METHODS
A review of parotid tumours which were discussed at combined clinical-radiological-pathological sessions in our institution between January 2003 and November 2008 revealed 10 cases of histopathologically confirmed parotid gland oncocytomas.
The gender,
age at diagnosis,
clinical presentation,
type of surgical resection (superficial vs.
total parotidectomy) and recurrence during patient follow-up of all 10 cases were recorded retrospectively.
Institutional review board approval was obtained prior to the study.
All 10 cases were imaged using the TOSHIBA Aquilion multislice CT SCAN SYSTEM with the scan level extending from the level of the external auditory canal to the hyoid bone,
and the plane of the scan parallel to the hard palate.
Five of the 10 cases were imaged using the 4-slice Toshiba system.
Images were acquired at 135 kV and 250 mA with a pitch factor of 3.5 and a total scan time of 30 seconds.
Axial sections of 3 mm thickness were reconstructed with use of the FC 10 soft tissue algorithm.
A bolus intravenous dose of 70 ml of non-ionic contrast (350 mg I/ml) was administered to patients at an injection rate of 1.5 ml per second.
Scanning was initiated 47 s after the onset of contrast injection.
The remaining 5 patients were imaged using the 64-slice Toshiba system.
Images were acquired at 120 kV and 200 mA with a pitch factor of 0.8 and a total scan time of 7 seconds.
Axial sections of 3 mm thickness were reconstructed with the use of the FC 04 soft tissue algorithm.
A bolus intravenous dose of 50 ml of non-ionic contrast (350 mg I/ml) was administered to patients at an injection rate of 1.5 ml per second.
Scanning was initiated 50 s after the onset of contrast injection.
A senior head and neck radiologist retrospectively reviewed the CT images of the 10 confirmed cases of parotid gland oncocytomas.
The tumours were then categorised in terms of location,
size,
margins,
contour and pattern of enhancement.
Tumour location was defined as involving the superficial,
deep or both the superficial and deep lobes of the parotid gland.
The intraparotid segment of the facial nerve creates a surgical plane that divides the gland into superficial and deep lobes,
but is not routinely identified even with high-resolution imaging.22 The course of the intraparotid facial nerve can be inferred by identification of the retromandibular vein within the gland since the nerve lies just lateral to this vessel.17,
22 The parotid oncocytomas in our series were classified as involving the superficial lobe if the tumor was located lateral to the retromandibular vein; and as involving the deep lobe if the tumor was located medial to the retromandibular vein or showed extension medially through the stylomandibular gap.
Each patient was also evaluated for synchronous bilateral and multifocal disease.
The size of the tumour was expressed in terms of maximal axial dimensions measured to the nearest millimeter.
The largest lesion was measured in cases of multifocal disease.
The tumour was deemed to have ‘sharp’ margins if it was well demarcated throughout its circumference and ‘indistinct’ margins if otherwise.
A tumour was considered to have a ‘lobulated’ contour if it demonstrated surface undulations or a ‘smooth’ contour if it lacked such undulations.
As pre-contrast images were not acquired,
a tumour was presumed to be enhancing if it showed a mean attenuation of more than 100 HU and appeared significantly more hyperdense than the native parotid parenchyma and ipsilateral muscles on visual comparison. The enhancement pattern of the tumours was categorised as either homogenous or inhomogeneous.
Tumours which showed inhomogeneous enhancement were further described as demonstrating either a non-enhancing ‘curvilinear cleft’ or ‘cystic component’,
the latter defined as having a mean attenuation of 20 HU or less and being round or oval in appearance.
RESULTS
Table 1 (Figure 7) shows the age and gender distribution as well as the radiological features of the parotid gland oncocytomas.
Of the 10 cases,
7 were women and 3 were men aged between 49 and 74 years (mean age of 61 years).
All 10 patients initially presented with slowly enlarging painless parotid masses over a period of 6 to 96 months (mean 30 months),
2 of whom were found clinically to have bilateral parotid masses.
CT revealed a unilateral solitary tumour in 4 patients,
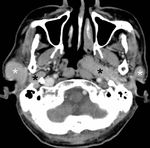
unilateral multifocal disease in 1 patient and synchronous bilateral multifocal tumours (Figure 1) in the remaining 5 patients.
Three of the 5 patients found to have bilateral parotid tumours following CT had presented with unilateral parotid masses and were clinically occult for bilateral disease.
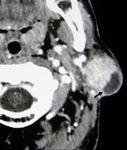
The tumour was limited to the superficial lobe of the parotid gland in the 4 patients with unilateral solitary tumours on CT (Figure 2),
while both the superficial and deep lobes were involved in the other 6 patients.
The maximum axial diameter of the tumors ranged from 6 to 66 mm with a mean of 19.8 mm.
All of the tumors showed sharp margins.
The oncocytomas in 4 of the cases demonstrated a lobulated contour with the tumours in the other 6 cases showing smooth contours.
Three patients had large parotid oncocytomas which involved the deep lobe and showed extension to the parapharyngeal space through the stylomandibular gap.
The contours of these large oncocytomas were distorted by surrounding anatomical structures such as the styloid process and surrounding muscles,
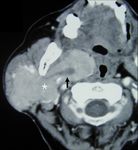
giving rise to the ‘deformable’ appearance of the tumours (Figure 3).
The tumors in 4 of the cases showed homogenous enhancement.
Heterogeneous enhancement was demonstrated in the remaining 6 cases (60 %),
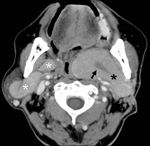
out of which a central non-enhancing curvilinear cleft was seen in 4 cases (Figures 4 and 5) and a cystic component seen in the other 2 cases (Figure 6).
None of the tumours showed calcification.
Cut sections of the gross specimens of the tumours which showed central non-enhancing curvilinear clefts revealed central grey-white scars which correlated microscopically with hyalinised and fibrous tissue.
Cystic degeneration was noted histopathologically with respect to the 2 tumours demonstrated to have non-enhancing cystic components on the CT scan.
We concluded that these central scars and areas of cystic degeneration would most likely be responsible for the non-enhancing curvilinear cleft and cystic component detected on CT respectively.
Seven of the patients in our series underwent either superficial or total parotidectomy depending on the location of the tumour.
Ultrasound-guided core-needle biopsy was used to obtain the histopathological diagnosis in the 3 patients who declined surgery.
The follow-up duration of the 7 patients who underwent surgical resection ranged from 12 months to 19 months with a mean of 18 months.
At the time of the last follow-up,
no clinical evidence of local tumour recurrence was detected in these 7 patients.