Patients
Over the period June-December 2010 we prospectively enrolled twenty-four subjects.
Of these,
twelve were patients with clinically and histologically proven hepatic cirrhosis (7 male,
5 female; age range 45-71,
mean 54.1 y-o),
addressed to Magnetic Resonance Imaging (MRI) surveillance of regenerative nodules (n=11) and hepatocellular carcinoma treated with radiofrequency ablation (n=1).
All patients showed a Child-Pugh grade A.
Median time between hepatic biopsy and MRI examination was of 7.2 months.
Remaining twelve subjects (8 male,
4 female; age range 26-53,
mean 31.4 years-old) were enrolled to form a control group without history of chronic liver disease.
The group included nine healthy volunteers and 3 patients addressed to upper abdomen MRI for the following indications: suspected intrapancreatic accessory spleen,
suspected liver haemangiomas,
assessment of multiple renal cysts.
Excluded were cirrhotic patients with known or suspected newly diagnosed hepatocellular carcinoma,
ascitic patients,
oncologic patients,
and subjects showing history of chronic liver disease without clinical and/or histological confirmation of cirrhosis.
Institutional review board approval was obtained for this study.
DWI protocol
Examinations were performed on a 3.0T magnet (Achieva; Philips Medical Systems,
Best,
The Netherlands),
equipped with a 16-elements phased-array surface coil.
All patients underwent a routine upper-abdomen MRI protocol,
including dynamic imaging after gadolinium injection in fifteen of them (no post-contrast study was performed in healthy volunteers).
Before contrast administration,
DWI was performed by using a respiratory-triggered,
single shot spin-echo echoplanar imaging sequence characterized by sequential,
independent motion probing gradients that were applied - within the same acquisition – along the frequency-encoding (x),
phase-encoding (y),
and section-select (z) directions.
B-values of 0,
400 and 800 sec/mm2 were used.
Remaining acquisition parameters are reported in Tab.
1.
Parallel imaging technique was not used,
to avoid any additional signal loss in ADC determination [12].
Spectral fat-saturation with Spectral Presaturation by Inversion Recovery (SPIR) was employed systematically,
in order to avoid chemical-shift artefacts.
A preliminary phantom study was performed to validate our system (not shown).
Image analysis and ADC determination
DWI acquisition determined 3 sets of images,
corresponding to the x,
y and z gradient directions.
Each set included images obtained at different b-values (0,
400 and 800 sec/mm2).
For each set,
two abdominal radiologists in consensus (R.G.,
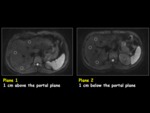
D.B.) positioned 3 regions of interest (ROI) on a slice obtained with b=0 sec/mm2,
at two different hepatic sites: a) 1 cm above the portal plane (plane 1) (ROIs on the hepatic segments IVa,
VII and VIII,
respectively); b) 1 cm below the portal plane (ROIs on the hepatic segments IVb,
V and VI,
respectively) (Fig.
1).
ROIs measured 2 cm2 each in diameter.
Positioning carefully avoided inclusion of vascular structures,
bile ducts or focal liver lesions.
No measurements were performed on the left lateral lobe,
to avoid artefacts from standing-wave effect [13] or respiratory motion.
After this preliminary operation,
ROIs were copied and pasted on same slices obtained at b=400 and 800 sec/mm2.
Signal intensity of each slice was calculated as the average of the three measurements.
On this basis,
liver ADC was calculated according to the following equation [14]:
ADC = 1/bi x ln (S0/Si) (1)
where S0 is the averaged signal sampled without diffusion probing gradients (bi = 0 s/mm2),
and Si the averaged signal sampled with bi = 400 and 800 sec/mm2,
respectively.
In summary,
in each patient we obtained two sets of liver ADC (0-400 and 0-800 sec/mm2),
at two different anatomic sites (planes 1 and 2),
along x,
y and z gradients direction.
To provide additional information regarding the influence of microcirculation changes in our model,
we estimated also the perfusion fraction f [14],
corresponding to the fraction of water within the voxel flowing in the capillary system [11,14]. According to the theory of intravoxel incoherent motion (IVIM),
b-values greater than 200 sec/mm2 make the influence of perfusion (D*) negligible in determining the ADC.
Thus,
liver ADC value becomes approximated to the pure diffusion coefficient (D) [11].
Accordingly,
f was calculated based on the equation [14]:
f = 1-exp [-b (ADC-D)] (2)
where ADC corresponds to the ADC calculated at the set of b 0-400 sec/mm2,
D was assumed to correspond to the ADC calculated at the set of b 0-800 sec/mm2,
and b is 400 sec/mm2.
Perfusion fraction f values were obtained in each patient at both planes 1 and 2,
along x,
y and z gradients directions.
Data analysis
Isotropy (or not) of the liver was assessed by comparing the differences of ADC values obtained along x,
y and z gradient directions within controls and cirrhotic patients,
at both planes 1 and 2.
After checking for data normality with the Levene’s test,
we achieved this goal by using the analysis of variance (ANOVA) for repeated measures.
Same analysis was performed to compare f values within subjects.
Furthermore,
we estimated the significance of the difference in ADC values as follows: a) within controls and cirrhotic,
by comparing ADC values between planes 1 and 2; b) between cirrhotic patients and controls; c) within cirrhotic patients and controls between the 0-400 and 0-800 sec/mm2 b-values set.
Analysis a) and b) was performed also for the f value.
Paired- or unpaired t-test were used accordingly.
Statistical significance was assumed for a p less than 0.01.