A CASE-BASED APPROACH
The study material for this report consists of a cohort of women with single-lumen or double-lumen implants who underwent between January 2008 and July 2010 either one or two MRIs before removal the implants.
The MRI examination was performed at one of two MRI centres of our Hospital.
All scanners (1,5 T) were equipped with a dedicated breast coil,
which has been shown to increase both the sensitivity and specificity of MRI.
At our institution patients with breast prostheses are examined with T1-weighted Fast low Angle Shot (FLASH) 3d and T2-weighted Turbo Inversion Recovery in the Magnitude (TIRM) sequences in the axial plane.
The sagittal images are obtained with T2-weighted fat saturated and silicone excited (silicone hyperintense,
water suppressed) or water excited (silicone suppressed,
water hyperintense) TIRM sequences.
Also a coronal T2-weighted fat saturated sequence could be used.
Intravenous contrast is given in selected cases,
depending on the clinical suspicion.
The post-contrast study consists of T1-weighted fat saturated FLASH3d sequences.
CASE 1
Case History:
Magnetic resonance imaging scans of a 45-year-old woman with single-lumen silicone implants.
No informations available about implant type and implantation year.
Image analisys:
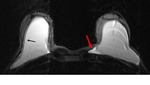
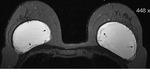
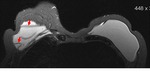
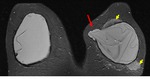
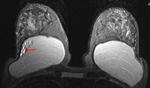
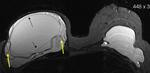
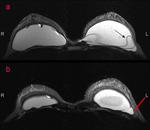
Axial T2-weighted TIRM image (Fig.
1) demonstrates a normal signal-lumen silicone implant on the left,
surrounded by a small amount of fluid.
On the outer side of the right implant there is a hypointense line running parallel to the fibrous capsule and just beneath this.
The beginning and the ending of the line can be followed to the surface of the implant.
This sign was interpreted as an uncollapsed rupture: a small amount of free silicone is on the outside of the silicone shell,
separating the shell and the fibrous capsule.
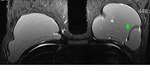
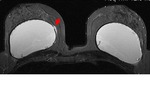
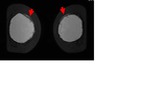
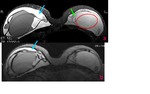
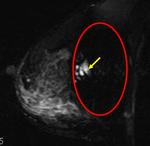
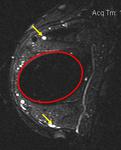
Coronal T2-weighted TIRM image (Fig.
2) confirms the presence of free silicone on the external aspect of the silicone shell.
Besides,
on the infero-medial contour of the right implant (Fig.
2),
there is a local invagination of the silicone membrane,
where the two membranes do not touch, containing a droplet of silicone.
This aspect is called "noose sign" or "key-hole sign"and it should be seen in more than one picture to arise the suspicion of intracapsular rupture.
In both axial (Fig.
1) and coronal scans (Fig.
2) one can see silicone gel surrounding the right implant shell but contained by the fibrous capsule.
This is an example of early intracapsular rupture (uncollapsed rupture).
Findings at surgery:
The MR images corresponded well with findings at surgery of a small amount of free silicone on the outside of the right implant and a small hole in the membrane.
CASE 2
Case history:
A 30 years old patient who had undergone a reductive mastoplasty and mastopexy for gigantomastia; because of the recurrence of breast ptosis,
a bilateral additive mastoplasty had been performed.
She referred to our institution for the onset of pain in her left breast.
No informations available about implant type.
Image analysis:
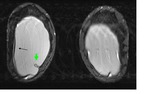
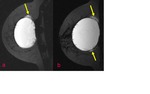
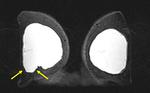
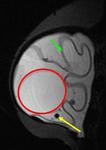
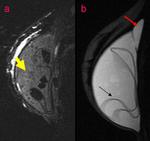
Axial T2 TIRM sequence (Fig.
3) shows a hypointense structure within the left implant that is in contact with the silicone shell and was thus classified as a radial fold.
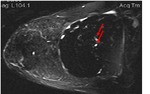
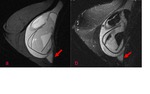
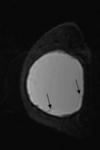
Sagittal water suppressed-silicone excited view (Fig 4) of the left breast shows a teardrop at the top of the implant and small hypointense elements in the silicone.
Sagittal silicone suppressed-water excited view at the same level (Fig 5) demonstrates that there is water mixed in the silicone gel.
The punctuate changes in signal intensity within the implants can be seen if there is an influx of serum/water into the implant through a defect membrane.
The presence of the teardrop sign and of water droplets mixed in the silicone gel led to MR diagnosis of intracapsular rupture of the left implant.
Findings at surgery:
Implant rupture was surgically confirmed.
CASE 3:
Case history:
A 57 years old patient underwent at our institution a first standard MRI examination with contrast agent.
The patients was recalled to undergo a second MRI examination for studying the breast implants because the radiologist noticed the presence of bilateral silicone abnormalities.
The patient had history of additive mastoplasty 9 years before (subglandular single-lumen silicone implants).
Image analysis:
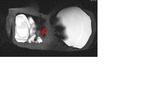
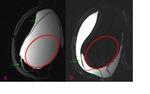
In the first MRI examination (Fig.
6) the radiologist noticed abnormal subcapsular lines at anterior and posterior margin of both the implants.
The patient was recalled and two months later,
in the axial T2 TIRM scan (Fig.
7),
a focal discontinuity of the inner side of the right fibrous capsule was noticed.
Coronal and sagittal T2-weighted water suppressed-silicone excited scans of both the implants (Fig.
8-9) showed the presence of extracaspular silicone.
Findings at surgery:
At surgery extracapsular rupture of both the implants was seen.
CASE 4:
Case history:
A 52 years old patient with previous history of left mastectomy and right additive mastoplasty for breast cancer.
She underwent breast MRI because of the onset of clinical signs and symptoms of breast implant failure on her right breast: the breast had become softer during the last few years.
Image analysis:
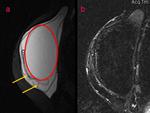
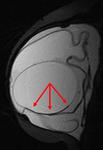
MRI examination with axial T2 TIRM sequence (Fig.
10) shows on the right breast a partially collapsed implant shell and a curvilinear low-signal-intensity line within the silicone implant.
These findings configurate the ‘linguine sign’ that is typical of intracapsular rupture.
In sagittal images of the right breast obtained with silicone signal suppression (Fig.
11b) and water signal suppression (Fig.
11a) the right prosthesis is characterized by a serum/silicone mixture; also a large lump of extracapsular silicone can be seen inferiorly.
Coronal view (Fig.
12) enhances the visualization of visible deformity in the fibrous capsule,
a finding suggestive of extracapsular spread of the silicone gel.
Findings at surgery:
At surgery the right implant was totally disrupted and siliconomas were found into the surrounding tissues because of an extravasation of silicone gel outside the fibrous capsule.
CASE 5:
Case history:
A 53 years old patient with previous history of bilateral additive mastoplasty.
No informations available about implant type.
Image analysis:
In the right breast silicone is present beyond the fibrous capsule as a nodule (granuloma/siliconoma) (Fig.
13),
but no other abnormal MR findings are present except a thick fibrous capsule (Fig.
14).
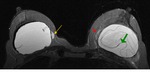
Coronal (Fig. 14) water suppressed T2-weighted image shows in the left breast extracapsular spread of silicone and a visible incoherency in the fibrous capsule on its internal side.
Extracapsular silicone can take any form,
often as a nodule or as streaks of silicone in close relation with the fibrous capsule.
On the other hand,
abnormal bulgings of the breast implants do not generate theirself a possible rupture diagnosis.
The radiologist posed the suspicion of bilateral extracapsular rupture.
Findings at surgery:
The right implant was described as intact as surgery,
but surrounded by a thick fibrous capsule.
The right lump described in the MRI examination was sent for histological examination,
where a silicone granuloma was described.
The extracapsular rupture of the left implant was confirmed.
CASE 6:
Case history:
A 59 years old patient with previous history of bilateral mastectomy and breast reconstruction with double-lumen breast implants.
She underwent MRI examination because of a recent trauma on her right breast.
Image analysis:
Axial T2-weighted TIRM image (Fig.15a) and axial T1-weighted GRE scan (Fig.15b) show right breast enlargement,
resulting in a breasts' asymmetry,
because of the presence of a fluid collection into the right implant pocket.
This collection looks hyperintense in both T2 and T1 acquisitions.
In sagittal “silicone only” (Fig.
16a) and “water only” (Fig.
16b) sequences of the right breast,
the inner lumen is well recognisable and looks intact,
while the outer membrane is partially collapsed,
floating into a collection of silicone mixed with saline and/or inflammatory/ haematic fluid.
On the basis of these findings,
the radiologist posed the suspicion of intracapsular rupture of the outer membrane of the right breast and possible intracapsular haematoma.
Sagittal views of the left breast (Fig.
17) show the presence of a double-lumen silicone implant with collapse of the outer membrane (linguine sign),
because of an intracpsular rupture.
Findings at surgery:
At surgery in the right implant pocket an haematic collection with free silicone was found.
Also the intracapsular rupture of the left implant was surgically confirmed.
CASE 7:
Case history:
A 42 years-old patient with bilateral cosmetic augmentation underwent MRI examination for the onset of severe bilateral breast ptosis.
Image analysis:
Axial T2 TIRM image (Fig.
18) shows that the intraluminal content of the right implant is somewhat inhomogeneous because of the presence of small hyperintense elements in the silicone substance; a sagittal T2-weighted MR-image of the right breast with silicone suppression (saline only sequence) (Fig.
19) reveals the presence of water/serum mixed in the silicone gel.
On the basis of these finding the radiologist posed the suspicion of intracapsular rupture of the right implant.
On the other hand,
in the coronal view (Fig.
20),
one can see an asymmetry of the augmented breasts with a large inferolateral contour deformity,
suggestive of extracapsular spread.
Finally,
in the coronal view of the left prosthesis (Fig.21),
subtle hypointense lines running parallel to the capsular profile were noticed,
arising the suspicion of an early intracapsular failure.
Findings at surgery:
At surgery extracapular silicone was found on the right,
while the left implant was intact.
CASE 8:
Case history:
A 58 years-old patient with previous history of right breast reconstruction for breast cancer and left breast augmentation.
She presented with a decrease in the right breast implant volume.
Image analysis:
Axial T2-weighted TIRM image (Fig.22) and sagittal silicone-suppressed (Fig.23) and silicone-specific (Fig.
24) T2-weighted images of the right breast show an implant with two lumens,
both of which are filled with silicone.
The inner lumen retains a nearly spherical shape,
while the outer wall of the implant appears collapsed,
suggesting an intracapsular rupture of the outer membrane. Besides,
in the sagittal silicone-specific sequence (Fig.25), the back patch of the inner lumen appears displaced along the inferior border of the inner shell and is partially separated from the outer wall.
The displacement of the back patch was considered a sign of rupture of the double-lumen implant.
Findings at surgery:
An intracaspular collection of silicone gel,
with an intact inner lumen was found at surgery.
This case illustrates that evaluating the correct position of the back patch using axial and sagittal images can help to correctly identify the type and integrity of the implant.
CASE 9:
Case history:
A 42 years-old patient with previous history of bilateral breast augmentation (single-lumen silicone implants).
She was complaining of a strange softening on her left breast.
Image analysis:
Axial T2-weighted TIRM scan (Fig.
26a) and sagittal "silicone only" sequence (Fig.
27b) reveal a totally collapsed implant shell; an abnormal signal intensity of the silicone gel is more evident in the water only sequence (Fig.
27a).
Also a large superolateral contour deformity can be observed (Figg.
26b-27b),
arising the suspicion of extracapsular spread.
Findings at surgery:
At surgery the implant was ruptured (intracapsular rupture); the free silicone was found within an intact,
but superiorly thinned fibrous capsule consistent with a herniation.
This case is an example of true-positive MR diagnosis of extracapsular rupture.