PART I - PULMONARY TBC
PRIMARY PULMONARY TBC
It’s seen in patients not previously exposed to M.
tuberculosis and it’s most common in infants and children.
It has the highest prevalence in children under 5 years of age.
Although primary tuberculosis is the most common form of pulmonary TBC in infants and children,
it has been increasingly encountered in adult patients and now accounts for 23%–34% of all adult cases of tuberculosis.
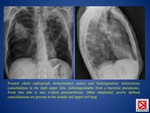
Chest radiography (FIG.
1) remains the mainstay of diagnosis; however,
normal radiographic findings may be seen in up to 15% of patients with proved tuberculosis.
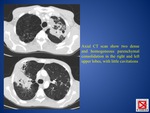
High-resolution CT (FIG.
2) is more sensitive.
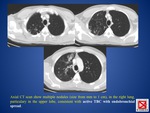
Primary tuberculosis typically manifests radiologically with these main entities:
- parenchymal disease
- lymphadenopathy
- pleural effusion (one-fourth of patients,
usually unilateral; possible calcification),
PNX (FIG.
1)
- miliary disease (1-7%,
overall in elderly,
infants and immunocompromised)
- atelectasis (either lobar or segmental,
frequently seen in children under 2 years of age)
Typical presentation → “primary complex”:
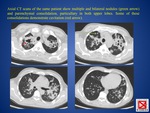
a) parenchymal disease (FIG.
1 and 2): dense,
homogeneous parenchymal consolidation that affects the areas of greatest ventilation → the most common sites are the middle lobe,
the lower lobes,
and the anterior segment of the upper lobes; its appearance is often indistinguishable from that of bacterial pneumonia.
b) lymphadenopathy (up to 96% of children and 43% of adults): typically unilateral and right sided,
involving the hilum and right paratracheal region,
although it is bilateral in about one-third of cases.
Evolution of primary complex:
- in approximately two-thirds of cases,
the parenchymal focus resolves without sequelae (it can take up to 2 years);
- radiologic scar that can calcify in up to 15% of cases,
entity that is known as a Ghon focus;
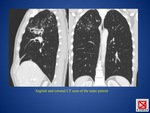
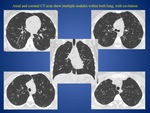
- persistent masslike opacities called tuberculomas,
that can cavitate (approximately 9% of cases) (FIG.
2)
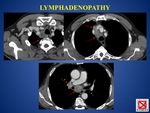
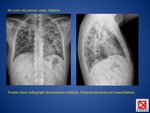
LYMPHADENOPATHY (FIG.
3)
Although lymphadenopathy is usually associated with other manifestations of tuberculosis,
it can be the sole radiographic feature,
a finding that is more common in infants and decreases in frequency with age.
Nodes involved often calcify (6 month/>).
The combination of calcified hilar nodes and a Ghon focus is called a Ranke complex and is suggestive of previous tuberculosis,
although it can also result from histoplasmosis.
CT is more sensitive than chest radiography for assessing lymphadenopathy.
Any nodes greater than 2 cm in diameter generally have a low-attenuation center secondary to necrosis at CT (FIG.
3).
This finding is highly suggestive of active disease,
in the appropriate clinical setting.
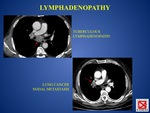
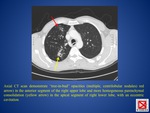
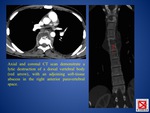
The radiologic differential diagnosis for tuberculous lymphadenopathy includes metastases (FIG.
4) and histoplasmosis in endemic areas.
POST-PRIMARY TBC
The term post-primary tuberculosis is generally used to refer to both re-infection with (30-60%) and reactivation of tuberculosis (40-70%) in patients with immunodepression.
It remains primarily a disease of adolescence and adulthood (40-60 years old) and it occurs in patients previously sensitized to M.
tuberculosis.
Primary tuberculosis is usually self-limiting,
whereas post-primary tuberculosis is progressive,
with cavitation as its hallmark,
resulting in hematogenous dissemination of the disease as well as disease spread throughout the lungs.
The features of primary and post-primary tuberculosis may overlap.
However,
the distinguishing features of post-primary tuberculosis include:
- predilection for the upper lobes
- absence of lymphadenopathy
- presence of cavitation
CT FINDINGS
Parenchymal disease (the earliest finding,
FIG.
7,
8 and 9): patchy,
poorly defined consolidation,
particularly in the apical and posterior segments of the upper lobes,
bilateral in one-third of cases.
Cavitation (FIG.
9 and 10): the hallmark of post-primary tuberculosis,
that affects about 50% of patients and indicates a high likelihood of activity.
The cavities typically have thick,
irregular walls,
which become smooth and thin with successful treatment.
Cavities are usually multiple and occur within areas of consolidation.
Centrilobular nodules and branching centrilobular areas of increased opacity (FIG 5,
6 and 7): if there is airway disease and,
in particular,
endobronchial spread of infection (most common complication of TBC cavitation),
“tree-in-bud” opacities may develop; this is characteristic but non pathognomonic for active TBC (can also be seen with viral,
fungal,
and parasitic infections and also in allergic bronchopulmonary aspergillosis).
Airway involvement: characterized by bronchial stenosis,
leading to lobar collapse and by traction bronchiectasis.
Pleural effusion (18%,
usually with parenchymal disease; possible calcification).
MILIARY DISEASE
Miliary tuberculosis occurs in 2% to 6% of primary TBC and also occur in post-primary TBC,
when the host’s defence mechanisms are overwhelmed.
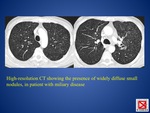
High-resolution CT (FIG.
11) is more sensitive than conventional radiography and show in 85% of cases a mixture of both sharply and poorly defined nodules of 1 to 2 mm,
widely disseminated throughout the lungs (haematogenous spread of infection),
with a slight lower lobe predominance.
The nodules usually resolve within 2-6 months with treatment,
without scarring or calcification.
PART II - EXTRA-PULMONARY TBC
PART IIA - MUSCULOSKELETAL TUBERCULOSIS
Musculoskeletal system is involved in only 1%–3% of cases of TBC; however,
the resultant bone and joint destruction is the cause of severe morbidity and of neurologic sequelae in spinal involvement.
It affects patients of all ages and most frequently the spinal column,
pelvis,
hip,
and knee.
Diagnosis is often difficult (there are no pathognomonic radiologic features),
with an average delay of 16-19 months between the onset of symptoms and reported diagnosis.
Only histologic analysis and tissue culture can help confirm the diagnosis.
MR imaging is more sensitive than conventional radiography and CT in assessing the extent of bone and joint involvement and for the diagnosis and assessment of tuberculous spondylitis (high sensitivity to soft-tissue abnormalities).
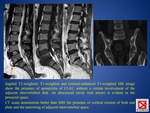
A) TUBERCULOUS SPONDYLITIS (FIG.
12,
13 and 14)
- 50% of skeletal tuberculosis involves the spine (probably from hematogenous spread via the venous plexus of Batson),
aboveall the lower thoracic and upper lumbar levels.
- infection usually begins in the anterior part of the vertebral body adjacent to the end plate → demineralization and scalloping of the end plate → spread of infection to adjacent intervertebral disk → potential spread to additional spinal segments and subsequential spread into the paraspinal tissues,
with formation of a paravertebral abscess (Pott’s abscess,
FIG.
12 and 13) +/- with calcification;
- if there is anterior subligamentous involvement of the spine,
infection can extend both superiorly and inferiorly to more segments,
with sparing or delayed involvement of intervertebral disks;
- characteristically associated with little or no reactive sclerosis/local periosteal reaction,
in contrast to pyogenic infections;
- rarely affects the posterior vertebral elements (including the pedicles),
in contrast to metastasis
- in the early stage,
imaging appearances are entirely non specific; in differentiating TBC from pyogenic infection,
the clinical picture is important: insidious onset of symptoms,
a normal erythrocyte sedimentation rate,
relevant respiratory symptoms,
and slow disease progression (favoring the diagnosis of tuberculosis)
B) TUBERCULOUS OSTEMYELITIS (EXTRASPINAL TBC OSTEOMYELITIS) (FIG.
15)
- tuberculous osteomyelitis is usually hematogenous in origin and the isolated form in the absence of associated tuberculous arthritis is relatively rare
- is most commonly seen in bones of the extremities (femur,
tibia),
including the small bones of the hands and feet
- in long,
tubular bones,
often involves the epiphyses; in children metaphyseal foci can involve the growth plate (this feature differentiates tuberculosis from pyogenic infection)
- initial radiologic appearance is similar to that of other types of osteomyelitis and includes foci of osteolysis with varying degrees of eburnation and periostitis.
- the diagnosis is usually made after considerable delay,
and radiographic changes are seen at clinical presentation; in contrast,
in pyogenic infection,
radiographic changes occur 2-3 weeks after presentation.
C) TUBERCULOUS ARTHRITIS (FIG.
16)
- may be secondary to direct invasion from an adjacent focus of tuberculous osteomyelitis or may result from hematogenous dissemination
- is typically monoarticular and primarily involves large weight-bearing joints (hip and knee)
- the imaging findings are similar to those of other infectious and inflammatory arthritides and are,
therefore,
non specific; these findings include osteopenia,
synovitis and other soft-tissue swellings,
marginal erosions,
and varying degrees of cartilage destruction
- the end result is usually fibrous ankylosis of the joint
- the differential diagnosis includes pyogenic and fungal infections factors → favoring a diagnosis of TBC include insidious onset,
minimal sclerosis,
the relative absence of periosteal reaction and bone proliferation
PART IIB - TUBERCULOSIS INVOLVING THE CNS
Most tuberculous infections of the central nervous system (neurotuberculosis,
5% of patients) are usually a result of hematogenous spread.
It results in two related pathologic processes: tuberculous meningitis (the most common manifestation,
across all age groups) and intracranial tuberculomas and abscesses.
Its prevalence is greater in immunocompromised patients.
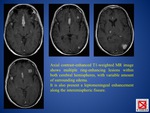
A) MENINGEAL INVOLVEMENT (TUBERCULOUS MENINGITIS)
- typical radiographic finding,
better seen at gadolinium-enhanced MR imaging than at CT → abnormal meningeal enhancement (FIG.
16)
- appearance non specific and with wide differential diagnosis: meningitis from other infective agents,
inflammatory diseases (rheumatoid arthritis and sarcoidosis) and neoplastic causes (both primary and secondary)
- most common complication → communicating hydrocephalus
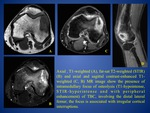
B) PARENCHYMAL INVOLVEMENT (can exist in conjunction with tuberculous meningitis)
- most common parenchymal lesion → tuberculoma (non-caseating granuloma),
solitary,
multiple,
or miliary,
anywhere within the brain parenchyma (above all within frontal and parietal lobes)
- it demonstrate homogeneous enhancement,
with irregular wall of varying thickness and in one-third with central calcification
- caseating tuberculoma with necrotic center demonstrate a ring enhancement (FIG.
17) and usually have a variable amount of surrounding edema; abscesses can be similar in appearance
PART IIC - GENITOURINARY TUBERCULOSIS
TBC may involve the genitourinary tract as a secondary site following hematogenous dissemination from the lung.
Genitourinary TBC is the most common clinical manifestation of extrapulmonary tuberculosis.
A) KIDNEYS (75% unilateral) (FIG.
18)
- the most common CT finding is renal calcification (50%)
- renal parenchymal cavitation may be detected as irregular pools of contrast material
- “moth-eaten” abnormality of calix at urography,
due to erosions
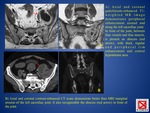
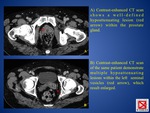
B) BLADDER (tuberculous cystitis)
It manifests as a shrunken bladder with wall thickening and reduced bladder capacity.
C) GENITALIA
- female: obstruction of the fallopian tubes (salpingitis,
94% cases) with multiple areas of constriction,
and calcified lymph nodes in the adnexal region,
endometrial adhesions with deformity and obliteration of endometrial cavity
- male: involvement of the prostate gland or seminal vesicles (FIG.
19) may lead to necrosis,
calcification,
caseation (hypoattenuating lesions at CT),
and cavitation
PART IIIC - ABDOMINAL TUBERCULOSIS
The abdomen is the most common focus of extrapulmonary tuberculosis,
with the solid viscera being affected more often than the gastrointestinal tract.
Although abdominal tuberculosis is usually secondary to pulmonary tuberculosis,
radiologic evaluation often shows no evidence of lung disease.
CT is the mainstay for investigating possible abdominal tuberculosis.
A) LYMPHADENOPATHY
The most common manifestation (FIG.
20) of abdominal TBC (55-60%),
with enlarged nodes with hypoattenuating centers and hyperattenuating enhancing rims at CT (40-60% of cases),
findings that are characteristic of,
but not pathognomonic for,
caseous necrosis.
The mesenteric,
omental,
and peripancreatic lymph nodes are most commonly involved.
B) GASTROINTESTINAL TBC (rare)
It can occur elsewhere in the small bowel,
but almost always involves ileocecal region (90% of cases),
usually both the terminal ileum and the cecum.
Rare localitations are esophagus,
stomach and proximal small bowel.
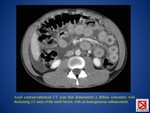
The most common CT finding (FIG.
21) is concentric mural thickening,
with associated luminal narrowing with or without proximal dilatation.
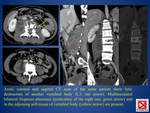
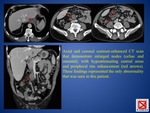
C) HEPATOSPLENIC TBC
- common in patients with disseminated disease,
either miliary or macronodular
- micronodular/miliary involvement: seen in patients with miliary pulmonary TBC,
characterized by innumerable 0.5–2.0-mm hypoattenuating nodules.
The liver appears hyperechoic at US.
- macronodular involvement: uncommon,
with liver or splenic enlargement and hypoattenuating lesions at CT,
with irregular ill-defined margins and minimal but definite peripheral contrast enhancement (imaging appearances non specific and similar to those of multiple metastases and abscesses).
At MR imaging,
these lesions are hypointense with T1-weighted sequences and hyperintense with T2-weighted sequences.
- hepatic tuberculomas eventually tend to calcify; the presence of calcified granulomas at CT in patients with known risk factors and in the absence of a known primary tumor should raise suspicion for TBC
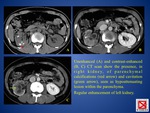
D) ADRENAL TBC
- it’s seen in up to 6% of patients with active tuberculosis.
- bilateral adrenal involvement and an Addisonian type clinical picture
- CT signs: enlarged glands associated with large,
hypoattenuating necrotic areas,
with or without dotlike calcification