Patient selection:
Patients with severe aortic valve stenosis and high surgical risk were reviewed on a monographic consultation.
Final treatment decision was based on a multidisciplinary session with cardiac surgeons and interventional and clinic cardiologists.
Preprocedural transthoracic echocardiography,
cardiac catheterization (coronariography and hemodynamic valve study) and MDCTA were performed in all patients.
From November - 2008 until July – 2010,
71 MDCTA were performed on patients that were candidate to percutaneous aortic valve replacement.
We have assessed:
- Aortic root (Fig 3):
- Valsalva coronary sinus measurement.
- Sinotubular junction measurement.
- Distance from valve ring to coronary arteries.
- Aortic valve calcifications presence and grade.
-
Ascending thoracic aorta,
aortic arch and descending thoracic aorta measurement.
Presence and grade of aortic calcification.
-
Abdominal aorta measurement,
as well as aortic tortuosity and presence and type of calcifications (circumferential,
peripheral,
porcelain aorta,
etc.).
-
Iliac and femoral artery measurement.
Ilio-femoral axis tortuosity and presence/type of calcifications (circumferential or peripheral) evaluation.
-
Unknown disease that would contraindicate percutaneous valve replacement was confirmed or discarded.
Principal techniques to evaluate aortic root before percutaneous aortic valve replacement are transthoracic echocardiography (TTE) and transesophageal echocardiography (TEE).
Accurate metering of valve ring is necessary to determinate adequate device selection.
There are two available stent sizes,
ensuring valve stability and minimizing para-aortic regurgitation scope.
In general,
23mm.
prosthesis is appropriate for an aortic ring between 18 and 22 mm.
in diameter and 26mm device is adequate for 21-26 mm.
aortic roots.
When a discrepancy exits between TTE and TEE,
the MDCTA measurement will be definitive.
MDCTA Technique:
Computer Tomography studies were performed using a 64-slice MDCT (GE Light Speed VCT),
0.625 x 64 mm.
collimation,
500 msec rotation time,
tube current of 300-600 mA and 120 kVp.
In cases with body mass index under 25,
we used 100 kVp.
Studies were performed without cardiac synchronism and without beta-blockers administration,
due to elderly patients.
Image acquisition started at thoracic entry until lesser trochanter to ensure detailed evaluation from aortic root until femoral arteries.
We have used 100 cc.
of non-ionic contrast administration at 300 mg/ml concentration (Ultravist 300mg/mL.
Bayer) with a posterior 40 cc.
physiological saline bolus,
in both cases with a 4ml/s flow rate.
Antecubital vein and two-way automatic injector was used for contrast administration.
Images were acquired during arterial enhancement phase,
using “bolus-tracking” automatized technique (“Smart-Prep”),
with automatic detection of peak enhancement at ascending aorta.
All axial data acquired were sent to a Workstation (Advantage Windows 4.4,
GE Healthcare) for study and review.
A combination of multiplanar reformat,
MIP and volume rendering were used to evaluate aorta and aortic-iliac-bifemoral axis.
Aortic valve calcifications were classified in: (Fig.4.)
Grade 1: No calcification.
Grade 2: Light calcification.
Grade 3: Moderate calcification.
Grade 4: Extensive calcification
Root measurements are taken in two orthogonal planes,
due to its elliptical form (both healthy and aortic stenosis patients).
The same is done with Valsalva sinus and sinotubular junction diameters (Fig.
5).
Distance from valve ring to coronary arteries ostium is also measured (Fig.
6),
because it’s been described cases of coronary occlusion due to native valve displacement during procedure.
Thoracic (Fig.
7) and abdominal aorta measurements were obtained on its minimal luminal diameter,
measured on images with the double oblique tool,
orthogonal to the medium vessel line.
A diameter over 4 cm.
in thoracic aorta and over 3 cm.
in abdominal aorta was considered as aortic aneurysm (Fig.
8).
Presence and type of calcifications were also evaluated ( Fig.9 ).
The presence of peripheral arterial arteriosclerotic disease limits transfemoral access.
Valve prosthesis catheter Edwards 22F needs a common femoral diameter between 7-8 mm.
and the 24F,
8mm.
at least. If arterial diameter is insufficient or an extensive calcification or tortuosity of the ilio-femoral axis is present,
transfemoral approach is associated with high risk of arterial lesion.
In these cases,
transapical approach may be indicated.
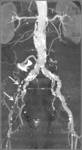
MDCTA allows permeability (Fig.
10) and diameter assessment of the ilio-femoral axis (Fig.
11 and Fig.
12).
Arteries were measured on its minimal luminal diameter,
using doble oblique tool,
and window level were adjusted to reduce the blooming effect produced by peripheral calcifications.
With MDCTA we can also assess aorto-ilio-femoral axis tortuosity and presence of calcifications (Fig 13).
Circumferential calcifications on abdominal aorta and aorto-iliac axis are considered of relative procedural contraindication (Fig 14 y Fig.
15).
Porcelain abdominal aorta (Fig.
9) is considered an absolute transfemoral approach contraindication.