Type:
Educational Exhibit
Keywords:
Abdomen, Pancreas, Oncology, CT, Neoplasia
Authors:
C. Caraiani1, A. Lebovici2, O. S. M. Isse2; 1Cluj-Napola/RO, 2Cluj-Napoca/RO
DOI:
10.1594/ecr2011/C-2001
Imaging findings OR Procedure details
CT was performed using a 16 slice scanner (Siemens Somatom Emotion 16,
Erlangen,
Germany).
Patients were asked to drink 1000 ml of water 30-45 minutes before the procedure.
The abdominal scan was done in the late arterial phase and in the portal venous phase.
We used bolus tracking at 120 UH and a delay of 15 seconds for the late arterial phase.
The injection rate was at 3-3,5ml/second.
We used thin-section scanning and MPR and MIP reconstructions to better deliniate vascular anatomy.
We considered vascular invasion and sign of inoperability if any of the following was invaded: the celiac trunk,
the mesenteric artery,
the hepatic artery,
the splenomesenteric confluence.
We also regarded as vascular invasion portal and superior mesenteric vein involvement on a distance longer than 1cm.
Venous occlusion of the portal and superior mesenteric vein was also seen as a sign of inoperability.
Patients with suspicion of venous invasion on a short distance,
in the absence of other surgical contraindications,
underwent surgical exploration and,
eventually,
benefited from vascular reconstructions.
The invasion of the splenic vein,
the splenic artery and the gastroduodenal artery were not considered as signs of inoperability.
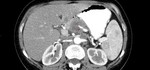
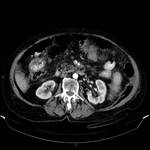
We considered as signs of vascular invasion:
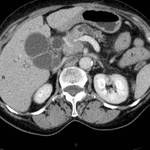
- arterial stenosis (arteries with diminished caliper or irregular margins- Figure 1)
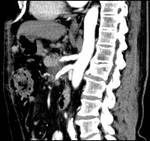
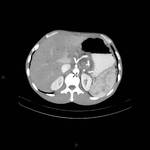
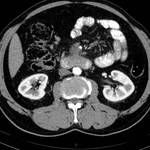
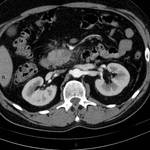
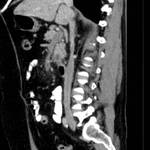
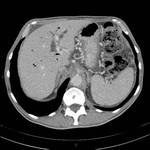
- vessels embedded in tumor or in contact with the tumor on more than 50% of their caliper (Figure 2,
Figure 3,
Figure 4)
- the so called "perivascular cuff"- arteries embedded in tumoral tissue at a distance from the tumor.
All cases in our series with this aspect had vascular invasion at surgical examination.
The aspect can be explained by periarterial lymphatic invasion (Figure 5)
- "periarterial streaks"- fine reticular opacities between the tumor and the vessels with no contact between the vessel and the tumor.
In our series we had no patient with this sign as the only sign of unoperability.
Valls and co reported 8 cases,
2 of them being proven at surgery as being unresectable.
This aspect can reflect either tumor invasion or a peritumoral desmoplastic reaction (Figure 6)
- venous occlusions (Figure 7).
Sometimes the presence of dilated collateral vessels signalates the presence of an occluded vein (Figure 8)
- venous stenosis.
Veins with diminished caliper or irregular margins.
The stenosis of the spleno-mesenteric confluence was considered a sign of unoperability.
Stenosis of mesenteric vein or portal vein on a distance longer than 10-15mm was considered sign of unoperability because of the poor prognosis of this patients,
even after vascular reconstruction procedures (Figure 9).
Stenosis and even occlusion of the splenic vein was not considered as a criteria for unresecability
- contact between veins and tumoral tissue.
Veins have no muscular wall,
so invasion occurs easier than for arteries.
Li and all report in their series that 43% of patients with tumoral contact on less than 50% of the circumference of the vein have venous invasion at surgery.
We considered operability/inoperability criteria the same as for venous stenosis.
- "tear-shaped superior mesenteric vein".
We had two patients with tear-shaped superior mesenteric vein in our series,
both considered being unresectable do to signs of arterial invasion.
We had no patients with tear-shaped superior mesenteric vein as the only sign of unresectability.
Hough reports 13 patients with tear-shaped superior mesenteric vein,
all of them with unresectable tumors.
Despite that,
we consider that if only a tear-shaped superior mesenteric vein is seen on CT,
the patient should not be considered as unelegible for pancreatic surgery
In our series,
based on 141 patients with pancreatic carcinoma,
42 of them with tumors considered resectable after CT scanning we had a positive predictive value for unresecability of 100% (no one of the tumors that we described as unresectable and underwent palleative surgery were proven to have,
in fact,
a resectable tumor) and a negative predictive value for unresectability of 91,5% (four patients were proven intraoperatively to have unresectable tumors and we described preoperatively a resectable tumor.
Carcinomatous peritoneal deposits was the reason in two cases and underestimation of venous invasion in the other two).