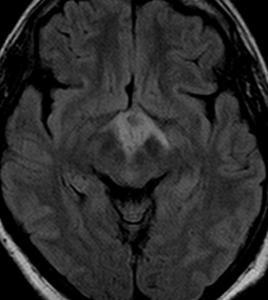
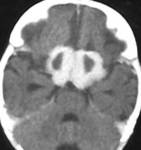
Fig.: TB granuloma involving hypothalamus,optic chiasma and optic tract
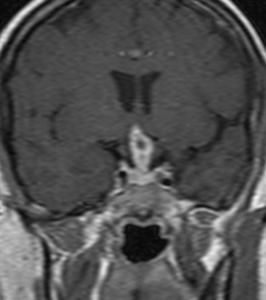
Fig.: TB granuloma involving hypothalamus ,optic chiasma and optic tract.
Colloid cyst
- Slow growing
- Neuroepithelial or endodermal origin
- Rare Suprasellar,usually anterosuperior to 3rd ventrical
- 5-6 decades
- T1 hyperintensity,T2 iso-hypointensity
- No contrast enhancement or calcification.
- Fig 17-19
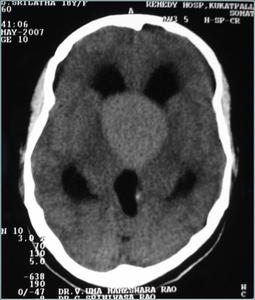
Fig.: Hyperdense colloid cyst on CT
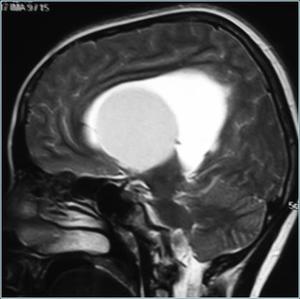
Fig.: Colloid cyst on sagittal T2
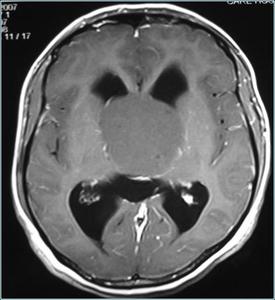
Fig.: Post contrast T1 image showing non-enhancing colloid cyst
Dermoid cyst
Fig 20-21
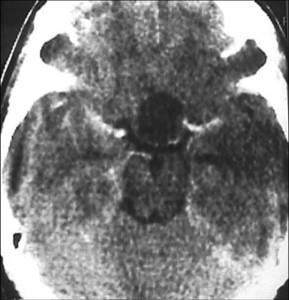
Fig.: Dermoid cyst with fatty attenuation on CT
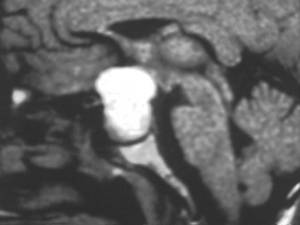
Fig.: Sag T1 image showing hyperintense dermoid cyst